Calcium's Sex-Specific IGF-1 Effect: Why the Same Supplement Raises One Child's Growth Hormone and Lowers Another's
The Surprising Hormonal Divergence Behind a Common Mineral Supplement
You might think popping a calcium supplement is a simple choice—something you, your kids, or your parents can all do the same way.
But the latest research turns that idea upside down. The same daily dose of calcium can send one child’s growth hormone up, while driving another’s down. This isn’t just about bones. Calcium’s effects reach deep into your hormones, inflammation, and even your immune system, and how your body reacts depends on factors as personal as your age, your sex, and your unique biology.
- IGF-1
- Insulin-like growth factor 1, a marker of growth hormone axis activity. Low levels indicate GH deficiency, high values suggest acromegaly or active growth.
- IGF-1 (Insulin-like Growth Factor 1)
- A hormone that plays a key role in growth and development in children and adults. In this article, it's the main biomarker showing opposite responses to calcium in boys and girls.
- Sex-specific effects
- When the same treatment or supplement produces different results in males versus females, as seen with calcium's opposite effects on IGF-1.
- Randomized controlled trial (RCT)
- A high-quality study design used to test the effects of treatments or supplements. The key findings here come from RCTs.
- Calcium
- Total serum calcium, essential for bone health, muscle contraction, and nerve signaling. low levels cause muscle cramps and osteoporosis risk, while high values may indicate parathyroid disorders.
- Short-chain fatty acids (SCFAs)
- Beneficial compounds produced by gut bacteria when they break down fiber and some minerals, including calcium. SCFAs may mediate some of calcium's metabolic effects.
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- acetate
- A short-chain fatty acid that plays a key role in cellular energy metabolism.
- carbonate
- A chemical compound often combined with calcium to create dietary bone supplements.
- CRP
- C-reactive protein is a common blood marker used to measure systemic inflammation.
Picture yourself at the kitchen table with your family, pouring out vitamins for the day. Maybe you’re adding a calcium chewable to your child’s breakfast plate, or reminding your partner to take theirs with coffee. It’s a normal, caring routine—one designed to protect bones, boost growth, or maybe just follow the advice you’ve heard for years. But what if, hidden beneath that simple act, your well-intentioned supplement is quietly pushing your child’s growth hormone in the wrong direction? What if the same pill helps your son but hinders your daughter, or vice versa?
That’s the unsettling question raised by new research showing that calcium’s effects are anything but one-size-fits-all. Most of us want the best for our families, but the truth is, your biology—not the bottle—determines what happens next. Whether you’re looking to support your own heart, your child’s height, or everyone’s immune system, it turns out that the way your body responds to calcium is as unique as your fingerprint.
So much of health advice is painted in broad strokes. Take one thousand milligrams of this. Aim for strong bones, prevent fractures, support growth. But real life isn’t that simple. The science is revealing a much more personal story—one where age, sex, and your own body’s signals matter more than any label or marketing claim. And that brings us to the real question: how do you make calcium work for you, not against you? Let’s unpack why this mineral is so important, how it acts differently in boys and girls, and what you actually need to know before you reach for that next supplement.
Calcium has always been sold as the universal bone builder. But the truth is, its reach goes far beyond your skeleton. Calcium is a key player in hormone signaling, immune response, metabolism, and even the way your body handles inflammation. And here’s the twist: the effects of calcium are deeply influenced by your sex and stage of life.
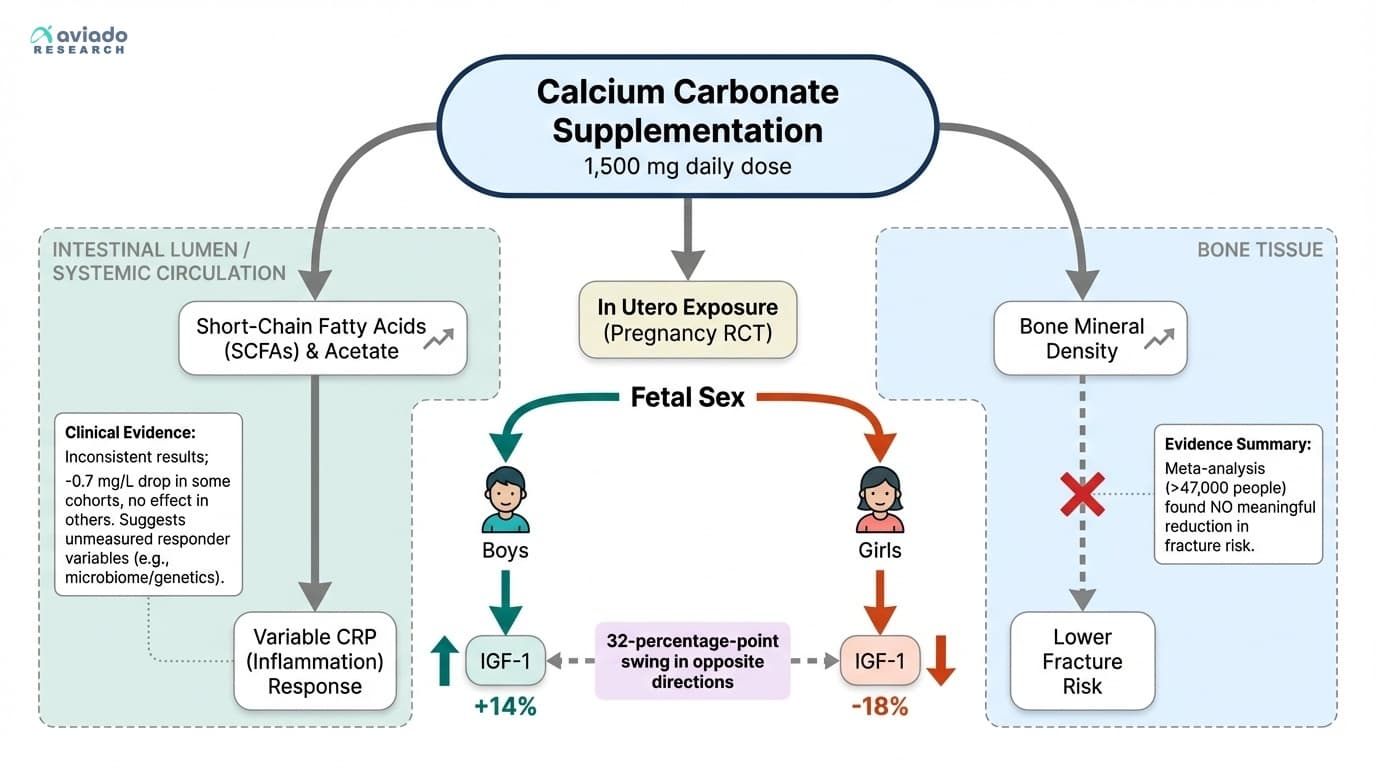
Let’s start with children. In a groundbreaking randomized trial out of Finland, researchers gave pregnant women fifteen hundred milligrams of calcium carbonate daily. When they looked at the children years later, they found something that flipped expectations on their head. Boys exposed to extra calcium in the womb had a fourteen percent rise in their IGF-1 levels after birth. IGF-1 is short for insulin-like growth factor one, a hormone that acts like a growth switch for bones, muscles, and metabolism. But here’s the kicker: girls in the same study had an eighteen percent drop in IGF-1 levels from the same calcium exposure. That’s not a small difference—it’s a complete reversal. The same mineral, the same dose, but two dramatically different hormonal outcomes just because of sex.
Why does this happen? It comes down to how male and female bodies regulate hormones during key growth periods. Boys are primed to respond to certain nutrients with increases in anabolic, or growth, signals—especially during childhood and puberty. Girls, who balance growth with complex hormonal cycles from a much earlier age, may interpret extra calcium as a cue to dial down certain growth signals, possibly as a way to protect bone health and energy balance differently. These differences are written deep into your biology, shaped by evolution and driven by how your body prioritizes growth, reproduction, and long-term survival.
And it doesn’t stop with children. In adults, especially women, the hormonal environment shifts again during life stages like pregnancy, perimenopause, and menopause. Estrogen, for example, helps your bones hold onto calcium, but when estrogen drops, your bones can start to lose more calcium, raising the risk for osteoporosis. For men, testosterone supports muscle and bone, but hormonal decline with age changes how your body uses calcium and IGF-1 as well.
What does all this mean for you? It means that the right dose for your body depends on where you are in life and who you are biologically. Calcium is not just about bones—it’s an active player in your hormonal orchestra, and it plays a different tune depending on your sex and age. That brings us to the next step: how can you measure what’s actually happening inside your body?
If you want to move beyond guesswork, you’ll need more than just a daily supplement. You’ll want to track how calcium is actually affecting your body. That starts with understanding the key biomarkers—measurable signals in your blood that reveal what’s happening beneath the surface.
The first marker to watch is IGF-1, or insulin-like growth factor one. This hormone is like your body’s growth dial. In children and teens, IGF-1 drives height, bone length, and muscle development. In adults, it supports tissue repair, muscle maintenance, and metabolism. Healthy IGF-1 levels depend on age and sex, but typical reference ranges are roughly one hundred to three hundred nanograms per milliliter in adults, with higher values in children and adolescents. If you’re supplementing calcium to support growth or muscle mass, IGF-1 is the marker you’ll want to track. A rise in IGF-1 means your body is responding with more growth signaling; a drop could mean the opposite.
For inflammation, the key marker is CRP, or C-reactive protein. This protein rises when your body is fighting inflammation or infection. Normal CRP should be below one milligram per liter in healthy adults. Some studies have shown that calcium supplementation can lower CRP, suggesting a reduction in inflammation, while others found no effect at all. The difference likely comes down to personal biology—your genetics, your gut microbiome, and your baseline health status. If you’re aiming to use calcium for inflammation or immune support, tracking CRP before and after a few months of supplementation will tell you whether it’s working for you.
If you’re concerned about bone health, the classic markers are bone mineral density (BMD) and, sometimes, markers like osteocalcin or bone-specific alkaline phosphatase. But here’s what the latest science reveals: an increase in BMD from calcium supplements does not always translate into fewer bone fractures. So while it’s useful to know your bone density, don’t assume that a higher number automatically means stronger, unbreakable bones.
Finally, if you want to know how your gut is responding, you can look at short-chain fatty acids (SCFAs) in stool tests, especially acetate and butyrate. These are produced by your gut bacteria when you digest fiber and, interestingly, their levels can rise with calcium supplementation in some people. Higher SCFAs are linked to better metabolic and immune health, but again, your response is unique.
What’s the big takeaway? Blood tests for IGF-1 and CRP, bone density scans, and even gut health panels can all help you see how your body is reacting to calcium. Testing before and after trying a supplement gives you real data—no more guessing, just personalized feedback. Now, let’s talk about how to actually use calcium wisely.
When it comes to calcium supplements, more is not always better. The evidence shows that the effects of calcium depend not only on how much you take, but also on how your body processes it, your age, and your biological sex.
Most clinical trials use between one thousand and fifteen hundred milligrams of calcium carbonate daily, often split into two doses. In the Finnish trial that discovered the sex-specific IGF-1 effect, pregnant women took fifteen hundred milligrams per day, which caused a fourteen percent rise in IGF-1 for boys but an eighteen percent drop for girls. If you’re starting calcium for yourself or your child, a common evidence-based protocol is five hundred milligrams twice daily—morning and night—rather than a single large dose. This helps your body absorb calcium more efficiently and reduces the risk of side effects like constipation or kidney stones.
But dose is just the start. The form of calcium also matters. Calcium carbonate is cheap and widely available, but it needs stomach acid to be absorbed well. If you have low stomach acid or take acid-blocking medications, you may absorb less. Calcium citrate is a good alternative, especially for older adults or people with digestive issues, because it’s better absorbed regardless of stomach acid. Aim to take calcium with food, as this boosts absorption and minimizes stomach upset.
What about timing with other supplements? Calcium can interfere with the absorption of certain minerals, especially iron and magnesium, if taken at the same time. Space calcium supplements at least two hours apart from iron or magnesium for best results. If you’re taking vitamin D, know that it helps your body absorb and use calcium more effectively. Most adults need at least six hundred to eight hundred international units of vitamin D daily, and people with low sunlight exposure may need more.
For children, especially those with rapid growth or dietary restrictions, the lower end of dosing—five hundred to one thousand milligrams daily—is usually safest. But remember, the response can be completely different for boys and girls. That’s why tracking IGF-1 and growth after a few months is so important. For adults, especially women after menopause or men over age fifty, the standard total intake from diet plus supplements should not exceed two thousand milligrams daily to avoid risks of kidney stones or vascular calcification.
And finally, think about your diet. Calcium from food—like dairy, leafy greens, or fortified plant milks—is often better absorbed and less likely to cause side effects. Food-based calcium also comes with other nutrients that help your body use it well. Supplements should be used to fill gaps, not as your only source. So what about other ways to support your body alongside or instead of calcium? Let’s look at the lifestyle levers you can pull.
Supplements can help, but they’re just one piece of the puzzle. Your lifestyle—how you move, sleep, and eat—plays an even bigger role in how your body handles calcium, builds bone, and manages hormones like IGF-1.
Start with movement. Weight-bearing exercise is the most powerful natural builder of bone density. Activities like walking, running, dancing, and resistance training send signals to your bones and muscles to grow stronger. For children and teens, at least one hour of active play or sports each day sets the foundation for lifelong bone health. For adults, especially women after menopause and men over fifty, aim for at least one hundred fifty minutes of moderate weight-bearing exercise each week. This not only helps bones but also boosts IGF-1, improves balance, and lowers inflammation.
Sleep is another hidden lever. Your body repairs and grows bone tissue mostly at night, during deep sleep. Poor sleep disrupts growth hormone and IGF-1 cycles, making it harder for your body to use calcium efficiently. Children and teens need eight to ten hours of sleep per night, while adults should aim for at least seven. If you’re supplementing calcium for growth or repair, getting enough restorative sleep is crucial to seeing benefits.
Now let’s talk food. Calcium-rich foods—like dairy products, tofu, sardines, almonds, leafy greens, and fortified plant milks—not only provide calcium but also deliver magnesium, potassium, and vitamin K, all of which help your body use calcium properly. Pairing calcium-rich foods with sources of vitamin D, like eggs or fatty fish, further boosts absorption. For people with lactose intolerance or vegan diets, plant-based milks and leafy greens can cover most of your needs, but check labels for added calcium and vitamin D.
The gut microbiome also matters. Your gut bacteria help break down fibers into short-chain fatty acids, which have been shown to increase in some people taking calcium supplements. These fatty acids support immune health, reduce inflammation, and may even help your body use calcium more efficiently. Eating a diverse range of plant foods—fruits, vegetables, whole grains, and legumes—nourishes your microbiome and amplifies the benefits of any calcium you take.
And finally, watch out for excess salt and soda. High salt intake can cause your body to lose more calcium in urine, while too much soda—especially colas—can interfere with calcium absorption. Moderation is key. By moving your body, prioritizing sleep, and eating a diet rich in whole foods, you set the stage for calcium to work in your favor. But how do you know if things are going off track? That’s what we’ll cover next.
It’s easy to assume that more calcium is always better, but your body will often give you signals if things aren’t right. Paying attention to these early warning signs can help you catch problems before they become bigger issues—whether you’re supplementing for yourself or your family.
In children, the most important signals are changes in growth rate, energy, and mood. If your child is taking calcium and you notice slower-than-expected growth, unusual fatigue, constipation, or stomach pain, it’s time to check in with your healthcare provider. These could be signs that calcium is affecting hormone levels—like IGF-1—or causing digestive upset. Boys and girls may respond differently, so if your son seems to be growing faster or your daughter’s growth slows down, testing IGF-1 can provide clarity.
For adults, particularly women after menopause and men over fifty, new muscle weakness, frequent muscle cramps, or bone pain may mean your calcium or vitamin D intake needs adjusting. On the flip side, too much calcium—especially from supplements—can cause kidney stones, constipation, or even abnormal heart rhythms in rare cases. If you experience these symptoms, stop supplementation and seek medical advice.
Other subtle red flags include unexplained joint pain, persistent low energy, or trouble sleeping. These can all be linked to how calcium affects inflammation and hormone balance. Testing CRP for inflammation, checking kidney function, and monitoring blood calcium levels can help you determine if your supplement routine needs a tweak.
Finally, if you or your child develops a new intolerance to calcium-rich foods, or if you notice changes in digestion after starting a supplement, consider switching to a different form (like calcium citrate) or increasing food-based calcium instead. If you have a family history of kidney stones or heart disease, be extra cautious with high-dose supplements and make sure to monitor your blood work regularly.
The key message is that your body will often tell you when something’s off. Tune in to these signals, respond early, and use testing to guide your next steps. That leads us to the bottom line—how to make calcium work for you, not against you.
Calcium’s story is more complex than any supplement bottle suggests. The same dose, in the same family, can help one person and hinder another. Boys and girls, men and women, each have unique needs shaped by biology, hormones, and life stage. IGF-1, CRP, and bone density are not just abstract numbers—they’re real signals that tell you whether your body is thriving or struggling with your current calcium routine.
The latest science says this clearly: universal dosing is out, personalization is in. Start with a food-first approach, using supplements to fill in gaps. Track your response with simple blood tests for IGF-1 and CRP, and adjust your dose based on how you feel and what you see in your results. For children, remember that growth patterns and hormonal responses can diverge dramatically by sex. For adults, especially as you age or move through life’s hormonal milestones, your calcium needs shift—and so does your risk for side effects.
Leverage lifestyle—exercise, sleep, a diverse diet—to amplify the benefits of any calcium you take. And above all, listen to your body’s early warning signs. If something feels off, don’t wait. Testing and a quick conversation with your healthcare provider can put you back on track.
In the end, calcium is not just a mineral for your bones. It’s a signal—one that interacts with your hormones, your immune system, and your unique biology every single day. When you tune in, personalize, and track, you unlock the real potential of this essential nutrient. Your health is personal. So should your calcium strategy be.
Calcium's Sex-Specific IGF-1 Effect: Why the Same Supplement Raises One Child's Growth Hormone and Lowers Another's
The Surprising Hormonal Divergence Behind a Common Mineral Supplement
Diagram glossary
- acetate:
- A short-chain fatty acid that plays a key role in cellular energy metabolism.
- carbonate:
- A chemical compound often combined with calcium to create dietary bone supplements.
- CRP:
- C-reactive protein is a common blood marker used to measure systemic inflammation.
- IGF-1:
- A crucial growth hormone that regulates childhood development and influences lifelong metabolism.
- SCFA:
- Short-chain fatty acids are microbial metabolites that provide energy and support gut health.
Conclusions
Calcium is far more than a basic mineral for bones—it’s a powerful, individualized signal for growth, metabolism, and inflammation. The same dose can help one person and hinder another, especially between boys and girls. Generic supplementation advice misses these crucial differences. The best approach is to personalize your calcium intake, track key markers like IGF-1 and CRP, and adjust your dose based on your unique biology.
Most studies on calcium's sex-specific effects are limited to pregnancy and early childhood, so it’s unclear how these findings apply to older children or adults. Many trials combine calcium with vitamin D, making it hard to isolate pure calcium effects. There is still little data on long-term impacts of sex-specific IGF-1 changes, and individual responses may depend on genetics, diet, and gut microbiome—factors not always measured in studies.
Track this in your stack
See how calcium relates to your health goals and monitor changes in your biomarkers over time.
