GABA Supplements Can't Cross the Blood-Brain Barrier — So Why Do Some People Swear By Them?
The surprising peripheral mechanisms that explain why oral GABA works for some but not others
You might reach for a GABA supplement on a stressful day, hoping for calm or better sleep.
But here’s the twist — most of the GABA in that capsule never actually enters your brain. Yet, plenty of people swear by these supplements. What’s going on? The real story is more interesting and more relevant to your gut, your heart, and your nervous system than you might expect.
- GABA-enriched foods
- Foods or drinks processed to raise GABA content (often via fermentation), such as some teas and dairy products.
- GABA (gamma-aminobutyric acid)
- A calming messenger in the nervous system. Your brain uses it to reduce “overfiring.”
- GABA
- The brain's primary inhibitory neurotransmitter, promoting calm and relaxation. Low levels linked to anxiety and sleep problems.
- Triglycerides
- Triglycerides, the primary fat storage molecule in blood. elevated levels indicate metabolic dysfunction and increase cardiovascular risk.
- Blood-brain barrier (BBB)
- A tight filter around the brain that blocks many molecules in blood. Most oral GABA does not pass through it.
- Peripheral GABA receptors
- GABA “docking sites” outside the brain, especially in the gut and blood vessels. They can change body signals linked to stress.
- Food-matrix delivery
- How a compound acts when eaten in food versus a pill. Food can change absorption and effects.
- BBB
- A protective membrane that blocks most orally consumed GABA from entering the brain.
Imagine coming home after a long, noisy day. Maybe your mind is still spinning as you try to wind down for the evening. You’ve heard friends talk about GABA — that supplement promising calm, better sleep, or less anxiety. You pick up a bottle, read the label, and wonder: will this actually help me relax? You take your first dose before bed, hoping for quiet in your mind or relief from the tension in your chest. If you wake up feeling better, was it the supplement? Or something else?
That search for calm is universal. Whether you’re dealing with work stress, family chaos, or just the hustle of modern life, you want something that works. GABA is everywhere now. It’s in capsules, in calming teas, even in fancy chocolate bars at the grocery store. But here’s the surprise: the science says that most of the GABA you swallow never actually makes it into your brain. That seems hard to believe, especially when you read reviews from people who swear it changed their lives.
This is where things get interesting. The story of GABA — how it affects your body, your gut, and your mind — is not what most supplement ads would have you believe. But it’s also not a simple case of “it doesn’t work.” The real science is much more fascinating, and it opens up new ways to think about your stress, your digestion, and even your heart health. Let’s unpack why GABA supplements are so confusing, and what you can actually expect from them.
GABA, or gamma-aminobutyric acid, is your body’s primary inhibitory neurotransmitter. Think of it as your internal brakes. When neurons are firing too rapidly — whether from anxiety, excitement, or just a busy day — GABA steps in to quiet things down. In your brain, GABA keeps you from feeling overwhelmed, helps you fall asleep, and even protects against overstimulation.
But GABA doesn’t just matter upstairs. Your gut is packed with GABA receptors, too. In fact, your digestive tract produces and responds to GABA almost like a second brain. This is why researchers call it the “gut-brain axis.” When GABA is active in your gut, it can send calming signals to your brain through the vagus nerve, the main communication highway between your belly and your mind.
Here’s where it gets even more interesting. GABA is also active outside your nervous system. Your heart, your blood vessels, and even your liver and kidneys respond to GABA. For example, GABA can help lower blood pressure by relaxing blood vessel walls. In your immune system, it helps control inflammation. So when you swallow a GABA supplement, you’re not just targeting your brain. You’re activating a whole network of body systems that influence everything from stress levels to cardiovascular health.
The catch? For a supplement to impact your brain directly, it has to cross the blood-brain barrier. That’s the security system that protects your brain from unwanted chemicals. Unfortunately, GABA is a big, water-loving molecule. Your blood-brain barrier is very selective, and it lets almost none of orally consumed GABA through. That makes GABA different from other calming supplements, like magnesium or certain herbs, which can cross more easily.
So why do some people feel benefits from GABA supplements at all? The answer points to the fascinating, underappreciated power of your gut and body to influence your mind through indirect pathways. We’ll dig into exactly how that works next.
If you want to know whether GABA is really affecting your health, you need to look beyond just how you feel after a dose. There are several biomarkers that can help you understand what’s happening in your body and what you might want to track if you’re experimenting with GABA, whether for stress, sleep, or cardiovascular support.
First, let’s talk about fasting triglycerides. This is a blood fat that’s often checked as part of a routine cholesterol panel. Some research — for example, a six-week randomized trial using GABA-enriched cheese — found that daily GABA intake could raise fasting triglycerides by about ten percent. For most people, that’s not a crisis, but if you already have high triglycerides or you’re at risk for metabolic syndrome or cardiovascular disease, it’s worth paying attention. The takeaway is that GABA supplements or foods can affect your blood lipids, so you’ll want to track this if you decide to take them regularly.
Next, consider heart rate variability, or HRV. This is a measure you can track with many wearables, and it reflects how well your nervous system can shift between stress and relaxation states. Because GABA can activate calming pathways in your body, some people see improvements in HRV when they use GABA supplements, especially before bed. If you’re using GABA for sleep or stress reduction, tracking HRV can help you see if your protocol is having a measurable effect.
Sleep quality is another practical marker. You can monitor how quickly you fall asleep, your total sleep time, and how often you wake up during the night. If you’re using GABA for sleep, give it at least a week and track these outcomes. If there’s no change, you might be among the many people who do not respond to oral GABA.
Finally, if you’re using GABA-enriched foods or supplements daily, it’s smart to check for side effects like digestive upset, headaches, or changes in mood. Most people tolerate GABA well, but a small number find that it can make them feel flat or even slightly down.
So what does it mean for you? Take a baseline measurement of your triglycerides and HRV if you plan to use GABA regularly. Track your sleep for a week before and a week after starting. If you see no change in how you feel and no change in these objective markers after two weeks, it’s likely that oral GABA is not doing much for you. That brings us to the question of how to actually use GABA — and how to maximize your odds of feeling a benefit.
If you’re considering trying GABA, start with a clear plan. The science says that response to oral GABA is highly individual, so you’ll need to experiment and measure.
A good starting dose is one hundred to two hundred milligrams once daily. Take this dose for three days, ideally at a time when you’re looking to relax, such as in the evening before bed. If you tolerate this well, you can try increasing to three hundred milligrams, taken thirty to sixty minutes before bedtime, for one week. Some studies have used doses as high as seven hundred fifty milligrams per day in divided doses, but higher is not always better. Because most of the GABA will not cross into your brain, increasing the dose often just increases the risk of side effects without adding benefit.
Track your response. Use a sleep tracker or journal to note how quickly you fall asleep, how refreshed you feel in the morning, and whether your overall stress levels seem to change. If you’re using GABA for cardiovascular support — for example, to help lower blood pressure — track your blood pressure readings and fasting triglycerides before you start and again after six weeks of daily use.
Here’s the key mechanism: when you swallow GABA, it binds to receptors in your gut and other peripheral tissues. This can influence your vagus nerve, which then sends signals up to your brain that help induce calm or relaxation. Some people have more sensitive GABA receptors or a more responsive vagus nerve, so they feel more benefit. Others notice nothing at all. If you feel no difference after two weeks at three hundred milligrams before bed, you may be a non-responder and it’s reasonable to stop.
If you prefer a food-based approach, you can try GABA-enriched teas or fermented foods. These products are often marketed as stress relievers or blood pressure support. Just remember that fermented foods contain a range of active compounds, so any benefit you feel may not be from GABA alone. And, as the cheese study showed, some GABA-rich foods can impact your blood lipids.
In summary, start with a low dose, increase gradually if needed, and measure both subjective and objective outcomes. If you find a protocol that works for you, stick with it, but retest your fasting triglycerides and check in with your health metrics after six weeks. If you do not see or feel a change, you can move on to other strategies for stress and sleep.
Even if oral GABA does not make a difference for you, there are powerful evidence-based ways to increase your body’s natural GABA activity — and these approaches often come with benefits for your brain, gut, and heart at the same time.
Exercise is one of the most reliable ways to boost natural GABA levels within your brain. Thirty minutes of moderate aerobic activity, like brisk walking or cycling, increases GABA activity and helps quiet neural overactivity. Resistance training and high-intensity interval training do this as well. The mechanism? Exercise increases the expression of enzymes involved in GABA synthesis in both your brain and peripheral tissues. This means your body can make more of its own calming neurotransmitter, with the added bonus of improving cardiovascular health and lowering blood pressure.
Nutrition matters, too. Magnesium, found in leafy greens, beans, nuts, and seeds, is a key cofactor for GABA production. Low magnesium can make it harder for your brain to use GABA efficiently, leaving you more prone to anxiety and sleep problems. A diet rich in magnesium supports your natural calming systems. B vitamins, especially B6, also play a role in helping your body convert glutamate (an excitatory neurotransmitter) into GABA. Foods like chickpeas, bananas, and salmon are excellent sources.
Sleep hygiene is crucial if you want to harness your natural GABA system. GABA is released in higher amounts during deep sleep, helping you stay asleep and wake up feeling restored. Create a wind-down routine, keep your room cool and dark, and avoid caffeine in the afternoon. If you struggle with sleep despite good habits, it may be worth exploring other causes, such as sleep apnea or high evening stress, rather than relying solely on supplements.
Gut health can also influence your body’s GABA system. Fermented foods like yogurt, kefir, and kimchi contain bacteria that support a healthy gut microbiome. Some gut bacteria can actually produce GABA, which may then signal through the gut-brain axis to influence your mood and stress levels. The more diverse and healthy your gut flora, the more robust your natural gut-brain signaling will be.
So while a capsule of GABA may or may not bring you calm, your lifestyle choices are guaranteed to make a difference. These levers — exercise, nutrition, sleep, and gut health — all work by supporting the body’s own GABA system, rather than trying to import it from outside.
You might wonder: how do I know if my body’s GABA system is out of balance? The signs are often subtle, but knowing what to look for can help you act early.
If you notice that your stress levels are persistently high, and simple things that used to roll off your back now leave you feeling tense or irritable, that may be a sign of low GABA activity. Trouble falling asleep, or waking up in the early hours with your mind racing, is another common clue. Some people notice muscle tension, a racing heart, or even mild digestive upset, especially under stress. These physical symptoms can be the body’s way of signaling that the brakes are not working as smoothly as they should.
If you are using GABA supplements and you start to feel unusually flat, down, or sedated, that’s a sign to back off or stop altogether. Rarely, people notice headaches or digestive discomfort after starting GABA or GABA-rich foods. If you have a history of depression, epilepsy, or are taking medications that influence the GABA system — such as benzodiazepines or certain anti-seizure drugs — always check with your healthcare provider before starting a supplement. GABA supplements are generally safe for most healthy adults, but they are not risk-free for everyone.
Pay special attention if you notice changes in your sleep, mood, or cardiovascular health that seem linked to starting or stopping GABA. If your fasting triglycerides go up significantly after six weeks of daily GABA use, that’s a sign to reconsider your protocol, especially if you have other risk factors for heart disease.
The bottom line is that your body will usually give you clues. Notice patterns in how you feel, how you sleep, and how your heart and digestion behave. If something feels off or dramatically different, it’s worth pausing to reassess. That brings us to the big picture — what does all this mean for your health moving forward?
GABA supplements are a perfect example of how a simple story can get complicated the closer you look. Swallowing GABA does not mean your brain gets a direct dose of calm. The blood-brain barrier is a real obstacle, and most orally consumed GABA never reaches your neurons. But that does not mean the supplement is useless. For some people, GABA acts through the gut-brain axis and peripheral receptors to trigger genuine feelings of relaxation, better sleep, or lower blood pressure.
The science tells us this effect is highly individual. Some people have a sensitive vagus nerve and robust gut signaling, so they feel a difference. Others do not. The only way to know is to try a measured, time-limited protocol, track your biomarkers and symptoms, and be ready to move on if you do not see benefits. Start low, increase slowly, and check your fasting triglycerides and sleep metrics after a few weeks.
If you do not respond to oral GABA, do not be discouraged. The best ways to strengthen your body’s natural GABA system are through lifestyle — regular exercise, a magnesium-rich diet, good sleep hygiene, and nurturing your gut microbiome. These interventions have the added benefit of supporting your brain, your heart, and your digestion, all at once.
In the end, the real lesson of GABA supplements is that your mind and body are deeply connected. Sometimes, working on your gut, your habits, and your sleep will have more impact than any single pill. If you want to experiment, do it with intention — and always listen to what your body is telling you. Knowing how to measure, track, and respond is your best tool for moving closer to calm, clarity, and health.
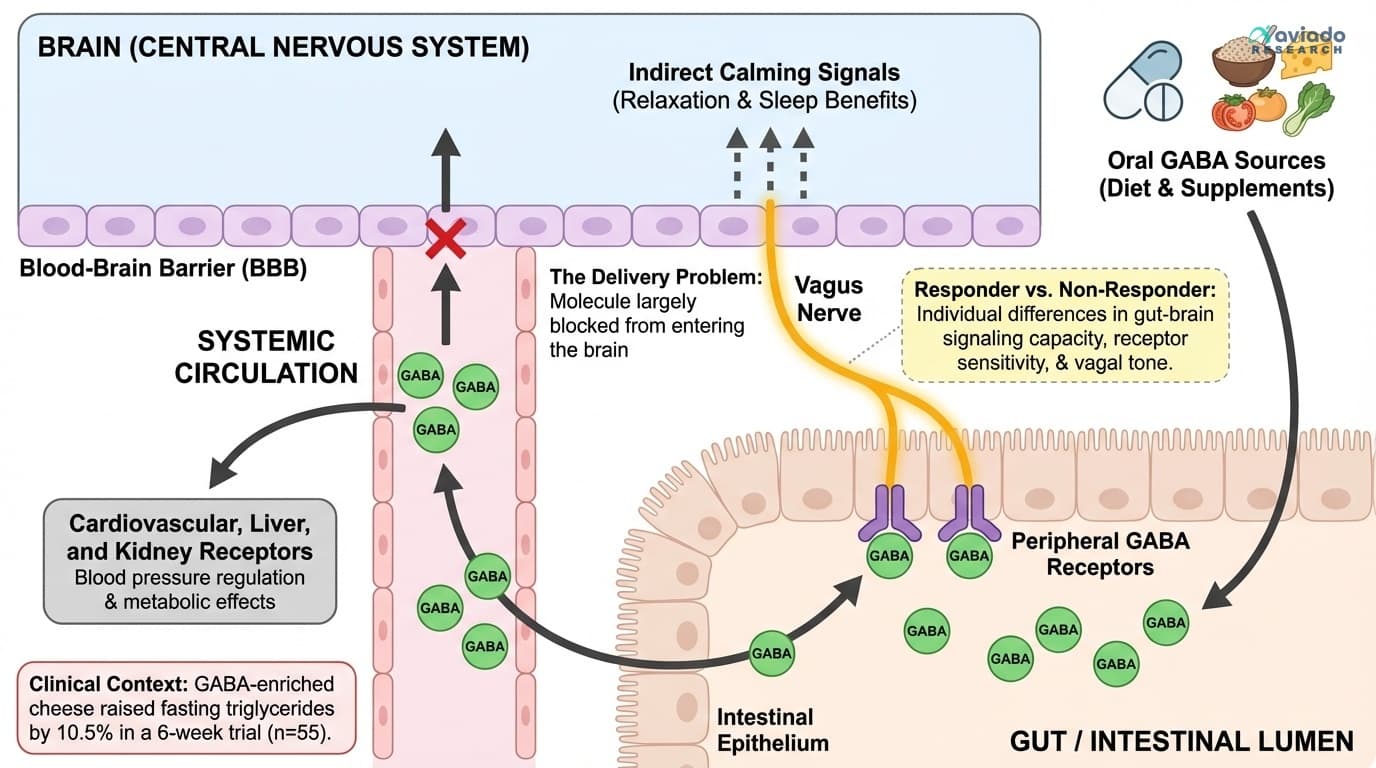
GABA Supplements Can't Cross the Blood-Brain Barrier — So Why Do Some People Swear By Them?
The surprising peripheral mechanisms that explain why oral GABA works for some but not others
Diagram glossary
- BBB:
- A protective membrane that blocks most orally consumed GABA from entering the brain.
- GABA:
- The primary inhibitory neurotransmitter responsible for reducing neural excitability and promoting calm states.
Conclusions
Oral GABA usually does not enter the brain in large amounts. If it helps you, it likely works through gut and body receptors that send signals to your brain. Because responses vary, you should treat GABA like a personal trial: use a clear dose plan, track sleep and HRV, and monitor triglycerides if you use GABA-enriched foods often.
Many studies are small and use short follow-up. Food-based GABA products may include other compounds that affect stress or sleep, so benefits may not be from GABA alone. Evidence on triglyceride changes comes from one 6-week crossover study and needs replication in other products and populations. Wearable sleep and HRV data can be noisy, so look for consistent trends over weeks, not single-night changes.
Track this in your stack
See how gaba relates to your health goals and monitor changes in your biomarkers over time.
