Your Second Brain: The Gut Revolution Every Young Man Needs
Why fixing your gut changes everything—from mood to hormones to performance
Surprising truth: Your gut contains more bacteria than human cells in your body. This hidden ecosystem controls your mood, energy, and stress response. Most young men have already lost 30-70% of their gut bacteria diversity from modern life.
This matters because your gut produces 90% of your serotonin and houses 70% of your immune system. When gut bacteria are imbalanced, you get brain fog, low energy, and chronic inflammation. Your body can't absorb nutrients properly even with a perfect diet.
You can rebuild your gut in 4-12 weeks. Take a multi-strain probiotic with 10-50 billion CFU daily. Add 30-40 grams of prebiotic fiber per day from diverse sources. Use L-glutamine at 5-10 grams daily to repair gut lining. Cut alcohol to under 4 drinks per week and avoid daily NSAIDs.
- CFU
- Colony-forming units. Measures the number of live bacteria in a probiotic supplement.
- IL-6
- A branded gut microbiome product family name used to identify a specific extract or formulation in research and supplement labels.
- Calprotectin
- A protein marker in stool that indicates gut inflammation. Normal levels are below 50 mcg/g.
- Dysbiosis
- An unhealthy imbalance or loss of gut bacteria diversity.
- NSAIDs
- Common painkillers like ibuprofen and naproxen that can damage the gut lining with frequent use.
- Prebiotic
- A type of fiber that feeds the good bacteria in your gut.
- Probiotic
- A supplement or food containing beneficial live bacteria that support gut health.
- BMI
- A measure of body fat based on an individual's weight and height.
- CRP
- A protein produced by the liver that indicates inflammation in the body.
- GABA
- An inhibitory neurotransmitter in the brain that promotes relaxation and reduces neuronal excitability.
- GALT
- Immune tissue in the digestive tract that protects the body from intestinal pathogens.
- GI-MAP
- A comprehensive stool test analyzing gut DNA to detect microbes and digestive markers.
Your gut isn’t just a digestive tube; it’s an ecosystem teeming with 38 trillion bacteria. These microbes outnumber your human cells and carry out essential functions every day. Think of your gut as your body's operating system—it's producing most of your serotonin, helping your immune system learn what to fight, making vitamins, and even sending messages straight to your brain through the vagus nerve. A landmark study published in Nature found that the diversity of your gut bacteria is a stronger predictor of overall health than traditional risk factors like BMI, blood pressure, or cholesterol [1]. Low diversity was directly linked to more inflammation, obesity, depression, and metabolic dysfunction.
For young men, this matters because your daily choices—from what you eat to how often you take antibiotics or painkillers—are shaping this ecosystem. Most young men have already lost a significant portion of their microbial diversity compared to non-industrialized populations [2]. Each round of antibiotics wipes out about 30% of your gut species, and many of these never come back [3]. This silent loss sets the stage for inflammation, poor mood, and sluggish metabolism.
Understanding your gut as your body’s control center changes how you approach health. Instead of chasing surface-level fixes, you start by rebuilding your foundation. In the next section, you’ll see how gut health drives your mind, immunity, and hormones.
Most health-conscious men in their 20s and 30s focus on muscles, testosterone, and maybe the occasional checkup. Gut health rarely makes the list. But your gut controls every major system you care about through direct biological pathways. The gut-brain axis uses 500 million neurons to send signals directly to your brain. When gut bacteria become imbalanced (dysbiosis), serotonin production drops by 40-60% and GABA synthesis is disrupted. A 2019 meta-analysis of 1,503 participants found that targeted probiotics reduced depression scores by 23% and anxiety by 18% in young adults [4].
Your gut houses 70% of your immune system through gut-associated lymphoid tissue (GALT). When your gut lining is damaged, bacterial toxins (LPS) leak into your bloodstream and trigger a 3-5x increase in inflammatory markers like IL-6 and TNF-alpha. This chronic inflammation reduces testosterone by 15-25%, slows muscle recovery, and creates the brain fog that derails your focus.
Gut health also controls nutrient absorption efficiency. Inflamed intestinal lining reduces B-vitamin absorption by 30-50% and cuts zinc uptake by 40%. If you keep finding low nutrient levels despite eating well, your gut is likely the bottleneck. Next, let's look at which biomarkers reveal your gut's actual status and how to track real progress.
To get serious about gut health, you need more than guesswork. Biomarkers give you a window into your gut’s actual status. The most comprehensive test is a stool analysis like the GI-MAP, which maps out your microbiome composition, flags any pathogens, checks for inflammatory markers (like calprotectin and lactoferrin), and evaluates digestive enzyme output and gut permeability. This test provides a full snapshot of your gut’s strengths and weaknesses.
Calprotectin is a key marker for gut inflammation. The standard healthy range is below 50 mcg/g. Anything above that suggests active inflammation, even if you feel fine. Calprotectin is especially helpful for telling the difference between irritable bowel syndrome (IBS) and more serious inflammatory bowel disease (IBD), and for tracking healing over time. Zonulin, measured in serum or stool, tells you about your gut barrier’s integrity. High zonulin levels mean your gut lining is letting unwanted substances leak through—a red flag for systemic inflammation.
Another important marker is hs-CRP, which measures overall inflammation in your body. If your hs-CRP is high and you don’t have an obvious reason (like an injury), it often points back to the gut. If you improve your gut and see your hs-CRP drop, that’s powerful confirmation of the gut-inflammation link. Finally, a stool short-chain fatty acid (SCFA) profile tells you if your beneficial bacteria are making enough butyrate, propionate, and acetate. Low levels mean your microbiome isn’t getting the fiber it needs. Food sensitivity panels (IgG/IgA) are more controversial but can highlight foods that trigger immune reactions in your gut when interpreted alongside symptom tracking.
Tracking these markers over weeks to months lets you see the impact of your interventions. Next, we’ll break down the core supplements and strategies that move these markers in the right direction.
Not all probiotics work the same way. To shift your gut health measurably, you need specific strains at therapeutic doses. Clinical trials show that multi-strain probiotics delivering 10-50 billion CFU daily can reduce IBS symptoms by 42% and improve mood scores by 15-25% within 8 weeks [4][6]. Focus on research-backed strains: Lactobacillus rhamnosus GG reduces anxiety and supports immune function, Bifidobacterium longum improves stress resilience and sleep quality, and Saccharomyces boulardii prevents antibiotic-associated diarrhea and supports gut barrier repair.
Strain specificity matters because different bacteria produce different metabolites. L. rhamnosus GG increases GABA production by 30%, while B. longum boosts brain-derived neurotrophic factor (BDNF) by 20%. Generic "Lactobacillus" products without strain identification rarely deliver these targeted benefits.
Rotate your probiotic brand every 2-3 months to maximize diversity. Your gut adapts to repeated strains, reducing their effectiveness over time. The biggest gains come when you combine probiotics with 30-40 grams of diverse prebiotic fiber daily, which helps new strains colonize and thrive. Up next, you'll learn how prebiotic fibers amplify these effects and drive measurable changes in gut diversity.
If probiotics are the seeds, prebiotic fiber is the fertilizer. Beneficial gut bacteria feed on diverse fibers to produce short-chain fatty acids (SCFAs) like butyrate, which fuels and protects your gut lining. Research from Stanford found that increasing the diversity of your dietary fiber boosted microbiome diversity more than any other single intervention [7]. This matters because a more diverse microbiome predicts better health outcomes across the board [1].
Aim for 30-40 grams of total fiber per day from a variety of sources. Key prebiotics include partially hydrolyzed guar gum (PHGG), acacia fiber, inulin, resistant starch (from cooked-and-cooled rice or potatoes), and psyllium husk. Each type feeds different bacteria, so mixing them creates broader benefits. Low fiber intake—common in the 18-39 male demographic—starves your beneficial bacteria and reduces SCFA production, weakening your gut barrier.
You can see changes in your SCFA profile and microbiome diversity within a few weeks of increasing fiber, but the biggest shifts show up over several months. Prebiotic fiber also works synergistically with probiotics, making your gut more receptive to new strains. Coming up, we’ll discuss targeted supplements that directly repair and fuel your gut lining.
L-Glutamine is the main fuel for your gut lining cells—called enterocytes. When your gut is under stress from antibiotics, alcohol, or NSAIDs, these cells burn through glutamine rapidly. Supplementing with 5-10 grams per day helps repair the gut barrier and reduce intestinal permeability. Multiple clinical trials show that L-glutamine lowers zonulin levels and improves tight junction integrity [8]. This makes it especially useful after antibiotics or during stressful periods, when your gut is most vulnerable.
Butyrate, the most important short-chain fatty acid, can be taken directly as sodium butyrate or tributyrin at doses of 300-600 mg per day. Butyrate feeds your colon cells, reduces inflammation, and strengthens the connections between gut lining cells. If your fiber intake is low or you’re recovering from antibiotics, direct butyrate supplementation can jumpstart the healing process.
These interventions work best when stacked—using L-glutamine to repair and butyrate to fuel and regulate immune activity. Most users notice improvements in digestion and inflammation markers (like calprotectin and zonulin) within 4-8 weeks. Next, we’ll tackle the habits and substances that most commonly damage young men’s guts.
Knowing what to add is only half the battle. To really restore your gut, you need to cut back on the things that do the most damage. Two culprits top the list for men in their 20s and 30s: alcohol and NSAIDs. Alcohol increases gut permeability within hours of drinking, making it easier for toxins and bacteria to leak into your bloodstream. NSAIDs—like ibuprofen and naproxen—are routinely used for pain management but directly damage your gut lining with chronic use. Both are normalized in young men’s social and athletic circles, but both undermine your gut from the inside out.
Processed foods are another hidden enemy. Emulsifiers, artificial sweeteners, and seed oils found in ultra-processed foods have all been shown to damage the gut lining in controlled studies [9]. Reducing or eliminating these irritants lets your gut lining repair itself and supports a healthier, more diverse microbiome. For alcohol, aim to keep intake under four drinks per week. For pain relief, consider targeted therapies instead of daily NSAIDs.
Cutting back on gut wreckers doesn’t have to be all-or-nothing. Even small, consistent reductions make a difference over time—especially when combined with the rebuilding strategies from earlier sections. Up next: how to recognize trouble early, before gut issues spiral into bigger problems.
Gut problems rarely start with dramatic symptoms. For most young men, the first signs are easy to dismiss: persistent bloating, gas, or irregular bowel movements. These aren’t just minor annoyances—they’re signals that your gut ecosystem is struggling. If you notice your food tolerances getting worse over time (for example, suddenly reacting to dairy or gluten you used to handle), that’s another early warning sign. This pattern often points to progressive gut barrier damage and rising gut permeability.
Another red flag is the connection between your gut and your mind. If you track your mood and notice that anxiety, brain fog, or mood dips coincide with digestive flares, you’re actually seeing the gut-brain axis in action. This isn’t just “in your head.” Research shows the connection is physiological—fixing your gut often improves mental clarity and mood [4].
Paying attention to these trends, especially as a proactive and health-focused man, lets you catch issues early and intervene before they become chronic. In the final section, we’ll put it all together into a practical protocol you can start today.
You now know why gut health is a keystone for everything else—mood, hormones, immunity, and even how you absorb nutrients. For men in their 20s and 30s, the path forward is clear and actionable. Start with a high-quality multi-strain probiotic (10-50 billion CFU/day) focused on research-backed strains like Lactobacillus rhamnosus GG, Bifidobacterium longum, and Saccharomyces boulardii [4][6]. Rotate brands every few months for maximum diversity.
Increase your prebiotic fiber intake to 30-40 grams per day, using a mix of PHGG, acacia, inulin, resistant starch, and psyllium. This combination feeds your beneficial microbes and drives up both diversity and short-chain fatty acid production [7]. Support your gut barrier with L-glutamine (5-10g/day) and, if needed, direct butyrate supplementation (300-600 mg/day) [8]. At the same time, work to reduce chronic NSAID use, limit alcohol to four or fewer drinks per week, and minimize ultra-processed foods [9].
Track your progress using the biomarkers covered earlier—especially calprotectin, zonulin, and your SCFA profile. Most men will see measurable improvements in 4-12 weeks. By making these changes, you’re not chasing trends—you’re rebuilding your foundation for better performance, mood, and long-term health.
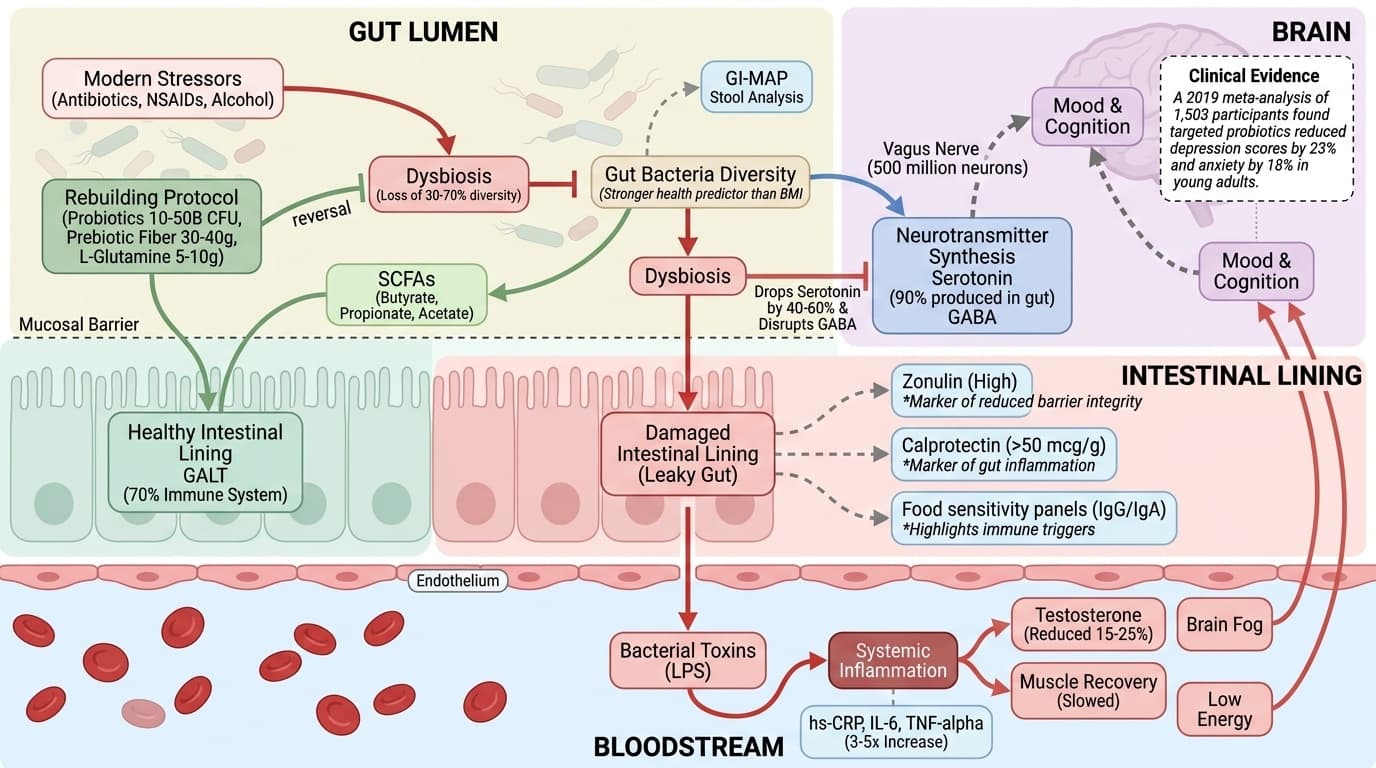
Your Second Brain: The Gut Revolution Every Young Man Needs
Why fixing your gut changes everything—from mood to hormones to performance
Diagram glossary
- BMI:
- A measure of body fat based on an individual's weight and height.
- Calprotectin:
- A protein biomarker in stool used to detect intestinal inflammation.
- CFU:
- A unit used to estimate the number of viable bacteria or fungal cells.
- CRP:
- A protein produced by the liver that indicates inflammation in the body.
- GABA:
- An inhibitory neurotransmitter in the brain that promotes relaxation and reduces neuronal excitability.
- GALT:
- Immune tissue in the digestive tract that protects the body from intestinal pathogens.
- GI-MAP:
- A comprehensive stool test analyzing gut DNA to detect microbes and digestive markers.
- IgG/IgA:
- Major classes of antibodies that provide immune protection in blood and mucosal linings.
- IL-6:
- A cytokine protein involved in regulating immune responses and systemic inflammation.
- LPS:
- A toxic component of bacterial cell walls that triggers strong inflammatory immune responses.
- SCFA:
- Fatty acids produced by gut bacteria that nourish colon cells and reduce inflammation.
- TNF:
- A signaling protein involved in systemic inflammation and the acute phase immune response.
Conclusions
Your gut microbiome controls your mood, immune function, hormone production, and nutrient absorption. For men in your 20s and 30s, this isn't just about avoiding stomach problems—it's about optimizing every system in your body. The path forward is evidence-based and measurable: use targeted probiotic strains at 10-50 billion CFU daily, build fiber diversity to 30-40 grams per day, repair your gut barrier with L-glutamine and butyrate, and eliminate the habits causing hidden damage. Track your progress with calprotectin, zonulin, and microbiome diversity testing. When your gut ecosystem thrives, everything else follows.
While the evidence for gut health interventions is strong, most studies focus on short- to medium-term outcomes. There’s still debate about the long-term effects of specific probiotic strains, the accuracy of some food sensitivity panels, and how best to measure gut diversity in real time. Individual responses can vary, and most research has not focused exclusively on young, healthy men. Always consult a healthcare provider for personalized advice, especially if you have complex symptoms.
Track this in your stack
See how probiotics relates to your health goals and monitor changes in your biomarkers over time.
