Hormonal Health in Your 20s and 30s: Why Your Menstrual Cycle Is Your Fifth Vital Sign
A Comprehensive Guide for Women Navigating Hormones, Fertility, and Health Data
Most women think irregular periods are normal, but here's what's surprising: your menstrual cycle is actually a vital sign. Medical organizations now rank it with blood pressure and heart rate. Hidden hormone problems show up in your cycle years before blood tests catch them.
Your cycle today shapes your bone health, metabolism, and brain function for decades. If you've used birth control since your teens, you may have never seen your body's true signals. Missed periods, bad PMS, or new acne aren't just annoying. They're early warnings about thyroid problems, insulin resistance, or autoimmune disease.
Start tracking your cycle for three months. Test progesterone on days 19-22 of your cycle. Take vitex at 400 mg daily if you have short cycles or bad PMS. Support your thyroid with 200 mcg selenium and 15-30 mg zinc daily. If stopping birth control, start 200 mg magnesium and 50 mg B6 two months before you quit. Your period isn't just about babies. It's your health report card.
- Vitex (Chasteberry)
- Plant supplement that supports progesterone production. Standard dose is 400 mg daily.
- Progesterone
- Prepares uterine lining for pregnancy and supports early gestation. low levels indicate inadequate ovulation or luteal phase defects.
- TPO Antibodies
- Immune proteins that attack your thyroid, often seen in thyroid autoimmune diseases.
- LH/FSH Ratio
- Balance between two brain hormones that control ovaries. Ratio above 2:1 often signals PCOS.
- HOMA-IR (calc)
- Insulin resistance by combining fasting glucose and insulin levels.
- TSH
- Thyroid-stimulating hormone, the primary thyroid function screening test. elevated TSH indicates hypothyroidism, low values suggest hyperthyroidism.
- Post-Pill Amenorrhea
- Missing periods for 3+ months after stopping birth control. Signals hormone recovery problems.
- B6
- A water-soluble vitamin essential for metabolism, brain function, and hormone regulation.
- DHEA-S
- A steroid hormone produced by the adrenal glands that converts into sex hormones.
- insulin
- A pancreatic hormone that regulates blood sugar levels and cellular energy storage.
- LH/FSH
- Pituitary hormones that regulate the menstrual cycle, ovulation, and reproductive function.
- mIU/L
- Milli-international units per liter, a standard measurement for blood hormone concentrations.
Your menstrual cycle reveals your health status in real time. The American College of Obstetricians and Gynecologists made it official in 2015: your cycle is a vital sign, just like blood pressure or heart rate. A healthy cycle runs 28-35 days with minimal pain and moderate flow. When this pattern breaks down, your body is sending an early warning.
These cycle changes often appear years before blood tests show problems. Thyroid disorders, adrenal stress, insulin resistance, and inflammation all disrupt your cycle first. If you've used hormonal birth control since your teens, you may have never seen your natural hormone patterns. This creates a blind spot that can hide developing health issues.
Tracking your cycle as a vital sign helps you catch problems early and respond before they become serious. Your cycle data becomes the foundation for understanding what's happening inside your body and what interventions might help.
The hormonal patterns you establish in your 20s and 30s have effects that echo throughout your life. Bone density, fertility, metabolism, and cognitive resilience are all programmed in part by your hormonal health during these decades. For example, chronic under-eating or intense exercise can lead to hypothalamic amenorrhea—where periods stop for months—quietly robbing your bones of strength. This increases your risk of osteoporosis later in life, even if you restart your cycles.
Thyroid disorders, especially Hashimoto’s thyroiditis, are common in women aged 20-40. This condition is often missed because its early symptoms—like fatigue and low mood—are easily mistaken for stress or depression. Meanwhile, polycystic ovary syndrome (PCOS) affects about 10% of women and often starts in this age group, causing irregular periods, acne, and unwanted hair growth. PCOS also sets up insulin resistance, which can snowball into metabolic issues as you age.
Your decisions about starting or stopping hormonal contraception also play a big role. Birth control can mask irregular cycles and alter hormone levels for months or even years after stopping. Understanding how these interventions affect your body ensures you make informed choices that protect your long-term health. In the next section, we’ll show you the key hormonal biomarkers to track—and why timing matters.
Getting the right hormone tests at the right time gives you actionable data about your health. Here are the key markers with optimal ranges for women 18-39:
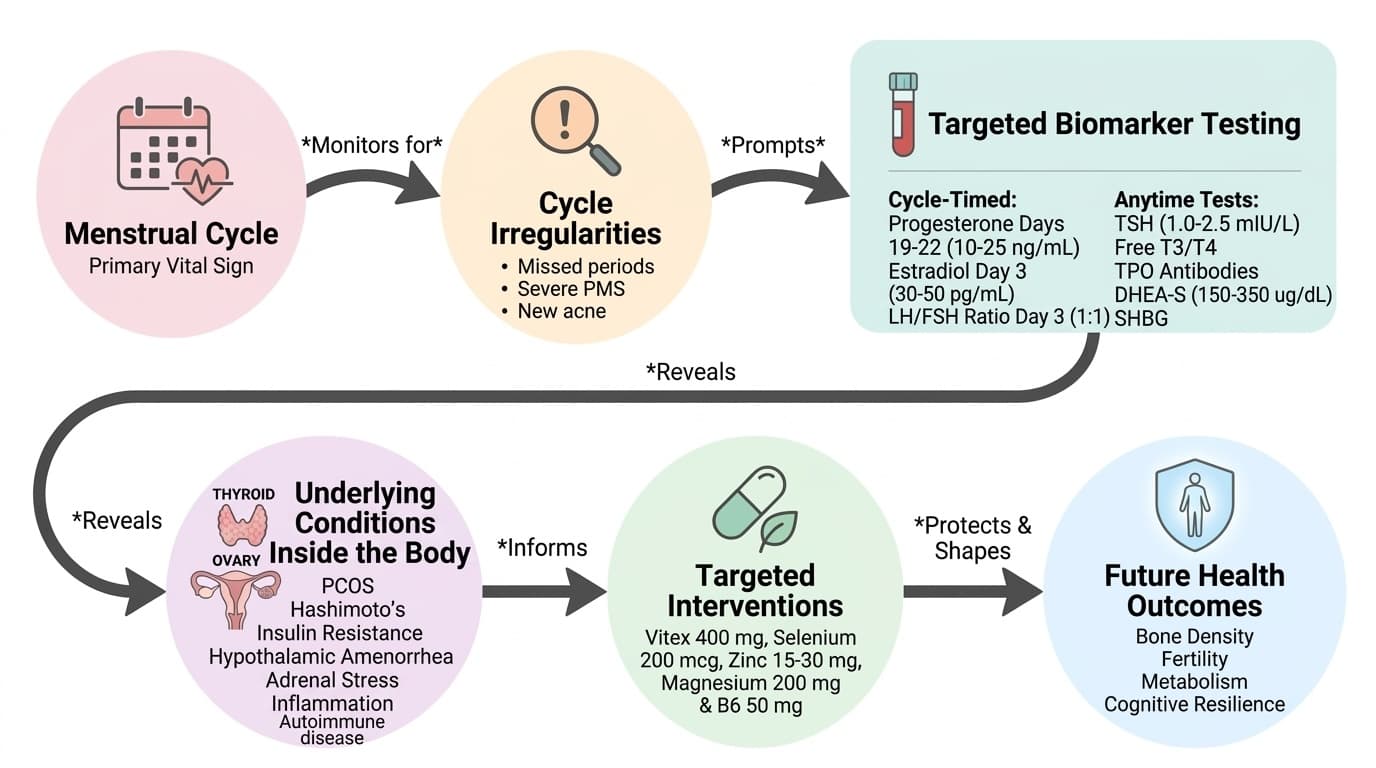
Cycle-Timed Tests: - Progesterone (Days 19-22): Optimal 10-25 ng/mL. Confirms ovulation occurred. Many women with regular periods don't actually ovulate. - Estradiol Day 3: Optimal 30-50 pg/mL. Shows ovarian function and egg reserve. - LH/FSH Ratio Day 3: Optimal around 1:1. Ratios above 2:1 suggest PCOS.
Anytime Tests: - TSH: Optimal 1.0-2.5 mIU/L. Standard range misses early thyroid problems. - Free T3, Free T4: Shows actual thyroid hormone levels, not just brain signals. - TPO Antibodies: Catches Hashimoto's years before TSH changes. - DHEA-S: Optimal 150-350 ug/dL. Reflects stress load and adrenal health. - SHBG: Optimal 40-120 nmol/L. Birth control raises this and levels stay high after stopping.
Timing matters. Random hormone tests can't be interpreted accurately because levels change throughout your cycle.
Each hormone marker responds to specific factors with predictable timelines. Progesterone only rises after ovulation, so stress or undereating that blocks ovulation keeps it low. Most women see progesterone changes within 2-3 cycles of adjusting diet, exercise, or starting vitex at 400 mg daily.
Estradiol responds to body weight, exercise intensity, and sleep quality. Too little or too much of any factor disrupts production. Day 3 estradiol below 30 pg/mL suggests declining egg reserves, which affects fertility timing.
Thyroid markers shift with nutrient status. Selenium at 200 mcg daily can lower TPO antibodies within 3-6 months. Zinc at 15-30 mg daily supports thyroid hormone production, with changes visible in 4-8 weeks. Iodine needs vary based on diet and location.
DHEA-S drops quickly with overtraining or chronic stress, sometimes within weeks. Recovery through sleep optimization and stress management takes 3-6 months. The LH/FSH ratio changes within one cycle based on weight, energy intake, or stress levels.
Key Interactions: Low thyroid suppresses ovulation, dropping progesterone and estradiol. High SHBG from birth control reduces free hormones for 6-18 months after stopping. Understanding these connections helps you target interventions effectively.
Start gathering data and supporting your hormones with this systematic approach:
Month 1-3: Data Collection 1. Track basal body temperature daily and cervical mucus changes. This confirms ovulation better than apps alone. 2. Record cycle length, flow intensity, and symptoms like mood, energy, and skin changes. 3. Get hormone tests timed to your cycle: FSH, LH, estradiol on Day 3; progesterone on Days 19-22.
Immediate Support Protocol: 4. Start thyroid nutrients: 200 mcg selenium, 15-30 mg zinc, adequate iodine from food or supplements. 5. For short luteal phases or PMS: Vitex 400 mg daily, taken consistently for at least 3 months. 6. Support liver function with cruciferous vegetables or DIM supplements if planning to stop birth control.
Pre-Birth Control Transition (2-3 months before stopping): 7. Begin 200 mg magnesium, 50 mg B6, and 15 mg zinc daily to replenish nutrients depleted by hormonal contraception. 8. Establish cycle tracking habits while still on birth control to smooth the transition.
This protocol gives you baseline data and supports your body's natural hormone production. Most women see initial changes within 1-2 cycles.
Every intervention you consider has a specific mechanism and evidence base. Vitex (chasteberry), for example, acts by supporting luteal phase progesterone production. The standard dose is 400 mg daily, which studies indicate may reduce PMS symptoms and lengthen short luteal phases. The form matters—standardized extracts are preferred for consistent results. Synergistically, vitex works best when combined with lifestyle changes that reduce stress and support ovulation.
For thyroid support, selenium at 200 mcg/day helps lower TPO antibodies and supports thyroid hormone conversion, while zinc (15-30 mg/day) is essential for thyroid hormone synthesis. Adequate iodine is necessary but should be tailored to your dietary intake. These nutrients are often depleted in young women, especially those on restrictive diets. Stacking selenium and zinc with a whole-foods diet amplifies the benefit.
If you’re coming off birth control, supporting liver detoxification becomes crucial. Cruciferous vegetables and supplements like DIM (diindolylmethane) enhance estrogen metabolism and help restore a healthy cycle. B6, magnesium, and zinc are commonly depleted by birth control and should be replenished two to three months before stopping. Studies suggest that this approach may reduce post-pill amenorrhea and ease the return of ovulation.
The key is to use evidence-based doses in forms your body can absorb, and to combine interventions for maximum effect. Next, we’ll explain how to watch for early warning signs that your hormones are off track, so you can act before bigger problems develop.
Your cycle provides early signals that something may be wrong. Watch for periods shorter than 24 days or longer than 38 days, sudden changes in flow or duration, and new symptoms like acne along your jawline or hair thinning at the temples. These can be signs of androgen excess, often linked to PCOS or post-pill changes. If your period is missing for more than three months after stopping birth control, that’s called post-pill amenorrhea and deserves evaluation—not just reassurance.
Other red flags include persistent fatigue, feeling cold all the time, or constipation—especially if these accompany menstrual changes. These symptoms often appear years before standard thyroid tests become abnormal, so push for a full thyroid panel including antibodies, not just TSH. Demographic-specific context matters: young women are at higher risk for undiagnosed thyroid disorders and PCOS, and early detection can prevent long-term complications.
Identifying these warning signs early helps you intervene before small issues become major health challenges. In the next section, we’ll show you how to connect your data and symptoms for a personalized approach.
Tracking your cycle, understanding your biomarkers, and using targeted interventions all come together to create a personalized approach to hormonal health. Your unique data—timed labs, symptom tracking, and supplement response—forms a pattern that tells you what’s working and what needs adjustment. For example, if your progesterone rises after starting vitex and your PMS improves, that’s a sign your intervention is effective. If your thyroid antibodies remain high despite supplements, it may be time to work with a specialist.
This personalized strategy is especially important if you’re navigating major transitions, like coming off birth control or preparing for pregnancy. Your data helps you make decisions with confidence, and it gives your healthcare provider a richer picture of your health. For women in their 20s and 30s, this approach sets you up for resilience—not just now, but for decades to come.
In the final section, we’ll summarize the key takeaways and help you move forward with clarity and confidence.
Hormonal Health in Your 20s and 30s: Why Your Menstrual Cycle Is Your Fifth Vital Sign
A Comprehensive Guide for Women Navigating Hormones, Fertility, and Health Data
Diagram glossary
- B6:
- A water-soluble vitamin essential for metabolism, brain function, and hormone regulation.
- DHEA-S:
- A steroid hormone produced by the adrenal glands that converts into sex hormones.
- insulin:
- A pancreatic hormone that regulates blood sugar levels and cellular energy storage.
- LH/FSH:
- Pituitary hormones that regulate the menstrual cycle, ovulation, and reproductive function.
- mIU/L:
- Milli-international units per liter, a standard measurement for blood hormone concentrations.
- ng/mL:
- Nanograms per milliliter, a standard unit of measurement for blood biomarker concentrations.
- PCOS:
- A hormonal disorder causing irregular periods, ovarian cysts, and metabolic issues.
- PMS:
- Physical and emotional symptoms occurring in the days before a menstrual period.
- SHBG:
- A liver protein that binds to sex hormones to regulate their bodily availability.
- TPO:
- An enzyme involved in thyroid hormone production, often targeted by autoimmune antibodies.
- TSH:
- A pituitary hormone that stimulates the thyroid gland to produce thyroid hormones.
- ug/dL:
- Micrograms per deciliter, a standard unit measuring blood hormone and nutrient levels.
Conclusions
Your menstrual cycle provides early warning signals about your health that standard medical checkups often miss. By tracking your cycle patterns, testing hormones at the right times, and using targeted nutrients like vitex, selenium, and magnesium, you can identify and address problems years before they become serious. Don't accept irregular cycles, severe PMS, or chronic fatigue as normal parts of being a woman. Use your cycle data as a diagnostic tool and advocate for the testing and treatment your body needs.
While these recommendations are grounded in current evidence and clinical best practices, most data are based on observational studies or small trials, and individual responses can vary. Not all interventions are universally effective, and some supplements may interact with medications or underlying health conditions. Always consult with a healthcare provider before starting new supplements or making major changes, especially if you have chronic health issues or are planning pregnancy.
Track this in your stack
See how vitex relates to your health goals and monitor changes in your biomarkers over time.
Sources (10)
This article informs how supplementation moves 1 marker.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
