Immune Health After 40: Mastering the Balance Between Defense and Inflammation
A Comprehensive Guide for Men 40–65 to Reclaim Immune Resilience
Here's a surprising fact: by age 45, your thymus—the organ that teaches your immune system to spot new threats—has mostly turned into fat.
Your body fights germs and cancer cells using an old playbook. Your ability to handle new risks quietly fades. After 40, men face weaker defense against infections and stronger harmful inflammation. This raises your risk of heart disease, diabetes, and cancer.
This shift isn't just about catching more colds. The real danger is chronic low-grade inflammation. It slowly damages your blood vessels, brain, and immune cells. You might notice infections that stick around longer. New allergies appear. Aches don't go away. These are early warning signs your immune system is out of balance. If you're in your 40s, 50s, or early 60s, these changes are common but not inevitable.
You can take action today. Daily vitamin D3 (4,000–5,000 IU) supports immune function. EPA-dominant omega-3s (2–3 grams daily) lower harmful inflammation. Quercetin (500–1,000 mg daily) clears out old, damaged cells. Zinc picolinate (25–30 mg daily) boosts T-cell function. Regular moderate exercise—150 minutes weekly—strengthens your immune defenses without burning them out. These strategies help shift your immune system back toward healthy protection. You can stay resilient for decades to come.
- EPA-dominant omega-3s
- A specific form of omega-3 fatty acid supplement where EPA (eicosapentaenoic acid) is present in higher amounts than DHA; EPA is particularly associated with reducing inflammation, making this ratio ideal for controlling chronic inflammation in midlife men.
- Zinc Picolinate
- A specific form of zinc where the mineral is bound to picolinic acid, making it easier for the body to absorb compared to other zinc forms like zinc oxide. It is used in supplements to support immune
- NK cells
- Natural killer cells—immune cells that hunt down virus-infected and cancerous cells. Function declines with age.
- IL-6
- A signaling protein (cytokine) that promotes inflammation and muscle breakdown. Levels rise with age and visceral fat.
- Phytosome
- A delivery system that binds a plant compound to phospholipids to improve absorption.
- Inflammaging
- A term combining 'inflammation' and 'aging' that describes the chronic, low-level inflammation that gradually increases as you get older. Unlike acute inflammation that helps heal injuries, inflammagi
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- COVID
- An infectious respiratory disease caused by the SARS-CoV-2 virus.
- CRP
- A protein produced by the liver that indicates systemic inflammation.
- EPA
- An omega-3 fatty acid that helps lower harmful inflammation in the body.
- insulin
- A hormone produced by the pancreas that regulates blood sugar levels.
- mg
- A metric unit of mass equal to one thousandth of a gram.
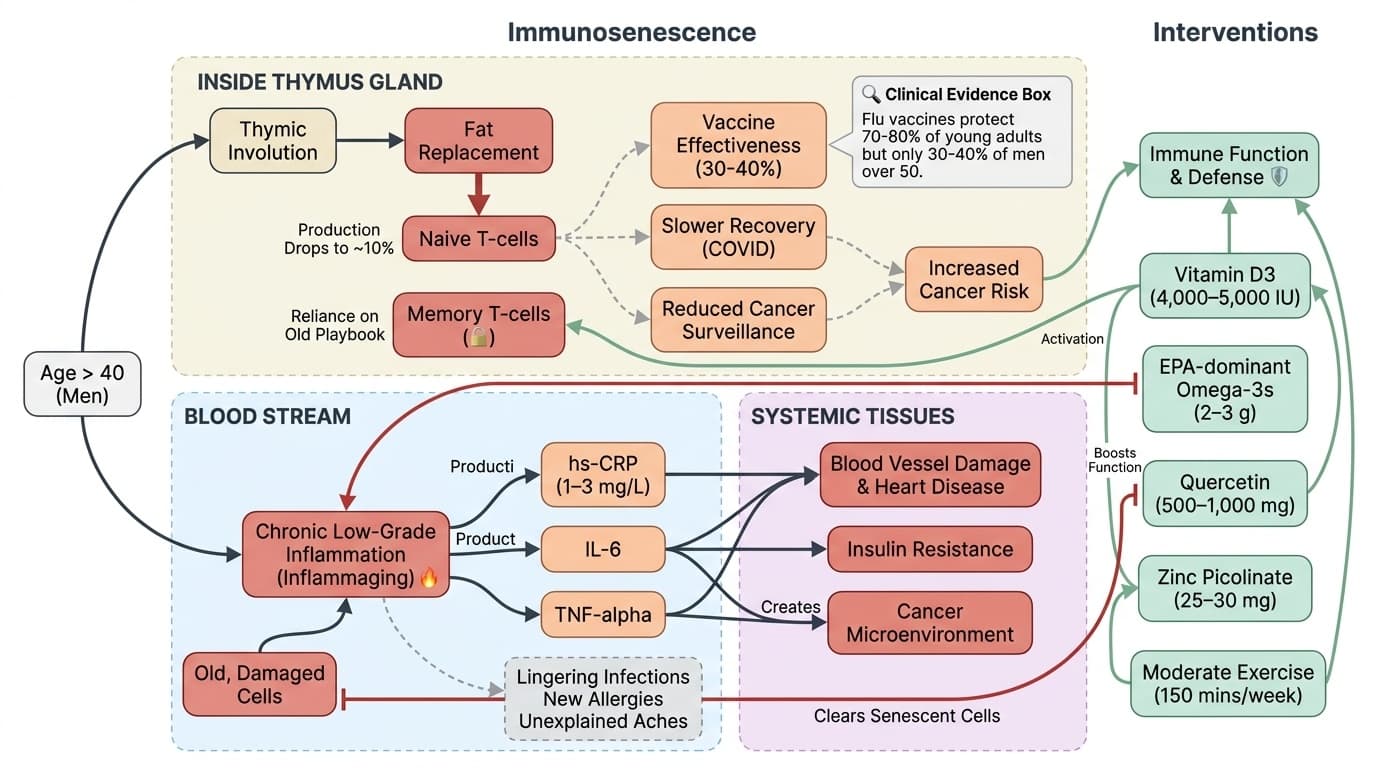
In your 40s and 50s, your immune system enters a new phase—a shift that’s easy to miss but crucial for your long-term health. The most dramatic change happens inside your thymus gland. By the time you hit 45, this small organ, once vital for training T-cells to spot new infections and cancer cells, is mostly replaced by fat. Your production of naive T-cells drops to about 10% of what it was in your youth. As a result, your body relies on memory cells—those trained by past threats—while your ability to handle new viruses or detect early cancer cells quietly diminishes [1].
At the same time, a different problem grows. Chronic, low-level inflammation—what researchers call “inflammaging”—increases year after year. Instead of the short, helpful swelling you get when you sprain an ankle, this kind of inflammation is a slow, constant burn. It harms your blood vessels, encourages insulin resistance, and can even create an environment where cancer cells thrive. This is why heart disease, diabetes, and many cancers become more common after 45 [2].
If you notice infections that linger, new allergies, or unexplained aches, these may be signs of this age-related immune shift. Understanding this transition is the first step to building a strategy that targets both weakened defense and rising inflammation. Next, you’ll see exactly how this double-edged change affects your risks—and what you can do to tip the balance back in your favor.
Immunosenescence is a fancy term for something very real: your immune system’s ability to fight new enemies—like viruses or cancer cells—drops off as you age. This is especially important for men between 40 and 65. Your thymus, which once produced armies of naive T-cells, has shrunk to almost nothing by your mid-40s. Instead, your immune system is running on memory, not fresh recruits [3].
Why does this matter? Vaccine effectiveness drops sharply. For example, flu vaccines protect 70–80% of young adults but only 30–40% of men over 50 [4]. Recovery from infections like pneumonia or COVID takes longer and carries more risk for complications. Your chance of developing cancer also climbs because your immune system’s “surveillance” function—hunting down abnormal cells—weakens just as cancer risk rises.
You may notice you’re getting sick more often, or that it takes longer to bounce back. These aren’t just annoyances—they’re early signs your defenses are slipping. The drop in naive T-cells also alters your immune balance, making you more likely to develop autoimmune conditions. Understanding immunosenescence helps you spot warning signs sooner and shows why it’s so important to support your immune system with targeted nutrition and lifestyle changes.
While your immune system’s ability to fight new threats is fading, its tendency to cause harm is rising. After 40, chronic low-grade inflammation—known as inflammaging—becomes a persistent threat. Blood markers like hs-CRP, IL-6, and TNF-alpha increase year after year, even if you feel healthy [5].
This type of inflammation is not the helpful kind you get after an injury. Instead, it’s a slow, ongoing process that damages blood vessels, encourages insulin resistance, and accelerates aging in your brain and muscles. It also creates a microenvironment where cancer cells can grow more easily. Even modestly elevated hs-CRP (1–3 mg/L) doubles or triples your risk of a heart attack, regardless of your cholesterol [6].
Men in their 40s through 60s are at the highest risk for this silent problem. Early signs include persistent aches, new allergies, and chronic skin issues. The rise in autoimmune diseases like psoriasis and rheumatoid arthritis during these years is also linked to inflammaging. Recognizing and lowering this “background fire” is essential for protecting your long-term health—and sets up the next step: understanding the most important biomarkers to track.
Tracking the right blood markers lets you see what's happening inside your immune system. Here are the most important ones for men between 40 and 65:
hs-CRP: This marker shows your level of systemic inflammation. The standard range is <3.0 mg/L, but the optimal target is <1.0 mg/L. Levels between 1–3 mg/L double your heart disease risk. Over 3 mg/L triples cancer risk and should prompt investigation for sources of inflammation like dental issues, visceral fat, or chronic infection [7]. hs-CRP drops 20–40% with omega-3 supplementation and regular exercise within 8–12 weeks.
ESR (Erythrocyte Sedimentation Rate): Target is <15 mm/hr. When both ESR and hs-CRP are elevated, chronic inflammation is confirmed. ESR responds more slowly, typically dropping over 3–6 months with intervention.
IL-6: Target is <1.8 pg/mL. IL-6 drives both muscle loss and inflammation, especially in men with excess belly fat. Reducing IL-6 by 30–50% requires weight loss around the midsection plus targeted supplements. IL-6 and hs-CRP usually drop together.
WBC Differential: Lymphocytes should be 20–40% of your white blood cells. A drop in lymphocytes with a rise in neutrophils signals immunosenescence. Advanced panels measuring CD4/CD8 ratios give deeper insight but aren't always available.
Vitamin D (25-OH): Optimal range is 50–70 ng/mL. Vitamin D boosts antimicrobial peptide production by 300% and calms autoimmune inflammation. Deficiency below 30 ng/mL impairs both infection defense and inflammation control. Raising vitamin D from deficient to optimal takes 6–12 weeks of supplementation.
Fasting Glucose and Insulin: Glucose should be <95 mg/dL, insulin <5 uIU/mL. High glucose and insulin both impair immune cell function and increase inflammation markers by 40–60%. Improvement typically appears within 2–4 months of lifestyle changes.
These biomarkers help you spot problems early and measure intervention success. Next, we cover the strategies that move these numbers in the right direction.
Specific nutrients can help rebalance your immune system and reduce harmful inflammation. Here’s what research suggests for men 40–65:
1. Vitamin D3 (4,000–5,000 IU daily, titrate to 50–70 ng/mL): Vitamin D is a potent immunomodulator. It boosts your body’s production of antimicrobial peptides and shifts your immune balance away from autoimmunity. Deficiency is present in up to 60% of men over 40. Supplementation has been shown to reduce respiratory infection risk by 30–50% [8]. The form matters: use vitamin D3 (cholecalciferol), not D2. Effects are usually seen in 4–8 weeks.
2. Omega-3 (EPA-dominant, 2–3 grams daily): EPA is the building block for molecules called SPMs, which help your body resolve inflammation safely. Most men have a high omega-6 to omega-3 ratio, which promotes inflammation. EPA supplementation consistently lowers hs-CRP and IL-6 within a few months [9]. Fish oil should be high in EPA relative to DHA for optimal immune benefits.
3. Quercetin (500–1,000 mg daily): This flavonoid acts as a senolytic, helping clear out old, dysfunctional cells that release inflammatory signals. It also stabilizes mast cells, reducing allergic inflammation, and shows promise as an antiviral. Look for quercetin phytosome or with bromelain for better absorption [10]. Effects may appear within 1–2 months.
4. Zinc (25–30 mg daily, as picolinate or bisglycinate): Zinc is crucial for T-cell, NK cell, and neutrophil function. Deficiency is common due to reduced absorption and medication use in older men. The best forms are picolinate or bisglycinate, which are better absorbed than zinc oxide. Results can be seen within weeks [11].
Stacking these supplements (with a meal, especially for zinc and quercetin) helps maximize immune benefits and minimize stomach upset. Each works through different mechanisms, and together they address both immune defense and excess inflammation. Next, let’s look at the role of exercise in immune health.
Regular, moderate exercise is one of the most effective ways to support your immune system as you age. For men in midlife, the target is about 150 minutes per week—think brisk walking, cycling, or moderate gym sessions [12]. This level of activity improves NK cell function, boosts neutrophil response, and lowers inflammatory markers like hs-CRP and IL-6.
But more is not always better. High-volume endurance training or excessive HIIT can actually suppress your immune function for up to 72 hours afterward. This so-called “J-shaped curve” means moderate exercise is protective, but overtraining leaves you more vulnerable to infections and slows recovery.
The mechanism is partly hormonal: moderate activity raises anti-inflammatory cytokines and enhances immune cell surveillance, while excessive exercise triggers stress hormones that impair immune response. If you notice more frequent or severe colds after upping your training, you may be pushing too hard.
Combining moderate exercise with targeted supplements produces a synergy—each intervention lowers inflammation and improves immune cell function through distinct pathways. Next, we’ll explore the often-overlooked gut-immune connection and its importance for midlife men.
About 70% of your immune system is located in your gut—a network called GALT. When your gut barrier is strong, it keeps harmful bacteria and toxins out of your bloodstream. But as you age, factors like NSAID use, acid blockers (PPIs), alcohol, and even chronic stress can make your gut more “leaky.”
This leakiness lets bacterial fragments (like LPS) enter your blood, triggering your immune system to stay on high alert. The result is persistent, low-grade inflammation that feeds into heart disease, diabetes, and even neurodegeneration [13].
Men over 40 are especially at risk, since gut permeability rises and medication use is common. Signs include bloating, frequent indigestion, or unexplained fatigue. Improving gut health—by reducing unnecessary NSAIDs, moderating alcohol, and increasing fiber and fermented foods—can lower systemic inflammation. Some supplements, including omega-3s and quercetin, also help support gut barrier integrity.
Understanding the gut-immune connection points to another reason why tracking inflammation markers matters. Next, we’ll discuss early warning signs and when to seek further evaluation.
Your immune system gives you clues when things aren’t right. For men 40–65, these warning signs deserve special attention:
- Infections that last longer or recur more often: If colds now take 10–14 days instead of 5, or you’re getting sick more than 2–3 times a year, your adaptive immunity may be lagging. - Persistent hs-CRP above 3.0 mg/L without acute illness: This is not a harmless number. It’s a signal your body is in a chronic inflammatory state. Causes to consider include dental disease, excess abdominal fat, sleep apnea, gut issues, or undiagnosed autoimmune conditions. - New allergies, skin rashes, or joint stiffness: Developing eczema, psoriasis, or environmental allergies in midlife often means your immune system is losing its ability to distinguish self from non-self.
If you spot these issues, it’s time for a deeper evaluation. That means working with a health professional to check for sources of inflammation, review your medication use, and update cancer screenings. Early action can prevent long-term complications—and sets you up for the final step: long-term disease prevention.
After 45, your risk for cancers—especially prostate, colon, and lung—rises sharply. This is partly because your immune system’s ability to spot and eliminate abnormal cells is fading. Declining T-cell and NK-cell function, combined with chronic inflammation, creates an environment where cancers are more likely to take hold [14].
Cancer screening is no longer optional for men after 45. Colonoscopies, PSA checks, and skin exams are essential. Early-stage cancers are much easier to treat, but as your immune “surveillance system” weakens, you can’t rely on your body alone to catch problems early.
Supporting your immune health with nutrients, exercise, and gut care improves your odds—but screening is your safety net. By tackling both inflammation and immunosenescence, you’re not just avoiding sick days. You’re making a long-term investment in lowering your risk of serious disease for decades to come.
Immune Health After 40: Mastering the Balance Between Defense and Inflammation
A Comprehensive Guide for Men 40–65 to Reclaim Immune Resilience
Diagram glossary
- COVID:
- An infectious respiratory disease caused by the SARS-CoV-2 virus.
- CRP:
- A protein produced by the liver that indicates systemic inflammation.
- EPA:
- An omega-3 fatty acid that helps lower harmful inflammation in the body.
- IL-6:
- A signaling protein that regulates immune responses and inflammation.
- insulin:
- A hormone produced by the pancreas that regulates blood sugar levels.
- mg:
- A metric unit of mass equal to one thousandth of a gram.
- Quercetin:
- A plant flavonoid and antioxidant that helps clear out old, damaged cells.
- TNF:
- A cell signaling protein involved in systemic inflammation and immune regulation.
- Vaccine:
- A biological preparation that provides active acquired immunity to a specific infectious disease.
- vitamin D3:
- A fat-soluble vitamin that supports immune function and overall health.
Conclusions
Immune health in midlife isn’t about dodging the occasional cold. For men 40–65, the real challenge is rebalancing a system that’s losing its edge against new threats while quietly fueling chronic inflammation. Tracking the right biomarkers, optimizing vitamin D, omega-3s, zinc, and quercetin, and sticking to moderate exercise can shift your immune system back toward healthy surveillance and lower your risk of the diseases that matter most—heart disease, diabetes, neurodegeneration, and cancer. Early warning signs and regular screening help you stay one step ahead. Immune aging is not destiny, and men who act now can reshape their health trajectory for years to come.
This article summarizes current evidence and expert consensus but does not replace individual medical advice. Some recommendations, such as advanced immune cell panels or high-dose supplementation, may not be appropriate for everyone and should be personalized with a healthcare professional. Most cited studies focus on broad populations, and individual response may vary. More research is needed on long-term effects of supplement stacking, especially in men with complex health conditions.
Track this in your stack
See how vitamin d3 relates to your health goals and monitor changes in your biomarkers over time.
