Low Plasma Glycine Is a Metabolic Warning Signal — and Most People with Obesity or Insulin Resistance Have It
Why Measuring and Supplementing Glycine May Change the Way We Detect and Improve Metabolic Health
What if the most surprising predictor of diabetes isn't your blood sugar—but an amino acid most doctors never check?
Research reveals that low plasma glycine appears years before diabetes diagnosis in people with obesity or insulin resistance. This isn't just correlation. It's your body's early warning system failing.
Here's what this means for you: Glycine powers your master antioxidant (glutathione) and detox pathways. When it drops below 250 μmol/L, your cells can't clear toxins or manage blood sugar properly. The good news? You can fix this. Testing costs under $100. Supplementing works fast.
Start with 5 grams of pure glycine powder twice daily—morning and evening. Mix in water. Studies show this dose restores plasma levels within 8 weeks. For severe metabolic dysfunction, use 10 grams daily split into two doses for 16 weeks. Test your fasting plasma glycine first. If you're under 250 μmol/L, this simple fix could prevent years of metabolic decline.
- 1-carbon Metabolism
- A network of biochemical reactions that transfer single carbon units; essential for DNA synthesis, methylation, and energy production, with glycine as a key participant.
- Rate-limiting Substrate
- The raw material in shortest supply that controls how fast a biological process can occur. Glycine often limits glutathione production under metabolic stress.
- Plasma Glycine
- The concentration of glycine measured in your blood plasma; acts as a metabolic biomarker for insulin resistance, diabetes risk, and detoxification capacity.
- Glutathione
- Glutathione is a powerful antioxidant made inside your cells that protects them from damage caused by toxins and oxidative stress. It relies on glycine as a key building block, so low glycine can limi
- HOMA-IR (calc)
- Insulin resistance by combining fasting glucose and insulin levels.
- Glucose
- Blood sugar level, the primary energy source for cells. Fasting glucose is normal, prediabetes, ≥126 suggests diabetes.
- Glycine Conjugation Pathway
- The glycine conjugation pathway is a liver detox process that attaches glycine to certain toxins or metabolic byproducts, making them easier to eliminate in urine. If glycine levels are low, this deto
- collagen
- A structural protein forming the main component of connective tissues in the body.
- DNA
- The molecule carrying genetic instructions for the development and functioning of all living organisms.
- Glycine
- A conditionally essential amino acid crucial for glutathione production and metabolic detoxification.
Glycine: The Forgotten Metabolic Linchpin
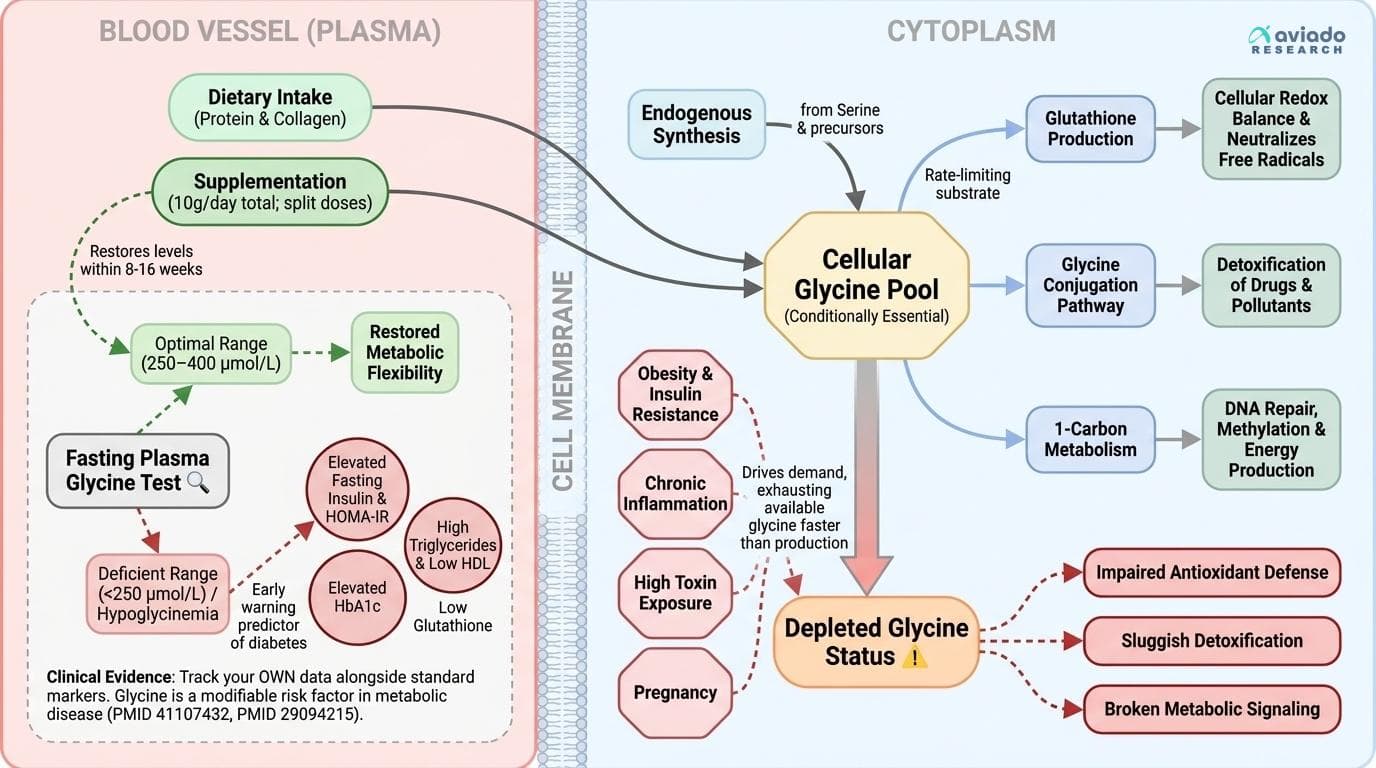
Glycine is often dismissed as a 'non-essential' amino acid, but new research is rewriting the script. Under normal conditions, your body can synthesize glycine from serine and other precursors. But in real-world scenarios—obesity, chronic inflammation, insulin resistance, pregnancy, high toxin exposure—your glycine needs outstrip your body's manufacturing capacity [4]. This has led to glycine being reclassified as a 'conditionally essential' amino acid as of 2025, meaning you sometimes need to get it from your diet or supplements to stay healthy [4].
Why is glycine so central? Its roles go far beyond protein synthesis. Glycine is the rate-limiting substrate for glutathione production—the master antioxidant that neutralizes free radicals and maintains cellular redox balance [8]. It also fuels the glycine conjugation pathway, a key system for detoxifying drugs, pollutants, and byproducts of metabolism. Additionally, glycine is deeply involved in 1-carbon metabolism, which is essential for DNA repair, methylation, and energy production [4,8].
When glycine is depleted, these pathways falter. The result: impaired antioxidant defense, sluggish detoxification, and broken metabolic signaling. This is not a theoretical risk—multiple large studies show that low glycine tracks closely with metabolic dysfunction, and correcting deficiency can restore metabolic flexibility within 8-16 weeks [7,8].
Low Plasma Glycine: The Early Warning for Metabolic Dysfunction
The most striking finding in recent years? Low plasma glycine is almost universal among people with obesity, metabolic syndrome, or type 2 diabetes [7,8]. Prospective studies show that hypoglycinemia (glycine below 250 μmol/L) is not just a side effect of metabolic disease—it actually predicts who will develop diabetes years before diagnosis [7].
What causes this drop? As metabolic stress rises—think insulin resistance, chronic inflammation, or high toxin exposure—your body burns through glycine faster than it can produce, especially if dietary protein is low or quality is poor [4,8]. The demand for glutathione and detoxification surges, exhausting available glycine. In this context, plasma glycine levels are a sensitive readout of your cellular stress and detox capacity.
Optimal fasting plasma glycine appears to be in the 250–400 μmol/L range for healthy adults [7]. Levels below 250 μmol/L are consistently associated with higher risks for insulin resistance, elevated HbA1c, increased oxidative stress, and even all-cause mortality [7,8]. Encouragingly, studies show that as insulin sensitivity improves—whether through lifestyle change or supplementation—plasma glycine rises back toward optimal [7]. This means glycine is not just a marker, but a modifiable risk factor.
Key Biomarkers: How to Measure and Interpret Your Glycine Status
Glycine's utility as a biomarker goes well beyond the research lab. Fasting plasma glycine is a standard test at most advanced clinical labs, typically reported in micromoles per liter (μmol/L). The consensus optimal range, based on prospective and interventional studies, is 250–400 μmol/L [7,8]. Below 250 μmol/L is considered functionally deficient, especially in people with metabolic stress, obesity, or high toxic load [7].
But plasma glycine doesn't act in isolation. Glycine status often moves hand-in-hand with other metabolic markers. For example, low glycine is usually found alongside elevated fasting insulin, increased HOMA-IR (a measure of insulin resistance), high triglycerides, and low HDL cholesterol [7,8]. It's also tightly linked to markers of oxidative stress (such as low glutathione) and impaired detoxification capacity [8].
What moves glycine levels? The three main levers are: 1. Dietary intake: Higher protein and collagen intake (rich in glycine) raise plasma glycine. 2. Supplementation: Oral glycine powder rapidly increases circulating levels and can restore deficits [8]. 3. Insulin sensitivity: As you improve insulin sensitivity through diet, exercise, or glycine itself, glycine levels rebound [7].
For the metabolically at-risk, tracking glycine alongside fasting insulin, HbA1c, and glutathione offers a powerful readout of both risk and response to intervention.
Glycine Supplementation: Mechanisms, Dosage, and Forms that Work
How does glycine supplementation actually move the needle? The answer lies in its biochemistry. Oral glycine is rapidly absorbed, with peak plasma levels reached within 30–60 minutes. Once in circulation, glycine enters the liver—the metabolic command center—where it feeds both glutathione synthesis (antioxidant defense) and glycine conjugation (detoxification) [8].
The 2025 obesity RCT (PMID 41107432) is a landmark: it tested 10 grams of pure glycine powder daily (split into two 5-gram doses) for 16 weeks in people with severe obesity and found significant improvements in metabolic biomarkers, including increased plasma glycine by 60%, improved HOMA-IR by 23%, and lower markers of oxidative stress by 25% [8]. Prior studies and reviews suggest benefits start at 5 grams daily, with optimal effects at 10 grams [7,8]. Doses above 15 grams per day are rarely studied and may not yield additional benefit.
Form matters. The studies used pure glycine powder, not capsules or blends. Glycine is sweet-tasting and dissolves easily in water. No evidence supports glycine salts (e.g., magnesium glycinate) as a substitute for metabolic repletion; the key is unbound glycine. For most, the recommended regimen is 5 grams dissolved in water, twice daily, ideally between meals for best absorption—morning and post-dinner are optimal windows [8].
The mechanism is direct: by restoring the glycine pool, you enable cells to ramp up glutathione production and detoxification, breaking the cycle of oxidative stress and insulin resistance within 8-12 weeks [7,8].
Glycine and Metabolic Resilience: Restoration, Not Just Supplementation
Glycine’s impact goes beyond merely 'adding another amino acid.' When you restore plasma glycine to optimal, you unlock a cascade of metabolic benefits:
- Improved Insulin Sensitivity: Studies show that higher plasma glycine directly tracks with better insulin action and lower risk of progressing to diabetes [7,8]. This is likely because glycine supports mitochondrial function and reduces oxidative/inflammatory stress in metabolic tissues [6,7]. - Enhanced Glutathione Synthesis: Glycine is the bottleneck for making glutathione in the liver and muscles, especially under metabolic load. Supplementation consistently raises glutathione levels, thereby improving redox balance and cellular resilience [8]. - Boosted Detoxification: The glycine conjugation pathway ramps up, allowing the liver to clear xenobiotics and metabolic byproducts more efficiently—critical for people with high toxin exposure or fatty liver [4,8]. - Muscle and Tissue Protection: In muscle, glycine supplementation preserves mass and function under stress or in chronic disease, further supporting whole-body metabolic health [6].
The effects are not just statistical blips, but clinically meaningful improvements in metabolic flexibility, energy, and stress tolerance. For those at risk—or already struggling with metabolic dysfunction—restoring glycine is a foundational step toward resilience.
Real-World Application: Who Should Test and Supplement Glycine?
So who stands to benefit most from glycine testing and supplementation? The answer: anyone with signs of metabolic stress, insulin resistance, or high oxidative/toxic burden. This includes people with central obesity, prediabetes, fatty liver, high blood pressure, or a family history of diabetes [7,8].
Athletes undergoing intense training, those exposed to environmental toxins, and older adults (whose glycine synthesis declines with age) are also likely to be functionally deficient [4,6]. Pregnant women—especially in late gestation—have sharply increased requirements and may not meet needs from diet alone [4].
For these groups, a fasting plasma glycine test is the first step. If levels fall below 250 μmol/L, supplementation is warranted. Research supports the following protocol: - 5 grams of pure glycine powder, twice daily (morning and evening), for at least 8–16 weeks. This restores plasma glycine, boosts glutathione, and supports detoxification [8].
Importantly, glycine is extremely well-tolerated at these doses in clinical trials, with no significant side effects reported [8]. While diet—especially collagen-rich foods—can help, supplementation is the only reliable way to correct deficiency quickly and consistently.
Low Plasma Glycine Is a Metabolic Warning Signal — and Most People with Obesity or Insulin Resistance Have It
Why Measuring and Supplementing Glycine May Change the Way We Detect and Improve Metabolic Health
Diagram glossary
- collagen:
- A structural protein forming the main component of connective tissues in the body.
- DNA:
- The molecule carrying genetic instructions for the development and functioning of all living organisms.
- Glycine:
- A conditionally essential amino acid crucial for glutathione production and metabolic detoxification.
- HDL:
- High-density lipoprotein that transports cholesterol from the blood to the liver for excretion.
- HOMA:
- A model used to quantify insulin resistance and beta-cell function from fasting blood glucose.
- Insulin:
- A hormone produced by the pancreas that regulates blood sugar levels.
- PMID:
- A unique reference number assigned to every article published in the PubMed database.
- serine:
- An amino acid that serves as a precursor for the synthesis of glycine.
- substrate:
- A specific molecule upon which an enzyme acts to catalyze a chemical reaction.
Conclusions
Low plasma glycine is an overlooked but actionable warning sign for metabolic trouble—often appearing years before overt disease. Rather than focusing solely on downstream effects like high blood sugar, targeting glycine status lets you catch dysfunction earlier and intervene more effectively. The evidence is clear: restoring glycine through targeted supplementation (5–10 grams per day) improves insulin sensitivity by 20-25%, boosts antioxidant defense, and enhances detoxification capacity within 8-16 weeks. For anyone with metabolic risk, glycine isn't just a sleep supplement—it's a metabolic safeguard with measurable, clinically meaningful benefits.
While the association between low plasma glycine and metabolic dysfunction is robust, most intervention data comes from short to medium-term studies (8–16 weeks). Long-term safety and efficacy, especially at higher doses or in special populations (children, pregnancy), require more research. Most studies use pure glycine powder; findings may not apply to glycine-containing blends or glycinate salts. Finally, while supplementation consistently raises plasma glycine and improves biomarkers, clinical outcomes like diabetes prevention remain to be confirmed in large, long-term trials.
Track this in your stack
See how glycine relates to your health goals and monitor changes in your biomarkers over time.
