Why Your Biotin Supplement Might Be Sabotaging Your Lab Results
How high-dose biotin creates false hormone and vitamin D readings—and what to do about it
You might be surprised to learn that your daily biotin supplement could make your blood tests completely unreliable.
High-dose biotin—often found in hair, skin, and nail formulas—can trick some of the most common lab tests into reporting dangerously incorrect results. That means your thyroid or vitamin D levels might look off, not because of a real health problem, but because of your supplement.
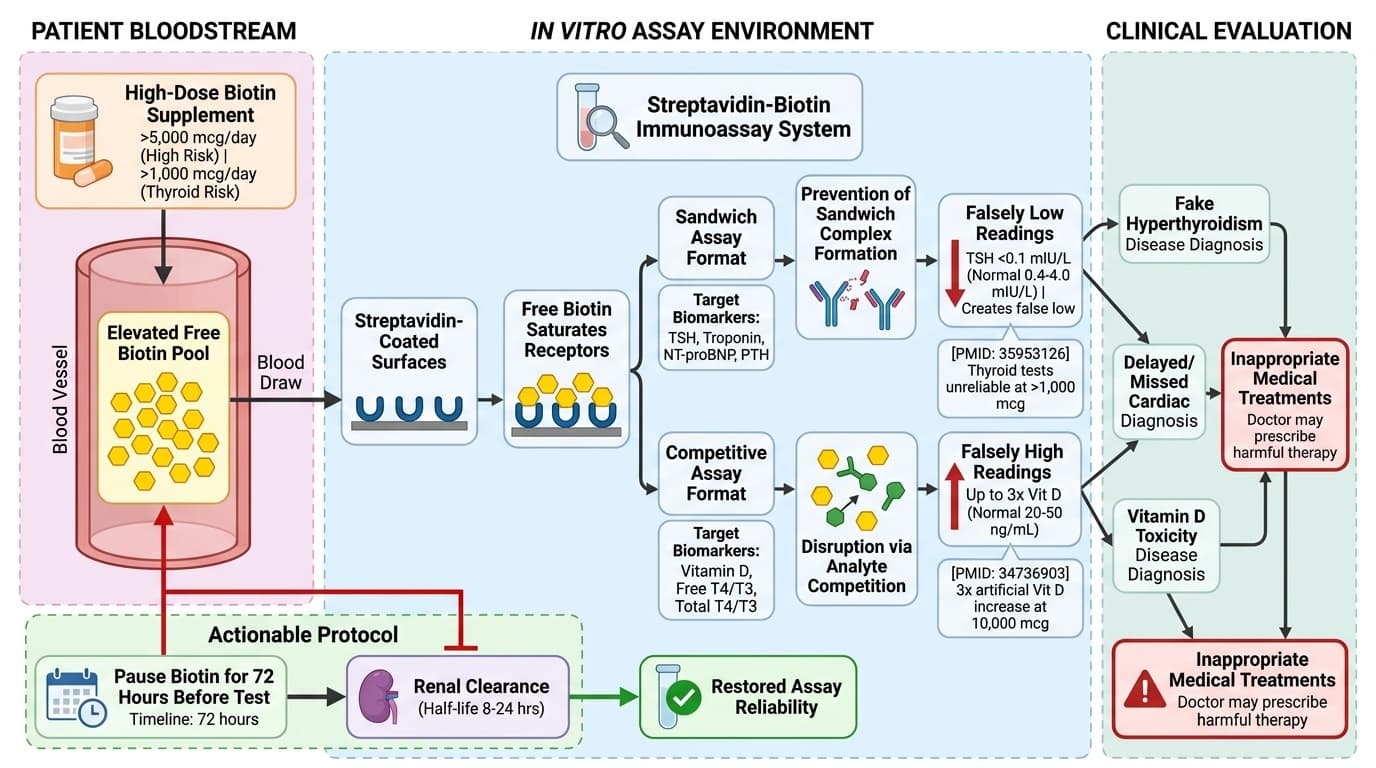
Researchers recently discovered that biotin interferes with a common lab technology called the 'streptavidin-biotin immunoassay.' This technique is used to measure hormones, vitamins, and even cardiac markers. When there is too much biotin in your blood, these tests can give false highs or false lows. People have been falsely diagnosed with hyperthyroidism, vitamin D toxicity, and other conditions—sometimes leading to unnecessary treatments or missed true diagnoses.
If you take more than 5,000 micrograms of biotin per day, studies show you are at high risk for this kind of lab interference. In clinical trials, just 10,000 micrograms per day was enough to create fake high vitamin D readings, while some thyroid tests were unreliable at doses as low as 1,000 micrograms. To avoid these problems, stop all biotin supplements for at least 72 hours before your next blood test. If you want to support hair or nail health, use 2,500 micrograms daily, but always pause it for three full days before any lab work. This simple step can save you from a misdiagnosis and unnecessary medical treatments.
- Enteric-coated
- A dosage form designed to resist stomach acid and release later in the intestine.
- Liposomal
- A delivery form that wraps a compound in tiny fat-like spheres to improve absorption or stability.
- 25-hydroxy vitamin D
- The main form of vitamin D measured in blood tests. Biotin interference can cause false high readings.
- Half-life
- The time it takes for half of a substance to be cleared from the bloodstream. Biotin's half-life determines how long you need to stop it before a lab test.
- Streptavidin-biotin immunoassay
- A lab test technology that uses biotin and streptavidin to measure blood markers such as hormones and vitamins. High blood biotin interferes with the results.
- Free T4
- Free thyroxine, the unbound active thyroid hormone in circulation. low levels cause fatigue and weight gain, high values cause anxiety and weight loss.
- TSH (Thyroid-Stimulating Hormone)
- A hormone measured to assess thyroid function. Biotin can cause TSH levels to appear falsely low on certain tests.
- Biotin
- A B-vitamin often used in supplements that can interfere with certain laboratory immunoassays.
- mIU/L
- Milli-international units per liter, a standard unit of measurement for blood hormone levels.
- ng/mL
- Nanograms per milliliter, a standard unit of measurement for concentration in blood tests.
- PMID
- A unique reference number assigned to every article published in the PubMed database.
- proBNP
- A protein biomarker measured in blood to help diagnose and evaluate heart failure.
You might think of biotin as just a beauty vitamin, but it can directly affect your medical lab results—sometimes dangerously so. The reason is rooted in how many modern immunoassays are designed. These tests often use a system called the streptavidin-biotin complex, which is prized for its ability to bind molecules with extreme tightness. This system is used in assays for hormones like TSH, free T4, and for vitamin D, along with many other markers your doctor checks for.
When you take high-dose biotin, your blood contains so much free biotin that it floods the assay system. The free biotin competes with test components, either blocking or mimicking what the assay is supposed to detect. For example, in a sandwich immunoassay (common for TSH), excess biotin can prevent the test from registering the true amount of hormone, making your TSH appear falsely low. In competitive assays (like some vitamin D tests), biotin can make your vitamin D look abnormally high.
A clinical trial (PMID: 34736903) demonstrated that people taking 10,000 micrograms of biotin had vitamin D levels that appeared three times higher than they actually were, until their blood was processed to remove biotin. These false readings aren't just numbers—they can trigger unnecessary medical treatments, like being told you have hyperthyroidism or vitamin D toxicity when your levels are actually normal. This interference can happen within hours of taking a dose and may persist for 24–72 hours, depending on your kidney function and dose. As biotin supplementation has skyrocketed—especially among women and people seeking hair or nail benefits—so has the risk of lab interference. Now that you know how biotin disrupts lab assays, it’s crucial to understand which biomarkers are most affected and how to interpret them safely.
The biomarkers most susceptible to biotin interference are those measured by immunoassays using the streptavidin-biotin system. These include TSH (thyroid-stimulating hormone), free T4, free T3, total T4, total T3, 25-hydroxy vitamin D, parathyroid hormone (PTH), and certain cardiac markers like troponin and NT-proBNP. Standard laboratory ranges for TSH are typically 0.4–4.0 mIU/L, but the optimal range for most adults aiming for thyroid wellness is 1.0–2.5 mIU/L. Biotin interference can make your TSH look falsely low, sometimes below 0.1 mIU/L, mimicking the pattern seen in hyperthyroidism. Free T4 and T3 may appear falsely elevated, creating a misleading picture of overactive thyroid.
For vitamin D, the standard range for 25-hydroxy vitamin D is 20–50 ng/mL, with optimal levels for most adults considered between 40–60 ng/mL. A clinical trial (PMID: 34736903) found that biotin supplementation at 10,000 micrograms daily caused falsely elevated vitamin D readings—up to three times the true value. These changes can occur within 24 hours of dosing, especially in people with normal kidney function. However, the effect may last longer in older adults or people with reduced kidney clearance, as biotin's half-life is extended.
The timeline to see false readings is rapid—within 12 hours of a high-dose supplement, and persisting up to 72 hours after stopping. Biomarkers like troponin, which are used to diagnose heart attacks, can also be affected, leading to delayed or missed diagnoses. This is especially risky for older adults and those with cardiovascular risk factors. Understanding which biomarkers are at risk helps you know when to be extra cautious with supplement timing, and sets the stage for practical steps to protect your results.
The molecular issue comes down to biotin’s extraordinary binding affinity. Biotin binds to streptavidin with one of the tightest non-covalent interactions in biology. In immunoassays, this property is used to capture or detect analytes by attaching biotin to antibodies or antigens, then capturing them with streptavidin-coated surfaces. If your blood is loaded with free biotin from supplements, that free biotin saturates the streptavidin sites, blocking the assay from working as designed.
A 2020 review (PMID: 35953126) details how the impact of this interference depends on the assay format. In sandwich assays, used for TSH and some cardiac markers, excess biotin leads to falsely low results. In competitive assays, used for vitamin D and some hormones, it can cause falsely high readings. The amount of interference is dose-dependent: studies show that as little as 1,000 micrograms (1 mg) of biotin daily can skew some lab results, especially in sensitive individuals. Doses above 5,000 micrograms have a much more pronounced effect, and levels used in neurological disease trials (100,000 micrograms) can cause extreme distortions.
The timeline for biotin removal from blood is governed by its half-life, which ranges from 8 to 24 hours depending on age, kidney health, and dose. Interactions with other supplements are minimal—biotin does not compete with other B-vitamins for absorption—but stacking it with other high-dose supplements doesn’t reduce the risk of assay interference. The only reliable solution is to stop biotin well in advance of any blood draw. Recognizing these molecular details empowers you to time your supplementation for both benefit and lab safety.
Biotin’s pharmacokinetics are crucial for accurate lab testing. When you take biotin orally, it’s almost fully absorbed, with a bioavailability close to 100% in standard supplement forms. Peak blood levels occur about 1 to 2 hours after ingestion, and the vitamin is cleared primarily by the kidneys. Biotin’s elimination half-life in healthy adults is 8–24 hours, but this can be significantly longer in older adults or people with reduced kidney function.
A key clinical study (PMID: 34736903) found that even after stopping 10,000 micrograms of biotin, blood levels remained high enough to interfere with immunoassays for up to 72 hours. In people with impaired kidney clearance, this window may extend to four or even five days. The timeline to see normal, biotin-free lab results is thus highly individualized. For most healthy adults, pausing biotin for 72 hours is sufficient, but for older adults or anyone with kidney issues, extending the pause to 96 hours is safer.
The dose-response relationship is clear: the higher your daily dose, the longer it takes to clear. People taking only 2,500 micrograms (typical hair/nail doses) may clear biotin in 48 hours, while those on 10,000 micrograms or more need the full 72 hours. If you use extended-release or liposomal forms, clearance may be further delayed due to slower absorption and release. This timing principle is especially important before medical checkups, so you get data that truly reflects your health. Now that you know the timeline, you can plan your supplement routine around lab appointments and avoid false alarms.
The risk of biotin’s lab interference is not the same for everyone. Women of childbearing age, older adults, and people with neurological diseases are most affected. Studies show that women are more likely to use high-dose biotin for hair, skin, and nail benefits, often exceeding 5,000 micrograms per day. In pregnancy, marginal biotin deficiency is actually more common (PMID: 28701385), but supplementation above 1,000 micrograms is rare in prenatal formulas. Older adults are at special risk because kidney function naturally declines with age, slowing the clearance of biotin and extending its interference window.
People with multiple sclerosis or certain rare metabolic disorders may be prescribed pharmaceutical-grade biotin at doses of 100,000 micrograms or higher. At these levels, even five days off biotin may not fully clear the system. Children are less likely to take high doses, but some pediatric metabolic therapies use very high amounts, demanding extra caution with lab tests. Racial and ethnic differences in biotin clearance have not been strongly established, but body weight and muscle mass may play minor roles in how long biotin lingers.
Early warning signs of biotin interference can include an unexpected lab report showing low TSH or suspiciously high vitamin D, especially if you feel fine and have no symptoms of hormone imbalance. If you are in a high-risk group and take supplements regularly, always tell your laboratory about your use before any testing. Understanding these demographic nuances ensures you can personalize your supplement strategy for safe and reliable healthcare decisions.
When it comes to biotin, more is not always better. Clinical studies suggest that doses of 2,500–5,000 micrograms daily are sufficient for most hair and nail benefits, with minimal risk of lab interference if you follow proper timing. Higher doses, such as 10,000 micrograms, are popular in some beauty formulations, but research shows no extra benefit for most users—and a much higher risk of distorting lab results.
The form of biotin matters, too. Standard biotin tablets and capsules have nearly 100% bioavailability, with rapid absorption and clearance. Liposomal or enteric-coated forms may slow absorption, potentially extending the time biotin remains in your blood. There is no evidence that one form reduces the risk of lab interference compared to another. Stacking biotin with other B vitamins or supplements does not alter the risk either, as biotin does not compete for the same transporters or metabolic pathways. However, combining biotin with chromium picolinate has been shown in RCTs to improve glycemic control in people with type 2 diabetes (PMID: 17506119), though this is unrelated to lab interference.
To maximize benefits and minimize risks, use the lowest effective dose and choose simple formulations. For hair and nail support, 2,500 micrograms once daily is effective for most adults. Always pause supplementation for three days before any blood draw—longer if you use time-release forms or have slower kidney function. This approach lets you enjoy the upside of biotin while protecting the accuracy of your health data.
Biotin is often included in B-complex formulas and is sometimes paired with nutrients like zinc, silica, or collagen for hair and nail health. Mechanistically, biotin serves as a cofactor for carboxylase enzymes involved in fatty acid synthesis and amino acid metabolism (PMID: 40854404). Stacking biotin with other B vitamins does not reduce lab interference, as each B vitamin uses separate absorption mechanisms.
However, biotin does show synergistic effects with chromium picolinate for blood sugar regulation. A 90-day RCT (PMID: 17506119) showed that combining biotin (600 micrograms) with chromium picolinate (600 micrograms) led to a significant drop in HbA1c among people with type 2 diabetes. The dose-response relationship was clear in these trials—higher doses beyond 1,000 micrograms did not further improve blood sugar but did increase the risk of lab assay interference.
When stacking, be aware that some supplements may delay biotin clearance. Fatty meals can increase absorption, and time-release formulations prolong its presence. No known supplement reduces biotin’s impact on immunoassays. For optimal synergy and safety, combine biotin with complementary nutrients only if you can pause the stack before lab work. This ensures you get the most benefit while still getting accurate medical information.
If you use biotin supplements, planning ahead for blood tests is essential. The first step is to identify the dose and form you are using. For standard tablets (2,500–5,000 micrograms), stop biotin at least 72 hours before your scheduled blood draw. For higher doses or time-release forms, extend the pause to 96 hours. If you are unsure about your kidney function, err on the side of a longer washout.
Next, check which biomarkers your test will include. If your lab work includes TSH, free T4, free T3, 25-hydroxy vitamin D, PTH, or cardiac markers, biotin interference is a serious concern. Even if your panel seems routine, biotin can skew results for a range of tests, including some hormone, allergy, and infection markers. Communicate your supplement use to your laboratory at check-in, so they can flag your sample for potential interference if needed.
After your blood draw, you can resume your usual biotin regimen. If your results are surprising or do not match your symptoms, consider repeating the test after a full biotin washout. This protocol is your best defense against misdiagnosis and unnecessary treatment, ensuring that your lab results reflect your true health—not just your supplement routine.
Sometimes, despite your best efforts, you may encounter unexpected lab results. Red flags include a lab report showing a suppressed TSH with normal or high free T4, or a vitamin D level far higher than you’d expect from your supplement dose. If you feel well and have no symptoms of thyroid or vitamin D issues, consider biotin interference as a likely reason.
If you’re in a high-risk group—such as women using high-dose beauty supplements, older adults, or anyone on high-dose biotin for medical reasons—take these warning signs seriously. The first step is to pause all biotin supplementation for 72–96 hours, then repeat the relevant tests. In most cases, lab values will return to baseline, confirming that the previous results were false positives or negatives due to biotin.
If you have a complex medical history or take multiple supplements, keep a record of your dosing and timing. Share this with your healthcare team as needed. Early recognition and action can prevent a cascade of unnecessary tests, treatments, or anxiety. Knowing what to look for—and what steps to take—empowers you to stay in control of your health data.
Why Your Biotin Supplement Might Be Sabotaging Your Lab Results
How high-dose biotin creates false hormone and vitamin D readings—and what to do about it
Diagram glossary
- Biotin:
- A B-vitamin often used in supplements that can interfere with certain laboratory immunoassays.
- mIU/L:
- Milli-international units per liter, a standard unit of measurement for blood hormone levels.
- ng/mL:
- Nanograms per milliliter, a standard unit of measurement for concentration in blood tests.
- PMID:
- A unique reference number assigned to every article published in the PubMed database.
- proBNP:
- A protein biomarker measured in blood to help diagnose and evaluate heart failure.
- PTH:
- Parathyroid hormone, a substance produced by the parathyroid glands to regulate blood calcium.
- TSH:
- Thyroid-stimulating hormone, a pituitary hormone that regulates the production of thyroid hormones.
Conclusions
Biotin’s benefits for hair, skin, nails, and metabolism are well-supported at moderate doses. However, its unique ability to interfere with common lab assays makes supplement timing critical for anyone who relies on blood tests for health monitoring. By understanding the mechanisms, timelines, and risk factors, you can use biotin safely without jeopardizing the accuracy of your hormone or vitamin results. For most adults, pausing biotin for 72 hours before lab work is enough to avoid false readings. Stay aware, plan ahead, and enjoy the benefits of this B-vitamin without the risk of medical misdiagnosis.
While the evidence for biotin’s assay interference is robust, most studies focus on short-term, high-dose supplementation. There is limited data on chronic low-dose use, especially in populations with kidney or liver disease. Not all lab assays use the streptavidin-biotin system, so interference risk varies by laboratory and test manufacturer—details that are not always disclosed to patients. Individual differences in absorption and clearance are not fully understood, especially in children, pregnant women, or people with rare genetic conditions. Future research should clarify the minimum effective dose for benefits, the safest washout periods for different demographics, and develop lab technologies immune to biotin interference.
Track this in your stack
See how biotin relates to your health goals and monitor changes in your biomarkers over time.
