Your Cortisol Rhythm Is a Fingerprint — And Most People Are Reading It Wrong
Why timing matters more than levels when measuring your stress hormone
You might think of cortisol as a single number on a lab report — too high or too low, good or bad.
But your cortisol is actually a living fingerprint that shifts hour by hour, shaping your energy, focus, and sleep. Understanding your true cortisol rhythm, not just a snapshot, is the key to unlocking better rest and a healthier stress response. Let’s dig into why most people get this wrong, and what it takes to measure and optimize your real cortisol pattern.
- Hair cortisol
- A lab test using a small hair sample to estimate average cortisol exposure over about 2–3 months.
- Cortisol Awakening Response (CAR)
- The jump in cortisol after you wake. Often measured at wake time and 30 minutes later.
- Late-night salivary cortisol
- A bedtime saliva measure. Higher-than-expected levels can align with insomnia and a “wired at night” pattern.
- Salivary cortisol
- Cortisol measured in saliva. It mainly reflects free (active) cortisol and can be collected at home.
- HPA Axis
- The body's central stress response system connecting the brain to adrenal glands. Chronic activation leads to elevated stress hormones and negative health effects.
- Corticosteroid-binding globulin (CBG)
- A blood protein that binds most cortisol. Higher CBG can make total cortisol look high while free cortisol stays normal.
- Diurnal cortisol slope
- How fast cortisol drops from morning to night. A flatter slope can signal dysregulation.
- CBG
- Corticosteroid-binding globulin is a blood protein that binds cortisol, limiting its active tissue exposure.
- estrogen
- A hormone whose fluctuating levels can shift the amount of corticosteroid-binding globulin in blood.
- HPA
- The hypothalamic-pituitary-adrenal axis is a bodily system that ramps up daily cortisol production.
Picture this: your alarm goes off, you roll out of bed, and you already feel behind. Maybe you reach for coffee or wonder why you’re sluggish even after a full night’s sleep. Or maybe you’re wide awake at midnight, staring at the ceiling, your mind racing while your body refuses to settle down. If you’ve ever had a doctor check your cortisol, you probably got just one result. Maybe it was flagged as high or low, and you were left with more questions than answers. Here’s the truth — your experience of energy, alertness, and even sleep quality is shaped not by a single cortisol number, but by the unique rhythm your body creates across the day.
Think of cortisol like the conductor of your body’s orchestra. It sets the tempo for how you wake up, handle stress, and wind down for sleep. But most of us are only seeing a single note, not the full symphony. This is why so many people feel dismissed or confused by standard testing. The real story is about your personal cortisol fingerprint, and learning to read it can change how you feel from morning to night. So how does this rhythm actually work, and why does it matter for your daily life? Let’s start with what makes cortisol tick.
Cortisol is your body’s main stress hormone, but it is also tightly tied to your internal clock, known as the circadian rhythm. Every cell in your body listens to this clock, and cortisol is one of the loudest signals it sends. In a healthy system, cortisol is supposed to spike quickly after you wake up. This is called the cortisol awakening response. It gets you moving, helps you focus, and primes your body for action. After this morning surge, cortisol should fall steadily as the day goes on, reaching its lowest point near bedtime. This sharp drop is the signal that tells your brain and body it’s time to rest and recover.
Why does this pattern matter? If your cortisol stays too high in the evening, you may feel wired but tired — exhausted but unable to sleep. If your morning rise is weak, you might drag through the day, struggling with motivation and mental clarity. The timing, not just the amount, of cortisol affects everything from memory to metabolism. That’s because cortisol helps regulate blood sugar, reduces inflammation, and communicates directly with your brain’s sleep centers.
Disruptions to this rhythm are linked to real health consequences. Research shows that people whose cortisol curves flatten out over time — meaning less difference between morning and night — are at higher risk for depression, cognitive decline, and even heart disease. Your body needs a strong signal for day and a clear signal for night. When the pattern blurs, your stress system and your sleep system both suffer.
So what does a healthy cortisol day look like? And how do you know if your rhythm is on track? That brings us to how you can actually measure your unique cortisol fingerprint.
Most people think of cortisol testing as a single blood draw, but this approach tells you almost nothing about your daily rhythm. The real power comes from mapping how your cortisol changes throughout the day. Here’s how to do it right.
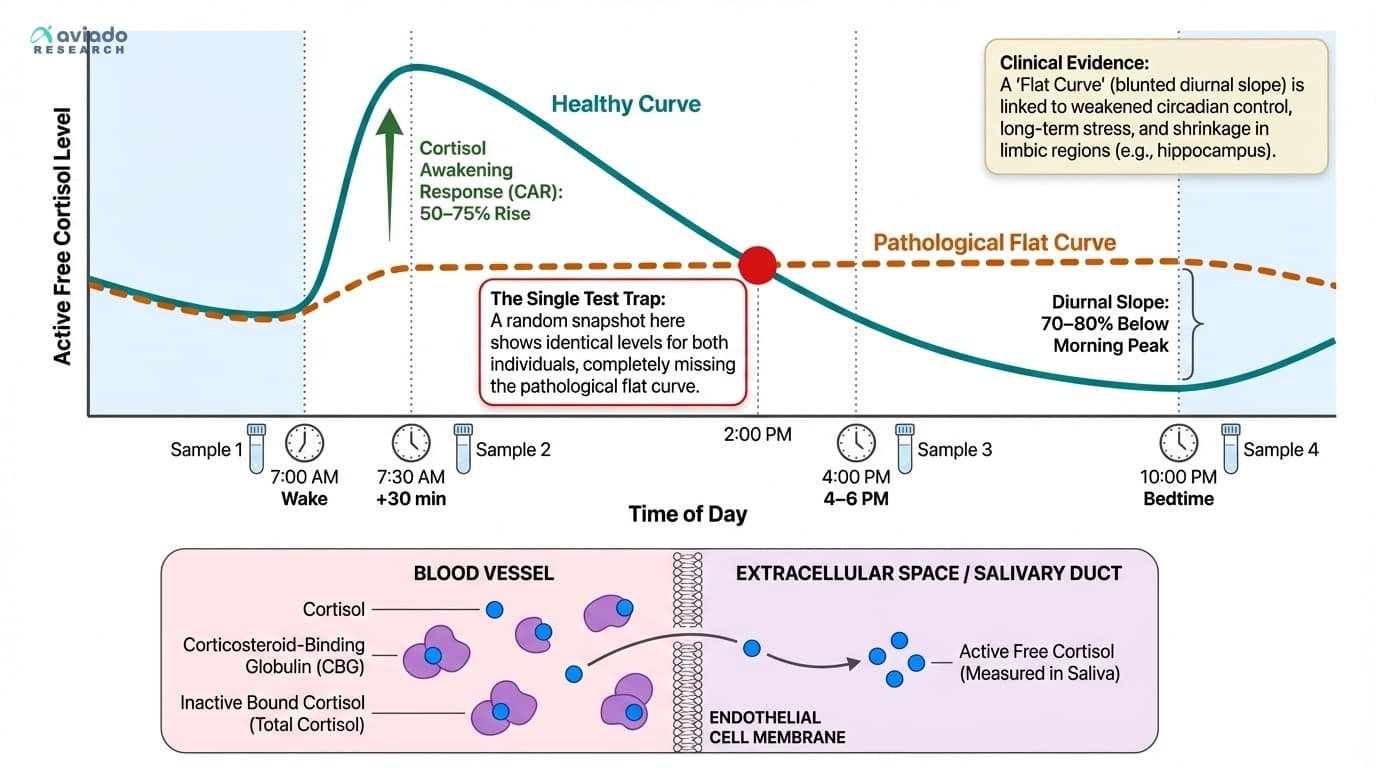
Researchers and progressive clinics use a four-point saliva test. You collect saliva samples at four key times: immediately after waking, thirty minutes after waking, late afternoon — usually between four and six PM — and at bedtime. This pattern captures your cortisol awakening response, your afternoon dip, and your night-time low. The science says you should see a rise of about fifty to seventy-five percent in the first thirty minutes after waking. By bedtime, your level should have dropped by seventy to eighty percent compared to your morning peak.
Why saliva? Unlike blood, where most cortisol is bound to carrier proteins and not active, saliva shows only the free, active cortisol that actually reaches your tissues. This means saliva testing reflects the hormone that is doing real biological work in your body. Blood tests can be misleading, because changes in carrier proteins — which can fluctuate with estrogen, inflammation, or liver health — don’t always change your active cortisol.
What if your curve is flat? This is where things get interesting. A flat curve means your cortisol does not drop enough from morning to night. You might think low cortisol is always good, but the science says otherwise. Studies in older adults show that a flatter daily curve, even when values are technically normal, is linked to poorer memory and shrinkage in brain regions like the hippocampus. In people with chronic stress or mood issues, a flat curve often means your stress system is always on, but never surging or resting properly.
So when you measure, don’t just look for highs or lows. Look for a strong morning rise and a steady decline. That pattern is your fingerprint of a healthy stress response, and it’s what you want to protect or restore. So how do you actually measure all this at home or with your doctor? And what do you do if your pattern is off? Let’s get practical.
If you want to map your cortisol rhythm accurately, you need to follow a clear protocol. Start with a four-point saliva collection on a typical day. Here’s how to do it: collect your first sample immediately upon waking, before you even get out of bed. The second comes thirty minutes later. The third should be in the late afternoon, between four and six PM. The fourth is right before bedtime. To keep results reliable, avoid eating, drinking alcohol, smoking, or brushing your teeth for at least thirty minutes before each sample. Only drink water if needed. Try to choose a day when you’re not sick, traveling, or under unusual stress.
If you want to see a more stable picture, repeat this test on two or three typical days and look for patterns. The goal is to see a pronounced rise after waking, then a gradual decline. If your bedtime sample is higher than expected, or if the decline is small, this suggests a flat curve.
What if your numbers are off? First, remember that context matters. A single stressful event, poor sleep, or travel can shift your curve temporarily. But persistent patterns — like a weak morning rise or a stubbornly high evening value — deserve attention.
Intervention starts with understanding why your curve might be disrupted. Poor sleep timing, lack of morning light, irregular meal times, and chronic stress all push your rhythm off course. Some people also have underlying medical issues like sleep apnea, depression, or thyroid dysfunction that flatten or distort cortisol patterns. The first step is always to address lifestyle and sleep hygiene, but there are targeted supplements that can help regulate your rhythm too. Let’s look at the evidence for those next.
When it comes to supplements for cortisol, the goal is to support your natural rhythm — not to blunt cortisol across the board. You want a strong morning surge and a clear drop at night. Here are some evidence-backed options and how they work.
Phosphatidylserine is one of the best-studied supplements for lowering elevated evening cortisol. Multiple trials have shown that taking three hundred milligrams in the evening can reduce night-time cortisol and improve sleep quality. The mechanism here involves phosphatidylserine’s ability to dampen the overactivity of the hypothalamic-pituitary-adrenal (HPA) axis, which is your body’s main stress signaling system.
Ashwagandha, an adaptogenic herb, has been shown in randomized controlled trials to reduce overall cortisol by fifteen to thirty percent in people under chronic stress. The typical dose is three hundred to six hundred milligrams of a root extract, taken in the morning or early afternoon. Ashwagandha seems to work by reducing the sensitivity of your stress receptors and modulating the feedback loop that tells your body when to dial down cortisol production.
Magnesium is another key player, especially for those with sleep issues and evening cortisol elevations. Magnesium supports the enzymes that break down cortisol and helps relax your nervous system. A dose of two hundred to four hundred milligrams in the evening, preferably as magnesium glycinate or magnesium threonate, can help you wind down and reduce sleep-disrupting spikes.
Melatonin, taken thirty to sixty minutes before bed, does not directly lower cortisol, but it helps reinforce your body’s natural night signal, encouraging cortisol to drop as it should. Doses of point three to two milligrams are effective for most people.
Finally, vitamin B5 and vitamin C are important for adrenal health. Both are needed for cortisol synthesis, but also help prevent overproduction during times of chronic stress. Supplementing with five hundred milligrams of vitamin C and one hundred to two hundred milligrams of vitamin B5 daily can help buffer your stress response without pushing cortisol too low.
It’s important to remember that supplements are not a substitute for good sleep, regular light exposure, and stress management. Think of them as support, not a cure. So what lifestyle changes matter most for keeping your cortisol fingerprint healthy? Let’s dig into those next.
Your daily habits are the strongest levers for shaping your cortisol curve. The first and most powerful is your exposure to natural light. Your internal clock is set by the light you see in the morning. Make it a priority to get outside for at least fifteen to thirty minutes soon after waking. This morning light tells your brain to ramp up cortisol, boosting your alertness and mood for the day. It also helps your body know when to start winding down later.
Consistent sleep and wake times are the next big player. Your cortisol rhythm depends on regular signals. Try to go to bed and get up at the same time each day, even on weekends. When your schedule is erratic, your cortisol curve gets fuzzy, making it harder to feel rested or focused.
Movement matters too. Moderate exercise in the morning or early afternoon helps reinforce your natural cortisol peak. Regular physical activity reduces stress hormone output over time and strengthens the signal for a night-time drop. On the other hand, intense exercise late in the evening can keep cortisol elevated and disrupt sleep.
Nutrition plays a role as well. Eating regular, balanced meals — especially breakfast — helps anchor your daily rhythm. Skipping meals or eating large, high-sugar snacks late at night can push your cortisol curve in the wrong direction, leading to higher night-time levels. Focus on whole foods, plenty of fiber, and adequate protein to stabilize blood sugar and cortisol.
Stress management is the final lever. Chronic psychological stress flattens your cortisol curve, making it hard to recover or sleep well. Practices like mindfulness, deep breathing, or even a ten-minute walk outdoors can help reset your stress system, especially in the afternoon and evening. If you find yourself stuck in a cycle of worry or busyness late at night, try swapping screen time for calming activities that help signal your brain to ease off the gas pedal.
These habits do not just improve your cortisol rhythm. They also make your entire stress and sleep system more resilient. So what should you watch out for if your curve is off track? Here are the early warning signs your cortisol rhythm needs attention.
How do you know if your cortisol rhythm has drifted out of balance? Listen to your body’s signals. The most common red flag is trouble waking up, even after a full night’s sleep. If you feel groggy, unmotivated, or in need of caffeine to get started, your morning cortisol surge may be blunted. This can leave you dragging through the day, with trouble focusing or getting things done.
On the flip side, if you feel wired at night — restless, anxious, or unable to fall asleep — your cortisol may be staying too high in the evening. Night-time awakenings, especially between one and three AM, are also a classic sign of a disrupted cortisol drop. You might wake up feeling alert, even though you know you should be asleep.
Mood changes are another clue. Chronic irritability, low mood, or feeling emotionally flat can link back to a flattened cortisol curve. Memory lapses and brain fog often show up when your stress system is running on empty or stuck in the on position.
Physical signs matter too. Unexplained weight gain, especially around the midsection, and cravings for sugar or salty foods can signal that your cortisol rhythm and your metabolic system are out of sync. Frequent infections, slow recovery from illness, or persistent aches and pains may also reflect a stress system that is not getting the rest it needs overnight.
If you notice these signs, it’s time to look at your cortisol rhythm alongside your sleep, nutrition, and stress patterns. Early action gives you the best shot at restoring a healthy, dynamic curve before more serious problems develop. So what is the big picture when it comes to your cortisol fingerprint, and what should you do next? Let’s bring it all together.
Cortisol is not just a stress hormone or a single lab result. It is your body’s way of marking the passage of each day, guiding your energy, focus, and rest. Understanding your unique cortisol fingerprint means looking at the pattern, not just the peaks and valleys. By measuring at multiple times, using saliva instead of blood, and watching for a strong morning rise and steady evening drop, you get a real map of how your body handles stress and recovery.
The good news is, you can shape your rhythm. Light, sleep routines, nutrition, movement, and targeted supplements all work together to support a healthy curve. The payoff is better sleep, clearer thinking, steadier mood, and long-term protection for your brain and heart.
If you feel stuck, start by tracking your sleep, morning energy, and night-time restlessness. Then move to testing your full cortisol curve. Use what you learn to adjust your habits and, if needed, layer in supplements. Remember, your cortisol rhythm is not fixed. With the right information and small, steady changes, you can rewrite your daily signature and unlock better health, one day at a time.
Your Cortisol Rhythm Is a Fingerprint — And Most People Are Reading It Wrong
Why timing matters more than levels when measuring your stress hormone
Diagram glossary
- CBG:
- Corticosteroid-binding globulin is a blood protein that binds cortisol, limiting its active tissue exposure.
- estrogen:
- A hormone whose fluctuating levels can shift the amount of corticosteroid-binding globulin in blood.
- HPA:
- The hypothalamic-pituitary-adrenal axis is a bodily system that ramps up daily cortisol production.
Conclusions
Cortisol works like a schedule, not a score. The most useful question is not “Is my cortisol high?” It is “Does my cortisol rise after waking and fall by bedtime?” Use multi-time-point saliva testing to see your daily shape. Add hair cortisol if you need a longer view of chronic exposure. Treat results as pattern data, then target sleep timing, light, and daily stress load to shift the curve.
Cortisol patterns vary by age, sex, genetics, shift work, sleep timing, and medications (including steroids and estrogen-containing contraceptives). Many studies report group averages, so your “normal” may differ. Home saliva tests can be thrown off by timing mistakes, food, nicotine, tooth brushing, and poor sleep the prior night. Hair cortisol can be affected by hair treatments, hair growth differences, and lab methods, and it cannot show morning-versus-night timing problems. These tests do not diagnose medical disease; unusual results should be reviewed with a clinician, especially if symptoms suggest adrenal or pituitary disorders.
Track this in your stack
See how cortisol relates to your health goals and monitor changes in your biomarkers over time.
