Your Homocysteine Level Is a Personal Report Card on Your Methylation Genetics — Here's How to Read It
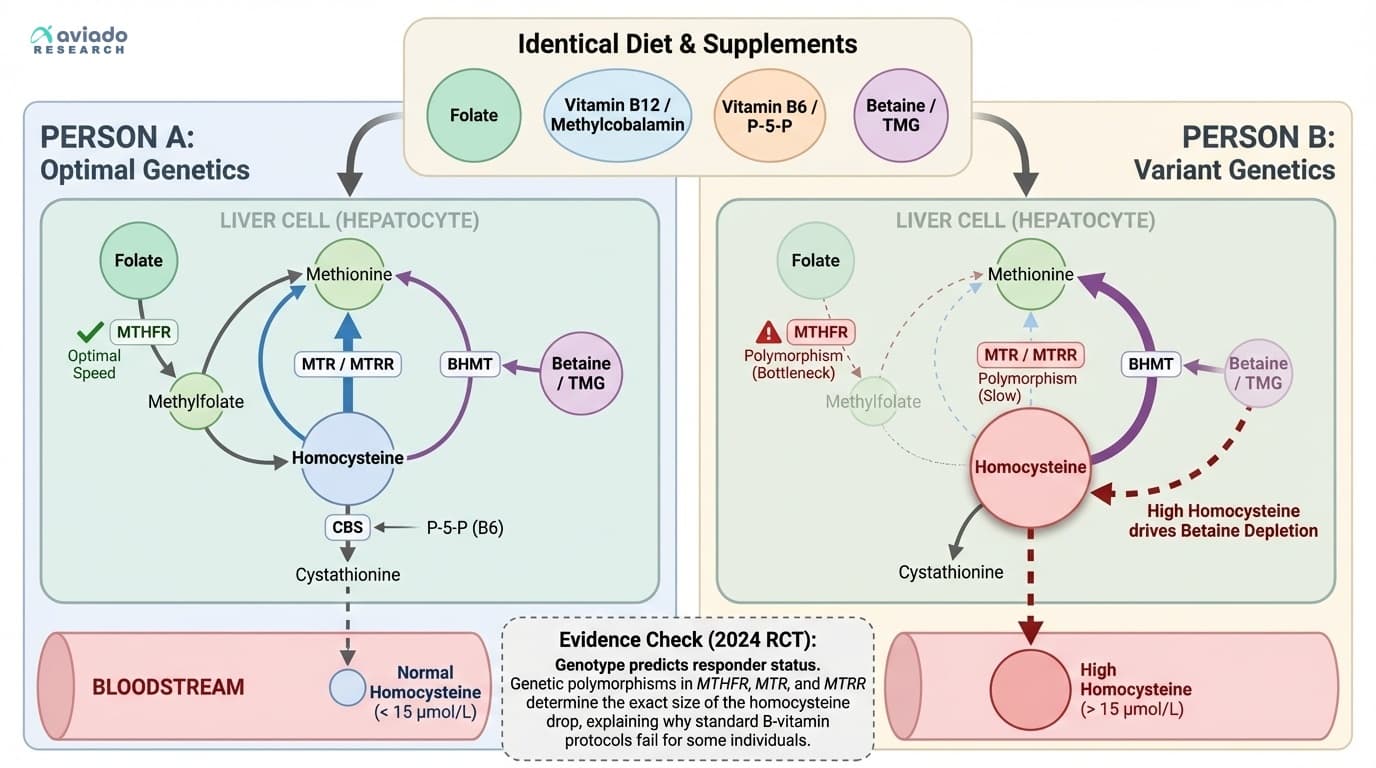
Why two people with identical diets and supplements can have wildly different homocysteine levels
Imagine your blood test as a personalized report card, telling you how efficiently your body's internal chemistry runs.
Homocysteine is more than just a number—it's a direct reflection of how well your genes handle one of the most fundamental metabolic cycles: methylation. Understanding what your homocysteine level says about your health, and how you can influence it, gives you a practical advantage for long-term well-being.
- MTHFR (C677T, A1298C)
- Common gene variants that can reduce your ability to make active folate (5-MTHF). This can raise homocysteine in some people.
- MTR and MTRR
- Genes that help use vitamin B12 to remethylate homocysteine back to methionine. Variants can change how well B12-based remethylation works.
- Homocysteine
- Homocysteine, an amino acid metabolite influenced by B vitamins. elevated levels damage blood vessels and increase cardiovascular and dementia risk.
- Methylcobalamin
- An active form of vitamin B12 used in the MTR reaction. It can be more directly usable than cyanocobalamin for some people.
- Folic acid vs methylfolate (5-MTHF)
- Folic acid is a synthetic form that must be converted. Methylfolate (5-MTHF) is the active form and can bypass MTHFR limits.
- Betaine (TMG) and the BHMT pathway
- Betaine, also called trimethylglycine (TMG), supports an alternate liver pathway (BHMT) that remethylates homocysteine without folate/B12.
- Pyridoxal-5'-phosphate (P-5-P)
- The active form of vitamin B6. It supports the “transsulfuration” route that helps clear homocysteine.
- adenosylmethionine
- A primary methyl donor molecule involved in cellular methylation reactions.
- B12
- An essential vitamin required for remethylating homocysteine back into methionine.
- B6
- An essential vitamin whose active form helps metabolize homocysteine.
Picture this. You are sitting in your car, headed to work, or maybe you are out for a walk with your favorite playlist. Your mind drifts to that annual blood test you just got back. There is a number you have probably never thought about: homocysteine. The lab flagged it as 'borderline high.' Maybe your doctor shrugs it off or mentions B vitamins. But you cannot shake the feeling that there is more to the story.
This is not just about hitting a target on a lab form. This number tells you how well your body runs one of its most important chemical cycles, called methylation. It is like a report card for your inner engine. Two people can eat the same food, take the same vitamins, and end up with totally different results. That is not random. It is a signal from your genes—and your choices—that you can interpret and act on.
Think of your homocysteine level as a check engine light. It does not just mean you are missing a vitamin here or there. It is a reflection of how your unique biology is handling the pressure of daily life, stress, and even aging. For many people, a high homocysteine is the first clue that something deeper is going on. So what does this number really mean, and how can you use it to optimize your health? That is exactly where we are headed.
Homocysteine is an amino acid, a small molecule your body produces every day as it processes protein. But it is not just a waste product. It sits at the crossroads of a chemical pathway called the methylation cycle. This cycle helps your body build DNA, make neurotransmitters, repair cells, and detoxify hormones and chemicals. When methylation runs smoothly, homocysteine gets recycled back into methionine, a building block for many vital functions.
Here is where your genes come in. Several enzymes control methylation, and each is coded by your DNA. The star of the show is a gene called MTHFR. It stands for methylenetetrahydrofolate reductase, and it helps convert folate from food into the active form your body needs. If you have a common variation in MTHFR, your enzyme works more slowly. That means your body may struggle to process folate efficiently, and homocysteine can start to rise.
But MTHFR is only one piece. Two other genes, MTR and MTRR, control steps that require vitamin B12. These enzymes help add a methyl group—a tiny chemical tag—to homocysteine, transforming it back into methionine. If you have variations in these genes, you may need more or different forms of B12 to keep the cycle moving.
It is not just about genetics. Age, stress, medications, and even sex hormones can influence methylation. For example, estrogen boosts methylation efficiency, which is why premenopausal women often have lower homocysteine than men or postmenopausal women. As you age, your enzyme activity naturally slows, making optimization even more important.
When homocysteine builds up, it is more than a lab curiosity. High levels can damage blood vessels, increase inflammation, and disrupt brain chemistry. For you, this could mean higher risk for heart disease, cognitive changes, fertility struggles, or even mood shifts. The bottom line: your homocysteine level is a living snapshot of how your genes, nutrients, and lifestyle intersect. So how do you read your score? That brings us to the practical side.
The first step is to know your number. A fasting homocysteine blood test is widely available and costs less than most specialty markers. But understanding the result is where most people get stuck.
Most labs list anything below fifteen micromoles per liter as 'normal.' But research paints a different picture. Studies in heart health, fertility, and cognitive aging show risk can rise long before you hit that cutoff. For optimization, aiming for a homocysteine level below ten, and ideally between six and eight micromoles per liter, is more protective.
Why does this matter? In a 2023 study of women undergoing fertility treatments, even small increases in homocysteine—still within the lab reference range—were linked to higher rates of failed IVF cycles. For cardiovascular health, a level above ten consistently tracks with higher risk of heart attack and stroke. For brain health, higher homocysteine can accelerate cognitive decline by promoting inflammation and oxidative stress.
Where does your homocysteine come from? About seventy to eighty percent is produced in your liver, through the metabolism of methionine, an amino acid from protein. Your body can clear homocysteine in two main ways. One route relies on folate and B12, using the MTHFR, MTR, and MTRR enzymes to remethylate homocysteine back to methionine. The other route uses an enzyme called BHMT, which operates mainly in the liver and depends on a nutrient called betaine (also known as trimethylglycine).
If your folate and B12 intake are normal but your homocysteine is still high, your liver's BHMT pathway may be under strain. This is common in people with fatty liver, metabolic syndrome, or high alcohol intake. It is also why some people see little change with B vitamins alone—the backup system needs support.
So what does your number mean? If you are above ten, your methylation cycle is struggling. If you are between eight and ten, you are in a gray zone where small tweaks can still pay big dividends. Below eight is an optimal target for most adults looking to lower long-term risk. Knowing where you stand helps you personalize your next steps.
Once you know your homocysteine level, you have a starting point. But lowering it is not as simple as grabbing a generic B vitamin from the store. The form and dose matter—and your genes influence what works best for you.
A landmark randomized controlled trial published in 2024 looked at more than two thousand adults and tested a combination of methylfolate, methylcobalamin (the active form of B12), and P-5-P (the active form of B6). Researchers found that everyone’s homocysteine dropped, but the amount of change depended on their specific genetic variants. People with MTHFR mutations needed methylfolate to see a meaningful reduction. Those with MTR or MTRR variants responded better when methylcobalamin was included. The key takeaway: active forms of B vitamins work better than standard folic acid or cyanocobalamin, especially if you have common gene variations.
So how do you put this into action? Start with methylfolate at four hundred to eight hundred micrograms daily. This covers most needs and bypasses sluggish MTHFR enzymes. Add methylcobalamin at one thousand micrograms daily. This supports the B12-dependent step that remethylates homocysteine. Include P-5-P, the active form of B6, at twenty-five to fifty milligrams daily. B6 helps your body break down homocysteine through an alternate pathway.
If your homocysteine stays high after eight to twelve weeks, consider adding betaine. Start with five hundred to one thousand milligrams, taken twice daily. Betaine works through the BHMT pathway in your liver, offering a backup route when the folate-B12 system is slow. This is especially helpful if you have fatty liver, are middle-aged or older, or have not responded to B vitamins alone.
Each supplement targets a specific mechanism. Methylfolate and methylcobalamin feed the primary remethylation pathway. P-5-P keeps the transsulfuration route open for homocysteine breakdown. Betaine supports the liver’s backup system, especially when methylation is under extra stress. Retest your homocysteine after eight to twelve weeks to see your progress. If you are not at your target, you can fine-tune from there.
Supplements can move your numbers, but your daily choices are just as powerful in optimizing homocysteine. Every part of your lifestyle, from what you eat to how you sleep, interacts with your methylation cycle.
Start with your plate. Leafy greens and cruciferous vegetables are rich in natural folate and betaine. Think spinach, arugula, broccoli, and beets. Eating these daily supplies your body with the raw materials for methylation. Eggs and seafood are excellent sources of B12 and choline, another key methyl donor. Whole grains, legumes, and seeds provide B6, zinc, and magnesium, all of which support methylation enzymes.
Protein matters too, but more is not always better. Excess animal protein increases methionine intake, which can raise homocysteine if you are not getting enough B vitamins and betaine to process it. Balance your protein sources, and include plant-based meals to support overall methylation balance.
Alcohol is a wildcard. Even moderate drinking can deplete folate and B vitamins, raising homocysteine. If you are working to optimize your number, consider cutting back significantly or taking breaks to let your methylation system recover.
Physical activity is a natural methylation booster. Regular aerobic exercise—think brisk walking, jogging, cycling, or swimming—has been shown to lower homocysteine by increasing blood flow and supporting liver health. Aim for at least one hundred fifty minutes per week, broken into sessions that fit your schedule. Strength training also helps, especially as you age, by preserving muscle mass and improving insulin sensitivity, both of which support healthy methylation.
Sleep is often overlooked, but deep, restorative rest is when your body does most of its repair work, including methylation. Aim for seven to nine hours per night. Chronic sleep deprivation raises stress hormones like cortisol, which can slow methylation and push homocysteine higher.
Stress management is not just about feeling better—it is biochemistry. Meditation, mindful breathing, and time in nature have all been shown to reduce stress hormones and support methylation. Chronic psychological stress can deplete B vitamins and increase homocysteine.
Lifestyle changes work by supporting your body’s natural enzyme systems and providing the nutrients needed to keep methylation running smoothly. When you combine these with targeted supplementation, you create the conditions for long-term optimization.
Homocysteine does not cause obvious symptoms until it has been high for years, but your body often gives subtle clues. Recognizing these early warning signs can help you intervene before problems become entrenched.
You might notice unexplained fatigue, brain fog, or mood swings. These can be signs that your methylation cycle is struggling, especially if your diet and sleep are otherwise good. New onset of headaches, especially migraines, has been linked to elevated homocysteine. Some people experience tingling in the hands or feet, which can signal B12 deficiency and impaired methylation.
If you have a family history of heart disease, stroke, or early cognitive decline, pay close attention to your homocysteine. Elevated levels can silently damage blood vessels and increase clotting risk. In women, difficulty conceiving or repeated miscarriages may be linked to methylation issues and high homocysteine, even if other tests are normal.
Certain medications can raise homocysteine. These include common drugs like metformin, proton pump inhibitors, and some anti-seizure medicines. If you are taking any of these, it is worth checking your level annually and supplementing as needed.
If you have already been diagnosed with high cholesterol, hypertension, or fatty liver, you are at higher risk for methylation imbalance. These conditions often go hand in hand with elevated homocysteine. The earlier you check and correct, the better your long-term outlook.
When should you take action? If your homocysteine is above ten, or if you have symptoms and risk factors, do not wait for your doctor to suggest a plan. Start with the lifestyle and supplement strategies discussed here, and retest after a few months. If you see improvement, keep going. If your number stays high, consider genetic testing to personalize your approach further.
Your homocysteine level is more than a single digit on your lab report. It is a dynamic scorecard, reflecting how well your genes, nutrients, and lifestyle are working together to support your health. Understanding this number gives you a direct line to some of the body’s most essential processes—DNA repair, neurotransmitter balance, vascular health, and detoxification.
The science is clear. Optimizing your methylation through targeted B vitamins, betaine, and supportive lifestyle choices can lower your homocysteine and tilt the odds toward better long-term health. The most important step is to measure, personalize, and track your progress. Do not settle for 'normal' if your goal is lifelong vitality.
You have more control than you think. Whether your homocysteine is already high, or you simply want to future-proof your health, the path is the same: test, intervene, and retest. Each adjustment you make is a vote for a healthier, more resilient you. Your next blood test is not just a report—it is your roadmap to action.
So as you finish your commute or wrap up your walk, remember: your biology is not destiny. It is a conversation, and you are always at the table. The best time to start optimizing is now. Your future self will thank you.
Your Homocysteine Level Is a Personal Report Card on Your Methylation Genetics — Here's How to Read It
Why two people with identical diets and supplements can have wildly different homocysteine levels
Diagram glossary
- adenosylmethionine:
- A primary methyl donor molecule involved in cellular methylation reactions.
- B12:
- An essential vitamin required for remethylating homocysteine back into methionine.
- B6:
- An essential vitamin whose active form helps metabolize homocysteine.
- BHMT:
- An enzyme that uses betaine to convert homocysteine into methionine.
- DNA:
- The molecule that carries genetic instructions for development and functioning.
- Homocysteine:
- An amino acid whose elevated levels indicate impaired methylation cycle function.
- IVF:
- A medical procedure where an egg is fertilized by sperm outside the body.
- MTHFR/MTR:
- Key genes and enzymes that regulate folate metabolism and homocysteine remethylation.
- MTR/MTRR:
- Genes and enzymes driving the B12-dependent step that remethylates homocysteine to methionine.
- P-5-P:
- Pyridoxal-5'-phosphate, the biologically active form of vitamin B6.
- SAM:
- S-adenosylmethionine, the principal methyl donor in cellular metabolic pathways.
- TMG:
- Trimethylglycine, or betaine, a compound that provides methyl groups to reduce homocysteine.
Conclusions
Homocysteine is not just a “B-vitamin number.” It is a live signal of how your methylation pathways are running, shaped by your genetics and your nutrient forms. If your goal is to improve the number, use a test-and-verify plan: check fasting homocysteine, use active B vitamins first, and then support the betaine-BHMT pathway if you plateau. Treat the lab reference range as a screening tool, not a personal target, and let your repeat results guide your next step.
Evidence for genotype-guided homocysteine treatment is promising but still limited. Many studies link homocysteine to outcomes, but lowering homocysteine does not always prove improved clinical endpoints in every population. The 2024 genotype-stratified findings need replication and clearer effect sizes by variant. “Optimal” targets likely differ by condition (cardiovascular, neurological, fertility) and are not settled. Betaine data also skew toward clinical or liver-focused settings, so dosing and long-term effects in generally healthy people are less certain. This article is educational and does not replace individualized medical care, especially for pregnancy planning or known B12 deficiency.
Track this in your stack
See how homocysteine relates to your health goals and monitor changes in your biomarkers over time.
Sources (8)
This article informs how supplementation moves 1 marker.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
