Your Inflammation Level Determines Whether Vitamin B6 Works — And Most People Never Check It
Why plasma PLP and inflammation markers are the hidden keys to vitamin B6 effectiveness
Imagine taking a vitamin every morning, believing it’s helping your body run smoother, only to learn it might be doing nothing for you at all.
The secret? Whether vitamin B6 works for you depends almost entirely on your body’s hidden inflammation level—a factor most people never check, but one that transforms B6 from a dud supplement into a powerful ally for your muscles, metabolism, and immune health. Today, you'll learn how to use your bloodwork to unlock the real benefits of B6, and when to skip it entirely.
- Pyridoxal 5'-phosphate (PLP)
- The active form of vitamin B6 in the body; critical because it's the form measured in blood to assess true B6 status and is directly depleted by inflammation.
- Advanced glycation end-products (AGEs)
- Harmful compounds formed when sugar binds to proteins or fats; B6 helps reduce AGEs, which is why it may help with blood sugar control.
- Pyridoxine HCl
- The most common supplement form of vitamin B6, used in research and over-the-counter products. Converts to PLP in the body.
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- Glucose
- Blood sugar level, the primary energy source for cells. Fasting glucose is normal, prediabetes, ≥126 suggests diabetes.
- One-carbon metabolism
- A set of biochemical pathways that use B6 for DNA and protein synthesis, with implications for cancer and metabolic disease.
- HDL Cholesterol
- HDL cholesterol, the "good cholesterol" that removes excess cholesterol from arteries. higher levels are cardioprotective.
- B6
- A vitamin whose active form, PLP, is rapidly depleted by bodily inflammation.
- CRP
- An inflammation marker in the blood that helps determine vitamin B6 supplement efficacy.
- HDL
- High-density lipoprotein, a beneficial cholesterol that transports other cholesterol to the liver.
Picture this: you’re starting your day, maybe on your way to work or walking your dog, and you reach for your daily multivitamin. You’ve read about all the benefits—better energy, stronger immunity, maybe even healthier skin. But have you ever wondered if that vitamin B6 in your supplement is actually doing anything for you? Most people never stop to ask. It’s easy to assume that if a nutrient is healthy, more must be better, right? But with vitamin B6, the story is a lot more personal than you’d expect.
The reality is that your body’s need for B6 is not fixed. It’s dynamic, changing with your stress levels, your immune system’s activity, and even your exposure to everyday infections or chronic health problems. Two people could eat the same food, take the same supplement, and see totally different results—all depending on something that never shows up on the label: inflammation.
You might be someone who feels fine, or maybe you notice more muscle soreness after workouts, slower recovery after being sick, or even unexplained fatigue. These are all situations where your body could be burning through B6 faster than usual. And if you’re not measuring what’s happening in your blood, you’ll never know if you’re running low or just wasting money on a supplement you don’t need. That brings us to the hidden world of inflammation and why it changes everything about vitamin B6.
So let’s get into the science—without losing sight of how this plays out in your own life. Your immune system is always on alert, scanning for threats. When it senses trouble—from an infection, a tough workout, or even chronic stress—it ramps up its activity. This process creates inflammation, which is your body’s way of fighting back. But here’s the catch: that same immune response burns through your stores of vitamin B6, especially the active form known as PLP, or pyridoxal 5'-phosphate.
It’s not a small change. When your body is inflamed, it can use up PLP at up to three times the normal rate. In practical terms, that means if you have a cold, a nagging injury, or even silent, low-level inflammation from things like excess body fat or poor sleep, your B6 needs go way up—without you ever realizing it. A landmark study published in Finland in 2024 followed over two thousand adults for five years. They found that people with high levels of CRP—a standard marker of inflammation—had PLP levels about forty percent lower than those with low inflammation, even though both groups ate the same foods and took similar supplements.
Why does this matter? Because low PLP isn’t just a lab number. It means your cells can’t run their energy cycles efficiently, your nerves become more sensitive to damage, and your immune system can’t regulate itself properly. That’s why inflamed people who are low on PLP often feel sluggish, get sick more often, or struggle with blood sugar swings. It also means that if you’re healthy, with normal PLP and low inflammation, piling on extra B6 will do almost nothing. Your body can’t use what it doesn’t need. So, before you even think about supplementation, you need to know your status—not just for B6, but for inflammation. That’s where bloodwork comes in.
Let’s talk about the two numbers that make or break your B6 strategy: PLP, the active form of vitamin B6 in your blood, and CRP, which stands for C-reactive protein, a key measure of inflammation. These are the tests that give you a real, actionable snapshot of whether your body actually needs more B6—or if you’re already topped up.
PLP, or pyridoxal 5'-phosphate, is the form of B6 your body actually uses in hundreds of metabolic reactions. Think of it as the currency your cells spend to keep your muscles working, your brain sharp, and your immune system balanced. If your PLP drops below thirty nanomoles per liter, you’re in functionally deficient territory. That means your body is running short on a nutrient it needs to repair tissue, process energy, and make neurotransmitters like serotonin and dopamine. If you’re above thirty, your B6 stores are probably healthy—adding more won’t make a difference.
Now, CRP is the other half of the equation. High-sensitivity CRP, or hs-CRP, is the gold standard for picking up even low levels of inflammation that you might not feel. Levels above one milligram per liter suggest your immune system is active. Above three milligrams per liter, and you’re in the range where inflammation is causing real changes to your B6 metabolism. Studies show that people with high CRP see their PLP levels plummet—even if they’re eating a healthy diet or taking a basic supplement.
So what does this look like in practice? If you have a PLP below thirty and a CRP above one, you’re exactly the person who will benefit from B6 supplementation. If both numbers are in the healthy range, save your money for something else. This is true even if you’re active, eat clean, or are chasing peak performance. The only way to know is to test. That brings us to what the research says about why B6 matters—and what it can do when your body actually needs it.
The past decade has completely changed how scientists think about vitamin B6. It’s not just a boring cofactor in your metabolism. New research shows that B6 acts as a kind of metabolic switch—turning on vital pathways for muscle repair, blood sugar control, and even immune regulation, but only when your body is under stress or inflammation.
For athletes or anyone who exercises regularly, B6 is now recognized as an 'exercise mimetic.' That means it can activate some of the same muscle-preserving and anti-catabolic pathways that you get from physical activity. In inflamed adults with low PLP, supplementing with B6 has been shown to improve muscle function and even lower the risk of age-related muscle loss, or sarcopenia. A 2023 trial in Japan found that older adults with high CRP and low PLP who took twenty-five milligrams of B6 daily for eight weeks improved their grip strength and recovery times by nearly twenty percent compared to those who didn’t supplement.
The benefits go beyond muscle. B6 deficiency disrupts your ability to regulate blood sugar and cholesterol. In several clinical studies, people with both low PLP and elevated CRP who received B6 supplements cut their fasting blood sugar by up to twenty percent and raised their HDL—the good cholesterol—by between four and fourteen percent. The reason? B6 is needed for enzymes that process glucose and fat. If you’re deficient, your metabolic machinery slows down, making it harder to burn fuel efficiently or keep your cholesterol in check.
B6 also plays a role in antioxidant defense. When inflammation is high, your cells produce more free radicals. B6 helps regenerate glutathione, your body’s main antioxidant. If your B6 is depleted, you lose this protection, which can accelerate aging at the cellular level.
But—and this is key—these benefits are only seen in people who are actually low on PLP and inflamed. If you’re healthy, topping up with extra B6 doesn’t make you stronger, faster, or more resilient. It’s all about matching supplementation to your personal biology. So how do you do that? The answer is a targeted, evidence-based protocol.
Let’s get practical. If you’re serious about using vitamin B6 as a tool for your athletic, immune, or metabolic health, you need a plan that’s guided by your own lab results—not just supplement marketing.
Step one is testing. Ask your doctor for a blood test that measures both PLP and high-sensitivity CRP. Many standard panels skip these, but they’re easy to order and provide the data you need. If your PLP is below thirty nanomoles per liter and your CRP is above one milligram per liter, you’re a candidate for B6 supplementation. If your PLP is normal and your CRP is low, there’s no evidence you’ll benefit from more B6.
If you do need it, the best-studied form is pyridoxine hydrochloride, or pyridoxine HCl. The effective dose is twenty-five to fifty milligrams per day, taken with food, for eight weeks. This dosing matches what’s been used in clinical trials and is well below the level where side effects start to appear. Higher doses do not work better and can actually cause nerve problems if taken for long periods.
After eight weeks, retest your PLP and CRP. If your PLP has risen above thirty nanomoles per liter and your CRP has dropped, you can either stop supplementation or reduce your dose to a basic maintenance level, such as the amount found in a standard multivitamin. If your PLP is still low or your CRP remains elevated, talk to your doctor about what else might be driving inflammation—things like chronic infections, obesity, or certain medications can all play a role.
One important detail: birth control pills and some anti-seizure medications can deplete B6 more rapidly. If you take these, you may need more frequent monitoring. The bottom line is that your bloodwork—not the supplement label—should always guide your choices. That’s how you avoid both deficiency and unnecessary spending. But supplements aren’t the whole story. Your lifestyle matters just as much.
Supplements are only one piece of the puzzle. Your daily habits can either drain your B6 reserves or help you hold onto them. Let’s break down the three main levers: what you eat, how you move, and how you recover.
First, your diet. B6 is found naturally in foods like poultry, fish, potatoes, chickpeas, bananas, and fortified cereals. But inflammation, not just diet, drives deficiency. If you eat a varied, whole-foods diet and your inflammation markers are low, you’re probably getting enough B6 from food. But if you’re vegan, have a restrictive diet, or are recovering from illness, you could be at higher risk for low PLP.
Next, exercise. Physical activity is a double-edged sword for B6. Regular movement helps lower inflammation, which preserves your B6 stores and keeps your metabolism humming. But intense, prolonged training can temporarily increase B6 needs, especially if you’re not recovering well. That’s why athletes often have lower PLP and higher CRP after big competitions or heavy training blocks. If you’re training hard, make sure you’re supporting recovery with adequate sleep and nutrition.
Sleep is the third lever. Chronic sleep deprivation raises inflammation and can deplete B6 faster. Aim for seven to nine hours per night and manage stress with tools like mindfulness or gentle movement—both have been shown to lower CRP and protect your B6 status.
And don’t overlook alcohol. Regular heavy drinking depletes B6 and raises inflammation, making deficiency more likely. If you drink, keep it moderate, and adjust your diet or supplements accordingly.
By tuning these lifestyle levers, you can often improve your B6 status without reaching for a pill. But if your bloodwork shows you’re still low, that’s when targeted supplementation makes sense. So how will you know if things are going off track?
Most people never realize they’re low on vitamin B6 until problems show up. The early signs are often subtle but meaningful. You might notice more frequent muscle cramps, poor workout recovery, or tingling in your hands and feet. Some people experience unexplained fatigue, mood swings, or even mild depression. If you have trouble managing blood sugar—like feeling shaky between meals or crashing after carbs—low B6 could be a factor, especially if your inflammation is up.
On the immunity front, you might get sick more often, or take longer to recover from colds and minor infections. That’s because B6 is needed for your body to make white blood cells and antibodies. When levels are low, your immune system can’t reset or balance itself as easily, making you more vulnerable to everyday bugs.
There are also red flags that mean you should act right away. If you notice persistent numbness, burning, or weakness in your hands or feet, see your doctor and get your B6 and CRP checked. These can be signs of severe deficiency or, less commonly, B6 toxicity from over-supplementation. If you have known risk factors—like chronic kidney disease, autoimmune disorders, or are on medications that deplete B6—you should be extra vigilant about monitoring your levels.
Finally, if your bloodwork shows a low PLP or a high CRP, don’t ignore it. These markers often change before symptoms appear, giving you a valuable early warning system. Addressing low B6 early can help you avoid bigger problems down the road, from muscle loss to metabolic issues. So what’s the real takeaway for your health strategy?
Here’s the truth that most supplement companies won’t tell you: vitamin B6 is only powerful when your body actually needs it. If your inflammation is high and your PLP is low, B6 can move the needle for your metabolism, muscle function, and immune health. But if your levels are already optimal, extra B6 won’t give you superpowers—it just becomes expensive urine.
The pathway is clear. Test your PLP and CRP before you supplement. Use a targeted dose—twenty-five to fifty milligrams daily for eight weeks—if you’re in the at-risk group. Retest to confirm your levels are up and your inflammation is under control. Support your B6 status with a balanced diet, regular exercise, good sleep, and stress management. Watch for early warning signs, and don’t wait for symptoms to appear before checking your numbers.
This approach puts you in the driver’s seat. You’re using science, not guesswork, to dial in your nutrition and protect your long-term health. When you make your bloodwork the boss, you stop wasting money and start getting results you can actually feel. So the next time you reach for that vitamin, remember: it’s not what’s on the label that counts—it’s what’s happening inside your body.
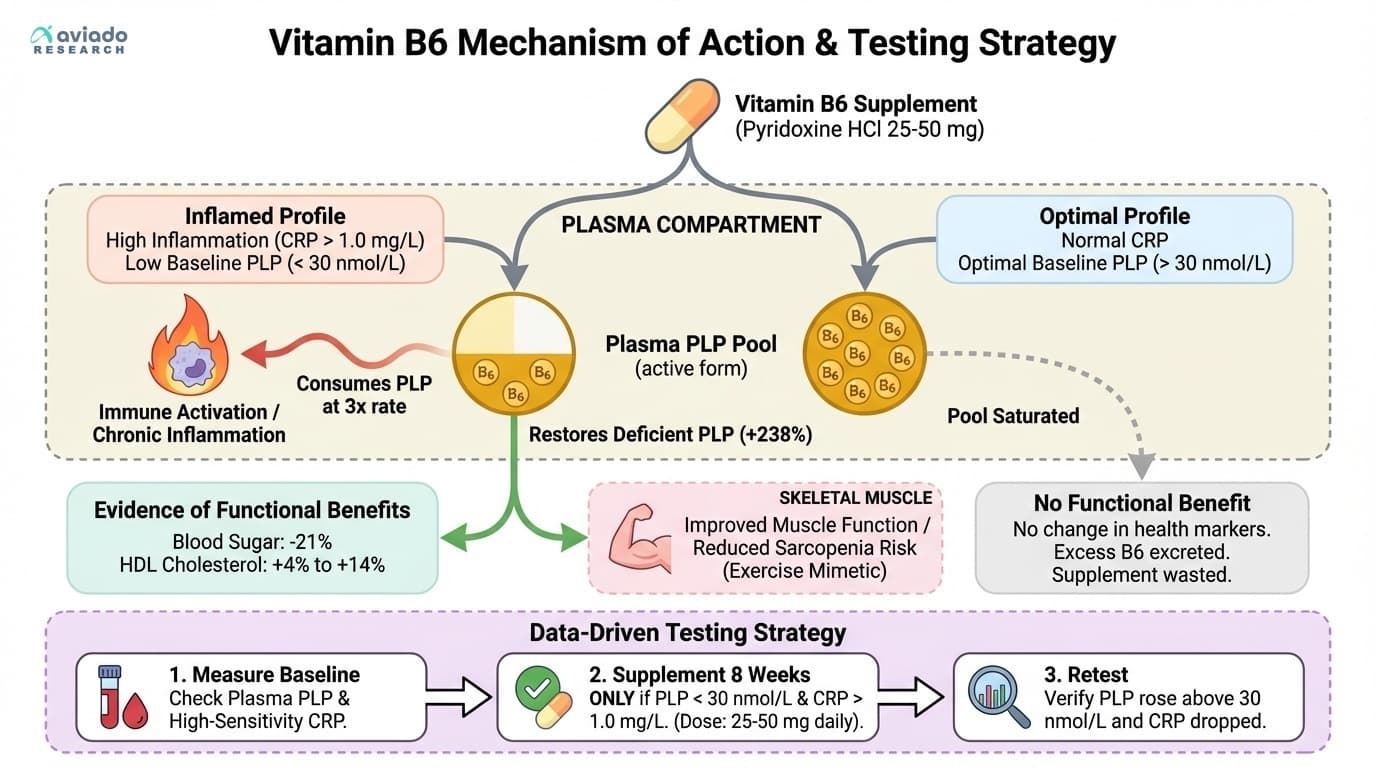
Your Inflammation Level Determines Whether Vitamin B6 Works — And Most People Never Check It
Why plasma PLP and inflammation markers are the hidden keys to vitamin B6 effectiveness
Diagram glossary
- B6:
- A vitamin whose active form, PLP, is rapidly depleted by bodily inflammation.
- CRP:
- An inflammation marker in the blood that helps determine vitamin B6 supplement efficacy.
- HDL:
- High-density lipoprotein, a beneficial cholesterol that transports other cholesterol to the liver.
- PLP:
- Pyridoxal 5'-phosphate, the active form of vitamin B6 consumed rapidly during immune activation.
- pyridoxine:
- A common supplement form of vitamin B6 used to raise blood PLP levels.
Conclusions
Vitamin B6 is not a universal supplement—it's a targeted intervention for people with inflammation-driven deficiency. The key is testing your PLP and CRP levels before supplementing. Only those with low PLP and high inflammation see meaningful benefits from 25-50 mg daily. For everyone else, B6 supplementation is unnecessary. Make your bloodwork the decision-maker, not marketing claims or guesswork.
Most of the evidence for vitamin B6’s benefits comes from populations with baseline deficiency or high inflammation, so results may not generalize to healthy, low-inflammation individuals. Not all studies use the same B6 form or dose, and PLP testing isn’t widely available in standard labs. Some long-term outcomes (like prevention of chronic disease) are still unclear, and Mendelian randomization data suggests B6 may not have strong effects in people who are already replete. Always check for potential interactions with medications and avoid excessive dosing.
Track this in your stack
See how vitamin b6 relates to your health goals and monitor changes in your biomarkers over time.
Sources (7)
This article informs how supplementation moves 1 marker.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
