Your Testosterone Number Is Lying to You: Why Free vs. Total T Is the Difference Between Optimized and Overlooked
The binding protein SHBG—not testosterone itself—may determine whether you respond to therapy or training
You might be told your testosterone level is 'normal,' yet still feel off — tired, unmotivated, or not quite yourself.
That number on your lab report often hides what is really happening inside your body. Understanding the difference between free and total testosterone, and what controls them, can be the key to unlocking better energy, muscle, and mood.
- SHBG (Sex Hormone-Binding Globulin)
- A blood protein that tightly binds testosterone. Higher SHBG usually means lower free T.
- Albumin-Bound Testosterone
- Testosterone loosely attached to albumin. It can break free and be used.
- Sex Hormone Binding Globulin
- SHBG, a protein that binds and inactivates sex hormones. high levels reduce free testosterone, low levels increase it.
- Total Testosterone
- Total testosterone, the primary male sex hormone influencing muscle, bone, and libido. low levels cause fatigue, low libido, and muscle loss.
- Hematocrit
- The percentage of blood volume occupied by red blood cells. low hematocrit indicates anemia, while high values may signal dehydration or polycythemia.
- Free Testosterone
- Bioavailable testosterone not bound to sex hormone binding globulin.
- Hemoglobin
- The oxygen-carrying protein in red blood cells. low hemoglobin causes fatigue and indicates anemia, while elevated levels may increase blood viscosity.
- adipose
- Body tissue specialized in storing energy as fat.
- androgen
- A type of hormone, such as testosterone, that controls male physical characteristics.
- aromatase
- An enzyme responsible for converting androgens like testosterone into estrogens.
Picture this: You drag yourself out of bed after a full night’s sleep, but you still feel foggy. You get through your day, but it takes more effort than it used to. Maybe you’ve noticed your workouts aren’t as effective, or your motivation and drive just seem to be missing. You finally go to your doctor, get blood work, and hear the words, 'Your testosterone is in the normal range.'
But deep down, you know something isn’t adding up. It’s a common experience — you’re told you’re healthy based on one number, but your body tells a different story. That disconnect is not just in your head. The standard lab tests most people get only tell you part of the story. They miss critical pieces that can make the difference between thriving and just getting by.
It turns out, your testosterone number might be lying to you. And understanding why — and what you can do about it — is the key to feeling your best, no matter your age or gender. Let’s unpack what’s really going on.
Testosterone is not just about muscle or libido. It acts as a master regulator for energy, mood, focus, and even how your cells use fuel. Both men and women make and rely on testosterone, though the amounts and the way it’s used can differ.
Here’s what happens in your body: Testosterone circulates in your blood in different forms. Most of it is bound to a protein called sex hormone-binding globulin, or SHBG. Some is loosely attached to albumin, another protein. Only a tiny amount — usually about one to three percent — floats free and unbound. This free testosterone is what can actually enter your cells and trigger the effects you feel: better energy, motivation, body composition, and sexual health.
But there’s a twist. Your body’s ability to use testosterone depends on much more than just how much you make. SHBG can act like a molecular sponge, soaking up testosterone and making it unavailable. If your SHBG is high, you might have plenty of total testosterone, but not enough free testosterone to feel your best. If it’s low, your total testosterone could look borderline, but you might still have enough free T for good health.
For women, these dynamics are even more critical. As you approach perimenopause or menopause, your testosterone and estrogen both decline, but SHBG can fluctuate with birth control, thyroid changes, or shifts in weight. That means symptoms of low testosterone — fatigue, brain fog, low libido — can show up even when your lab report says you’re normal. For men, the same principle applies, especially as you age or if you carry extra weight.
In short, the number most doctors focus on isn’t the whole story. Understanding the balance between total testosterone, SHBG, and free testosterone is what really determines how you feel day to day. That brings us to how you can measure what really matters.
If you want to know where you really stand, you need to look beyond the standard total testosterone test. Here’s what you should ask for, and why each number matters for your health and performance.
First, total testosterone. This is the sum of all testosterone in your blood, including what is bound and what is free. Most labs consider three hundred to nine hundred nanograms per deciliter normal for adult men, and fifteen to seventy for women, though these ranges vary by age and lab. But total testosterone by itself is not enough.
Second, SHBG — sex hormone-binding globulin. SHBG acts as a gatekeeper. High SHBG means more testosterone is locked away and can’t reach your cells. Low SHBG means more free testosterone is available, but it can also signal metabolic issues like insulin resistance. For men, SHBG should be between twenty and sixty nanomoles per liter. For women, it’s typically higher, but context matters — oral contraceptives, thyroid conditions, or liver issues can all push SHBG up or down.
Third, free testosterone. This is the portion that actually matters for how you feel. Direct lab tests for free testosterone can be inaccurate, so the most reliable method is to calculate free testosterone using your total testosterone, SHBG, and albumin levels. For men, optimal free testosterone is usually above ten nanograms per deciliter. For women, it’s above one and a half picograms per milliliter, but symptoms matter more than the exact number.
Here’s why this matters: You could have a total testosterone of five hundred, but if your SHBG is sixty, your free T might be low and you could feel tired, weak, or unmotivated. Flip that around — if your SHBG is twenty, your total testosterone might look borderline low, but your free T could be just right for you.
You should test in the morning, between seven and ten AM, when testosterone is at its peak. If you’re making changes — whether that’s exercise, supplements, or medical therapy — retest every eight to twelve weeks.
If you are on testosterone replacement therapy, monitor your red blood cell count, especially hematocrit, every twelve weeks for the first year. High hematocrit can raise your risk of clots. These are the numbers that move the needle for your energy, performance, and well-being.
So what does the science say about what actually changes these numbers for the better? Let’s look at what works.
When it comes to optimizing testosterone, there’s no magic bullet. But there are interventions with real science behind them. The right approach depends on your starting point — and it always begins with understanding the biology.
If your SHBG is high, less testosterone is available to your cells. Some supplements can help. For example, boron at six to ten milligrams per day has been shown to lower SHBG by up to twenty percent, freeing up more testosterone. The mechanism? Boron influences the liver’s SHBG production and helps modulate steroid metabolism. A small clinical trial found that after one week of boron supplementation, men’s free testosterone rose by almost thirty percent, and estradiol dropped by nearly forty percent. That means more usable testosterone, less conversion to estrogen, and better symptom control — especially for those who feel sluggish or struggle with body composition.
Zinc is another key player. Twenty-five to fifty milligrams daily can support testosterone synthesis, especially if you’re deficient. Zinc is needed for the enzymes that make testosterone in your testes or ovaries. Deficiency is common in athletes, those who sweat a lot, and anyone with a restrictive diet. One study showed that six months of zinc supplementation nearly doubled testosterone in men with low baseline levels.
Vitamin D is also critical. Your body needs it to make hormones, and low vitamin D is linked to lower testosterone in both men and women. Aim for at least two thousand international units daily, especially in the winter or if you get little sun. Vitamin D works by supporting the pituitary gland, which sends out the signals to boost your testosterone production.
If you’re considering herbal approaches, tongkat ali — sometimes called Eurycoma longifolia — at two hundred to four hundred milligrams per day has shown promise in raising free testosterone. The mechanism involves reducing SHBG binding and lowering stress hormones, which can suppress natural testosterone. In one twelve-week trial, men taking tongkat ali saw significant gains in free testosterone, muscle strength, and mood.
For women, adaptogenic herbs like ashwagandha can be helpful for balancing stress hormones that can suppress sex hormone production, especially in perimenopause. Two hundred to six hundred milligrams daily, standardized to withanolides, is a common dose.
No supplement replaces a healthy lifestyle, but targeted use can move your numbers and your symptoms in the right direction. Always retest after eight to twelve weeks, as the benefits accumulate with time and consistency.
But supplements are just one part of the equation. Let’s talk about the lifestyle levers that make the biggest difference.
Supplements help, but lifestyle is the foundation for healthy testosterone and SHBG balance at any age or gender. Here’s what works, and why.
Exercise, especially resistance training, is one of the most powerful ways to improve your testosterone profile. Lifting weights three to four times per week — using big, compound lifts like squats, deadlifts, or push-ups — can raise your testosterone by up to forty percent for twenty-four hours after a session. Over time, regular strength training also lowers SHBG, making more free testosterone available. The mechanism is twofold: muscle contraction sends signals to your brain to ramp up testosterone production, and improved insulin sensitivity from exercise lowers SHBG via the liver. Both men and women see these benefits, though the degree can vary.
Nutrition matters just as much. Your body needs enough healthy fats, protein, and micronutrients to make hormones. Diets too low in fat or protein can suppress testosterone. Aim for twenty to thirty percent of your calories from healthy fats — such as olive oil, avocados, nuts, and fatty fish. Protein should be at least one gram per kilogram of body weight daily.
Carrying excess body fat, especially around the belly, can lower testosterone and raise estrogen. That’s because fat tissue contains aromatase, an enzyme that turns testosterone into estrogen. Losing even five to ten percent of your body weight can lower aromatase activity and restore a healthier testosterone-to-estrogen ratio. This is critical for both men and women, especially during hormonal transitions like menopause.
Sleep is another pillar. Testosterone is released in pulses during deep sleep, especially in the early morning hours. Adults who sleep less than six hours per night have consistently lower testosterone than those who get seven to eight hours. Prioritize sleep hygiene — keep your room dark and cool, avoid screens before bed, and aim for a consistent schedule. Better sleep means higher testosterone, lower SHBG, and more energy to tackle your day.
Finally, manage stress. Chronic stress raises cortisol, which suppresses your body’s own testosterone production and can increase SHBG. Mindfulness, meditation, and even short walks outdoors can help bring stress hormones back into balance.
All these levers work together. Improving just one area can help, but stacking them creates a multiplier effect. Next, let’s talk about what to watch for if things start to go off track.
Hormonal changes rarely happen overnight. They tend to creep up, and many people miss the early warning signs until symptoms become disruptive. Knowing what to look for can help you act early and avoid years of feeling subpar.
For both men and women, the most common early sign is a change in energy and motivation. You might notice more fatigue, a drop in exercise performance, or a loss of interest in things you used to enjoy. Other red flags include brain fog, irritability, lower mood, or trouble concentrating. For men, loss of morning erections or decreased libido is a key early marker that testosterone is dropping. For women, low libido, vaginal dryness, or changes in menstrual cycles can indicate shifting hormone levels.
Physical clues show up too. Increased abdominal fat, difficulty building or maintaining muscle, and slower recovery from exercise or injury can all be signs of low free testosterone or high SHBG. If you notice new or worsening symptoms alongside a lab report that says you’re 'normal,' push for a deeper evaluation.
One critical warning sign to never ignore is a rapid rise in red blood cell count or hematocrit if you’re on testosterone replacement therapy. Elevated hematocrit can increase the risk of blood clots or stroke, so routine checks are non-negotiable.
Another key pattern is the combination of low total testosterone and low SHBG, often seen in people with obesity or insulin resistance. This can indicate a functional, not structural, hormone problem that may respond to lifestyle change rather than lifelong medication.
On the flip side, high SHBG with low free testosterone and normal total testosterone is a red flag for possible thyroid issues, use of oral estrogens, or even liver problems. Each pattern tells a different story and points to specific interventions.
The bottom line: Symptoms matter more than the reference range. If your life feels flat, your motivation is gone, or your body is changing in ways that do not make sense, it’s time to check free testosterone, SHBG, and look for the pattern — not just the absolute numbers. That brings us to the big picture, and how you can take control starting today.
Your testosterone number is only the beginning. If you stop at the total testosterone on your lab report, you risk missing the real drivers of how you feel and perform. Free testosterone, SHBG, and how your body handles each are what determine your energy, mood, and resilience.
The science shows you can influence these markers through a combination of lifestyle, targeted supplementation, and, when needed, medical therapy. Exercise, sleep, nutrition, and stress management all shift your hormone balance in powerful ways. Supplements like boron, zinc, and vitamin D can help move your numbers — but only if you’re addressing the root causes as well.
Most importantly, remember that symptoms matter. If you feel off, tired, or not yourself, dig deeper. Ask for comprehensive labs: total testosterone, SHBG, free testosterone (calculated), and estradiol if you have symptoms of hormonal imbalance. If you start a new intervention, retest after eight to twelve weeks. And if you’re on testosterone therapy, monitor your blood count to stay safe.
You have more control than you think. Understanding your own numbers, knowing what they mean, and making informed changes is the path to moving from just okay to truly optimized. Your journey to better energy, performance, and health starts with asking the right questions — and refusing to settle for 'normal' when you know you can do better.
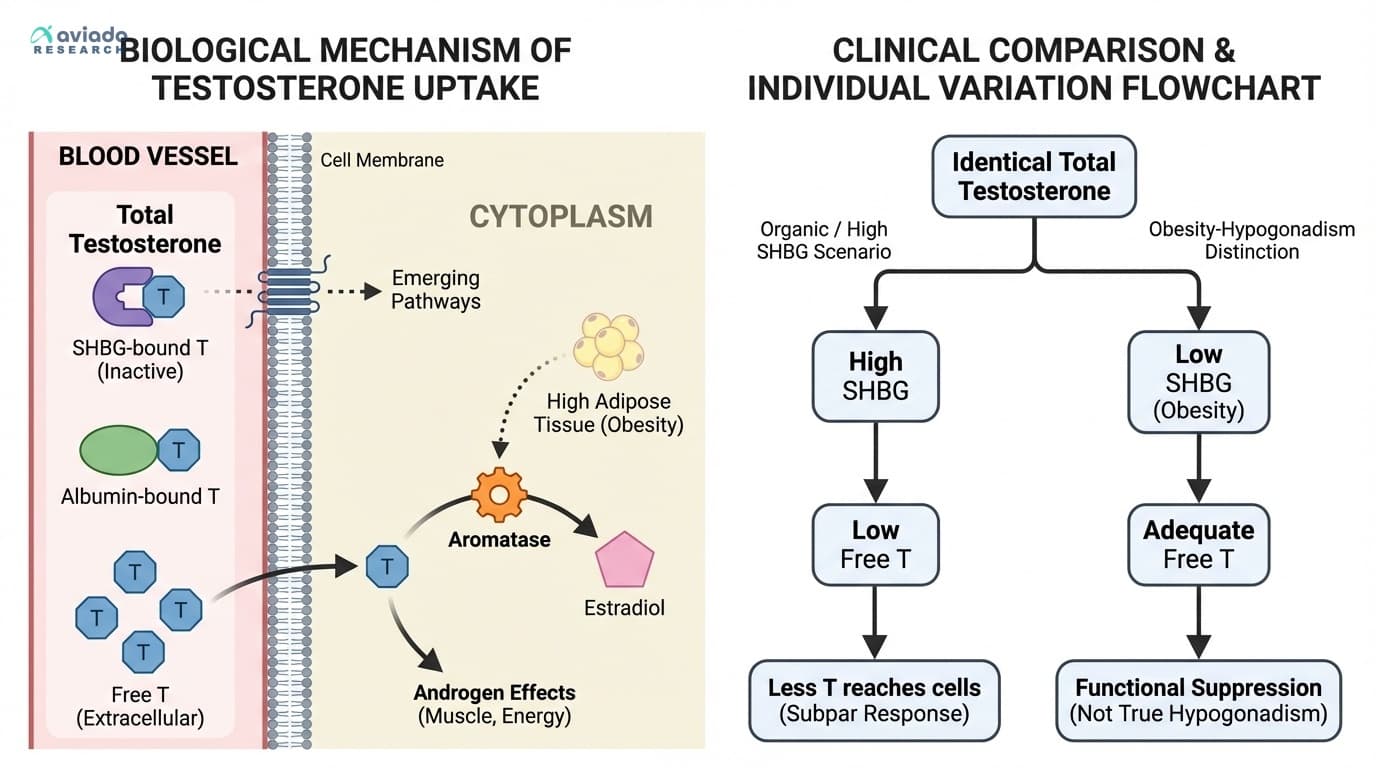
Your Testosterone Number Is Lying to You: Why Free vs. Total T Is the Difference Between Optimized and Overlooked
The binding protein SHBG—not testosterone itself—may determine whether you respond to therapy or training
Diagram glossary
- adipose:
- Body tissue specialized in storing energy as fat.
- androgen:
- A type of hormone, such as testosterone, that controls male physical characteristics.
- aromatase:
- An enzyme responsible for converting androgens like testosterone into estrogens.
- insulin:
- A hormone produced by the pancreas that regulates blood glucose levels.
- SHBG:
- A protein that binds sex hormones in the blood, regulating their biological availability.
- TRT:
- Testosterone replacement therapy is a medical treatment to restore healthy testosterone levels.
Conclusions
Total testosterone is only one clue. SHBG can hide what your tissues can use. Free and bioavailable testosterone better match real effects. If you have obesity, low total T may reflect low SHBG, not testis failure. If you use TRT, your delivery method and blood counts matter for safety. Test smart, then act on the full pattern.
Free testosterone testing is not perfect. Different lab methods can give different results. Many studies do not measure SHBG, so cause and effect stays unclear. Lipid and heart-risk data also vary by dose, route, and study quality. Obesity-related low testosterone has no single agreed cutoff, so doctors must use the full clinical picture.
Track this in your stack
See how testosterone relates to your health goals and monitor changes in your biomarkers over time.
