Your Vitamin A Supplement Could Be Silently Elevating TSH and Triglycerides — Or Doing Nothing At All
Why Personalized Testing Matters More Than You Think for This Widely Overlooked Nutrient
You might reach for a multivitamin or a vitamin A supplement thinking you’re doing something good for your health.
But here’s the twist: the same dose can boost your energy or silently tip your thyroid and heart into the danger zone, depending on your unique biology. Before you swallow another capsule, it’s time to get personal with your vitamin A story.
- Beta-carotene
- Plant-based vitamin A precursor that the body converts to active retinol. Safer than preformed retinol because conversion is self-regulated.
- Triglycerides
- Triglycerides, the primary fat storage molecule in blood. elevated levels indicate metabolic dysfunction and increase cardiovascular risk.
- TSH
- Thyroid-stimulating hormone, the primary thyroid function screening test. elevated TSH indicates hypothyroidism, low values suggest hyperthyroidism.
- Serum Retinol
- The main form of vitamin A measured in blood tests, but not reliable for assessing vitamin A status because the body maintains stable levels until stores are dangerously low or high.
- MRDR (Modified Relative Dose Response) Test
- A specialized blood test that provides accurate assessment of vitamin A stores, unlike standard serum retinol tests which miss early deficiency or excess.
- Retinol
- The active, animal-derived form of vitamin A found in supplements. More potent than plant-based beta-carotene for raising vitamin A levels quickly.
- TSH (Thyroid Stimulating Hormone)
- A hormone produced by the pituitary gland that regulates your thyroid. High levels signal thyroid problems and are influenced by vitamin A status.
- MRDR
- A specialized diagnostic test used to accurately assess the body's vitamin A stores.
- triglyceride
- A type of blood fat that can significantly raise heart disease risk when elevated.
Picture this: you’re in the kitchen, starting your morning routine. You open your supplement cabinet, maybe with a sense of hope—today you’ll be a little healthier. You take your vitamin A capsule alongside breakfast, not realizing that what’s inside could be working with you, or against you, and you wouldn’t even feel a thing.
Supplements are supposed to be simple. But vitamin A is not a one-size-fits-all nutrient. For some people, that capsule is a lifeline—restoring energy, brightening skin, and supporting your immune system. For others, it’s a silent saboteur, quietly raising hormone levels and blood fats that put your heart and metabolism at risk. The unsettling part? You can’t sense any of this happening. There’s no early warning. You just trust that more vitamins must mean more health.
This is what makes vitamin A different from so many other supplements. Its benefits and its dangers are both invisible at first. You go about your day with no idea if your body is using the boost or trying to protect itself from overload. The only way to know is to look under the hood and see how your body actually responds. And that brings us to why this matters so much for you.
Vitamin A is one of those nutrients you’ve probably heard about since childhood. Carrots for your eyes, right? But vitamin A does much more than help you see in the dark. It’s a major player in your immune function, skin health, and—most surprisingly for many people—your hormone balance and metabolism.
Here’s the science: vitamin A is stored in your liver and released as your body needs it. If you run low, your thyroid slows down to conserve energy, your skin gets dull, and your immune system weakens. Taking a supplement when you’re truly low can restore all those systems. But if you already have enough vitamin A stored up, extra doses don’t just float away harmlessly. Instead, they start interfering with your thyroid and your blood fat metabolism.
Why does this happen? Vitamin A interacts directly with your thyroid gland and your liver. In deficiency, supplementing helps your thyroid make more active hormone, revving up your metabolism and raising your energy. But in someone with adequate or high vitamin A stores, more of this nutrient can actually signal the thyroid to slow down—raising your TSH, which is your body’s command to make more thyroid hormone. But instead of more hormone, you get a sluggish system.
At the same time, vitamin A influences how your liver processes fats in your blood. Too much vitamin A can ramp up the production of triglycerides, those sticky blood fats that increase your risk of heart disease. This isn’t just a theoretical risk: studies show that in people who have enough vitamin A, supplementing can increase triglyceride levels by over fifty percent, putting you on a path toward higher cardiovascular risk.
So, the real story is that vitamin A acts as a double agent in your body. It can restore balance if you’re low, or tip you quietly into hormone and metabolic trouble if you aren’t. And you won’t know which side you’re on unless you check your status first.
You might be wondering: how can you tell if vitamin A will help or harm you? The answer is in your bloodwork, but with a catch.
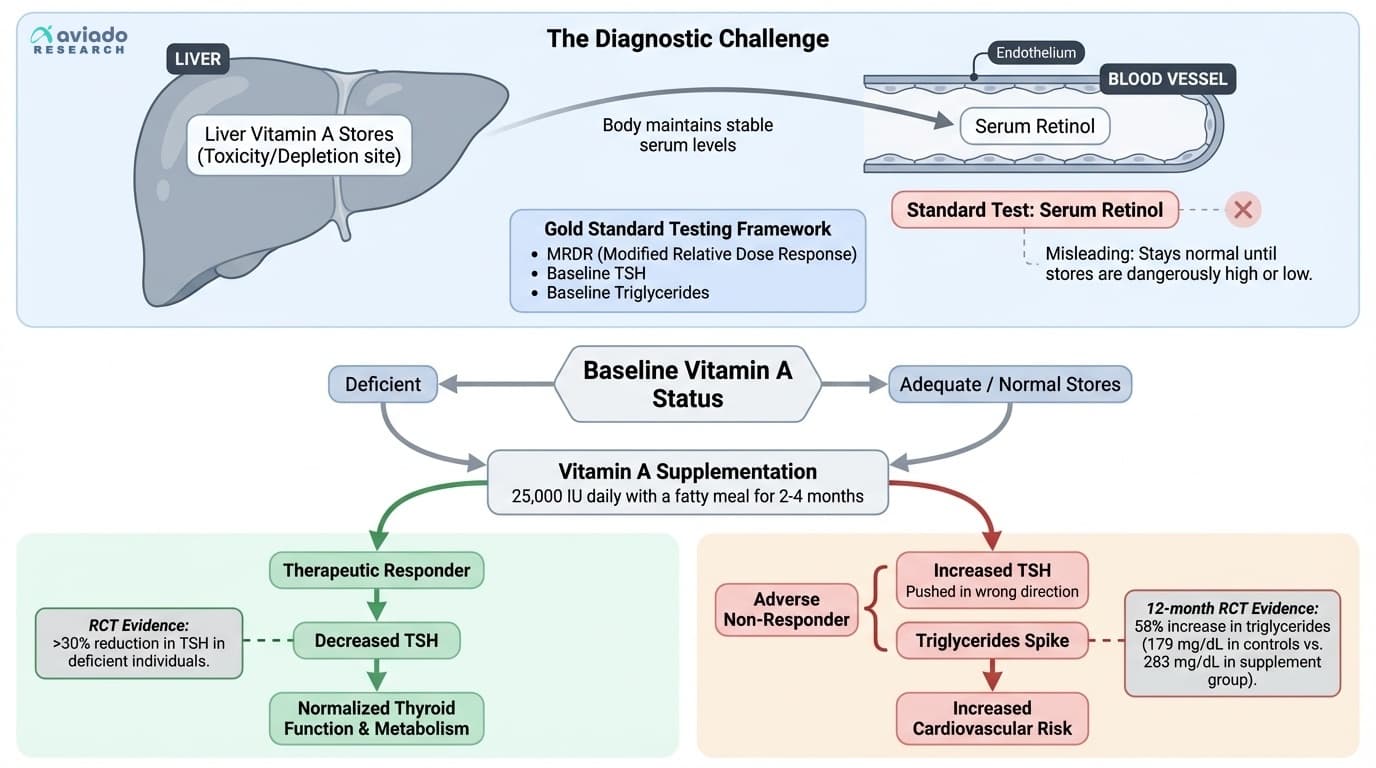
Standard vitamin A blood tests, usually called serum retinol, are not as helpful as you’d hope. Here’s why: your body keeps blood vitamin A levels tightly controlled, even as your liver stores get dangerously low or start to overflow. That means your serum retinol could look normal on a lab report, even if your body is quietly struggling in the background.
Instead, you need a more sensitive test. The best available is called the Modified Relative Dose Response test, or MRDR for short. This test measures how your body responds to a small test dose of vitamin A. If your liver is running low, the test shows a rise in certain vitamin A byproducts, flagging a deficiency before symptoms appear. If your stores are healthy, the test stays flat. Unfortunately, this test is not included in most routine checkups, but some specialty labs and integrative medicine clinics can order it for you.
But there’s more. Because vitamin A impacts your thyroid and your heart, you also want to check your TSH, or thyroid stimulating hormone, and your blood triglycerides. High TSH means your thyroid is under strain, while high triglycerides mean your liver is struggling with fat metabolism. Both can be early signs that vitamin A is tipping your system out of balance.
Here are the numbers you want to know:
- TSH: Ideally between one and two and a half milli-international units per liter, though your optimal range may be a bit lower or higher depending on your age and health status. - Triglycerides: Below one hundred and fifty milligrams per deciliter is considered optimal. The lower, the better for heart health. - MRDR: Should be below zero point zero six. Higher means you’re running low on vitamin A.
Why does this matter? Because if you start supplementing without knowing these numbers, you’re flying blind. You could be helping your body, or you could be stacking up silent risks for your thyroid and heart. That brings us to what you can actually do about it.
If you find out you’re truly low in vitamin A, the science is on your side when it comes to supplementing. Randomized trials have shown that a daily dose of twenty-five thousand international units of vitamin A, taken with a meal containing fat, can restore healthy levels in two to four months. This isn’t a forever dose—it’s a short-term protocol to refill your body’s stores.
Why a fatty meal? Vitamin A is fat-soluble, which means your body absorbs it best when you eat it with oils or fats. Swallowing a capsule on an empty stomach won’t do much. You want to pair it with foods like eggs, avocado, olive oil, or even a full-fat yogurt.
What about the risks? If you’re not deficient, that same dose can flip the script. In a year-long study of almost three hundred adults, those who took high-dose vitamin A saw their triglycerides jump from around one hundred and eighty to over two hundred and eighty milligrams per deciliter—a serious increase that raises your risk of heart disease. Their TSH also climbed by about thirty percent, putting more strain on the thyroid. These effects can show up before you ever feel sick or see symptoms.
The safest protocol is clear: test before you supplement. If your MRDR, TSH, or triglycerides are off, work with a healthcare provider to find out if vitamin A is the cause. If you are low, supplement for two to four months, then retest. If your levels are normal, skip the supplement and focus on getting vitamin A from food sources like sweet potatoes, carrots, leafy greens, eggs, and dairy.
Remember, more is not better—especially with vitamin A. It is stored in your liver for months, so a loading phase is all most people need. After that, maintain with diet, not pills.
Before you ever reach for a supplement, your first question should be: am I getting enough vitamin A from my food?
There are two forms of vitamin A in the diet. The first is preformed vitamin A, or retinol, found in animal foods like liver, eggs, butter, and full-fat dairy. This form is ready for your body to use right away. The second is provitamin A, found in brightly colored fruits and vegetables—think carrots, sweet potatoes, spinach, and kale. Your body has to convert this beta-carotene into usable vitamin A. Some people are rapid converters, others are slow, depending on your genetics.
If you eat a varied diet with plenty of these foods, you’re likely getting enough vitamin A. But certain groups are at higher risk for deficiency. If you avoid animal products, have trouble absorbing fat (like with celiac disease or after weight loss surgery), or have certain genetic differences, you might need more attention to your intake.
Cooking vegetables with a little oil helps your body absorb more beta-carotene. Adding avocado to your salad or sautéing greens in olive oil makes a real difference. For those who do eat animal products, a serving of liver once a week gives you more than enough vitamin A for most people. Eggs and dairy are solid sources too.
A healthy gut is also essential, since vitamin A is absorbed along with dietary fat. If you have ongoing digestive issues—frequent diarrhea, unexplained weight loss, or trouble with fatty foods—talk to your doctor about testing your absorption and vitamin A status.
Physical activity, good sleep, and managing stress all support healthy hormone balance and metabolism, which in turn help your body use vitamin A efficiently. It’s all connected. Remember, supplements are a backup plan, not the main event. Let your food do the heavy lifting wherever possible.
Because vitamin A toxicity and deficiency often develop quietly, it’s easy to miss the early clues. But your body does send signals—you just need to know what to watch for.
If you’re getting too much vitamin A, the first signs are often subtle. You might notice increased fatigue or sluggishness, which comes from your thyroid starting to slow down. Your skin can become dry or start peeling, sometimes with mild hair loss. Headaches, joint pain, and even mild nausea may creep in. Over time, high vitamin A can cause your triglycerides to rise, but you won’t feel that until later—unless you check your bloodwork.
On the flip side, if you’re running low on vitamin A, your immune system might feel weaker. You could get sick more often, or have trouble shaking off colds. Your night vision can decline, and your skin may look dull or rough. In children and pregnant women, vitamin A deficiency is more dangerous, but adults can also suffer from low energy, poor wound healing, and more infections.
The real danger is that both excess and deficiency can sneak up on you. That’s why it’s so important to pay attention if you notice new fatigue, changes in your skin, or unexplained changes in your lab results. If your TSH or triglycerides start drifting up after starting a new supplement, it’s time to pause and check your vitamin A status. And if you’re planning to supplement for immune or metabolic support, get a baseline reading first. Symptoms are your body’s way of asking for a check-in, not a reason to ignore the signs.
Vitamin A is powerful, and so is your biology. The same dose that helps one person can harm another, and there’s no way to know your response without checking your numbers first. Standard blood tests don’t always show the real story until it’s too late, so ask about the MRDR test or work with a healthcare provider who can dig deeper.
If you need a supplement, use it like a prescription: with a clear dose, a set duration, and a plan to retest. If your levels are healthy, trust your diet and your body’s own wisdom. Watch for early signs that something is off, and don’t ignore new fatigue, skin changes, or shifts in your lab results.
Most importantly, remember that nutrition is personal. The future of health is moving away from one-size-fits-all advice and toward precision—tailored to your biology, your genetics, and your lifestyle. Your vitamin A journey should be no different. Take the time to learn your numbers, listen to your body, and make each supplement choice work for you, not against you. That’s how you protect your heart, your hormones, and your metabolism for the long haul.
Your Vitamin A Supplement Could Be Silently Elevating TSH and Triglycerides — Or Doing Nothing At All
Why Personalized Testing Matters More Than You Think for This Widely Overlooked Nutrient
Diagram glossary
- beta-carotene:
- A plant-derived precursor to vitamin A that supports vision, immunity, and overall health.
- MRDR:
- A specialized diagnostic test used to accurately assess the body's vitamin A stores.
- triglyceride:
- A type of blood fat that can significantly raise heart disease risk when elevated.
- TSH:
- A hormone that regulates thyroid function and can be altered by vitamin A supplementation.
Conclusions
Vitamin A is not a "one size fits all" nutrient. Whether it helps or harms depends entirely on your baseline status — and most people have no idea where they stand. The same dose that lowers TSH and improves metabolism in deficient people can spike triglycerides and disrupt thyroid function in others. Testing before supplementing is the only way to make vitamin A work for you, not against you. Personalized dosing based on individual vitamin A status is essential for safely getting the benefits while avoiding hidden cardiovascular and metabolic risks.
Most research on vitamin A's metabolic effects comes from populations with a high risk of deficiency, so results may not apply to well-nourished individuals. Accurate testing (like MRDR) is not widely available, and many clinicians still rely on less reliable serum retinol levels. The impact on neurodegeneration and other long-term risks needs more study. Finally, dosing protocols are based on short- to medium-term trials; the safest duration and maintenance doses for different populations are still uncertain.
Track this in your stack
See how vitamin a relates to your health goals and monitor changes in your biomarkers over time.
