Your Vitamin D Supplement Dose Is Probably Wrong — And Only Your Blood Can Tell You Why
Individual response variation means the same dose can produce 4-fold differences in blood levels between people
You see a bottle of vitamin D on your kitchen counter and wonder if it's actually doing anything for you.
The truth is, your ideal dose is unique, and only your blood can tell you if you’re getting enough — or taking too much. This article unpacks why guessing your vitamin D dose is a gamble, what actually determines your body’s response, and how you can dial in your supplement regimen for real results in immunity, performance, and hormones.
- Vitamin D3 (cholecalciferol)
- The most common supplement form. Most studies use D3, not D2.
- Vitamin D2 (ergocalciferol)
- Another supplement form. It may raise 25(OH)D less than D3 in some people.
- Weight
- Body weight in kilograms, most basic anthropometric measure.
- Fat-soluble absorption
- Vitamin D absorbs better with food that contains fat. Taking it on an empty stomach can lower absorption.
- 25-hydroxyvitamin D (25(OH)D)
- The main blood test for vitamin D status. It reflects your vitamin D stores.
- Vitamin D, 25-OH
- 25-hydroxyvitamin D, the storage form reflecting vitamin D status. Deficiency (<20 ng/mL) extremely common, especially in northern climates.
- Baseline status
- Your starting 25(OH)D level before supplements. It strongly affects how much you benefit and how much your level rises.
- adipose
- Anatomical tissue primarily composed of fat cells used for energy storage and insulation.
- insulin
- A pancreatic hormone that regulates blood glucose levels by facilitating cellular sugar uptake.
- ng/mL
- Nanograms per milliliter, a standard unit of measurement for concentration in fluids.
Picture this: it’s a gray winter morning. You’re pouring your coffee, eyeing that bottle of vitamin D on your counter. Maybe you take whatever dose your friend recommended, or you stick with the label’s suggestion. But deep down, you wonder — is this really working? Does your body even notice?
Almost everyone knows someone who swears by vitamin D. Maybe they say it keeps them energized, or helps their immune system, or lifts their mood. But just as often, you’ll hear someone else say they took vitamin D for months and felt nothing. The reality is, most people have never checked their blood vitamin D. They just assume the dose is right because it’s “standard.”
So if you’re like most people, you’re supplementing blind. You might be getting too little, making no real difference to your health. Or you could be taking more than you need, wasting money or risking side effects. The only way to know is to test your blood. That’s the starting point for real, personalized health decisions. And with vitamin D, the stakes are higher than you think — from your immune strength to your hormone balance, athletic power, and even how you age.
So what makes vitamin D so unpredictable from one person to the next? And how can you know if your daily dose is actually moving the needle for your body? Let’s get into the biology that makes vitamin D unique.
Imagine two people taking the same vitamin D supplement every day. After a few months, one person’s blood level soars, and the other barely budges. It’s not a lab error. It’s biology in action.
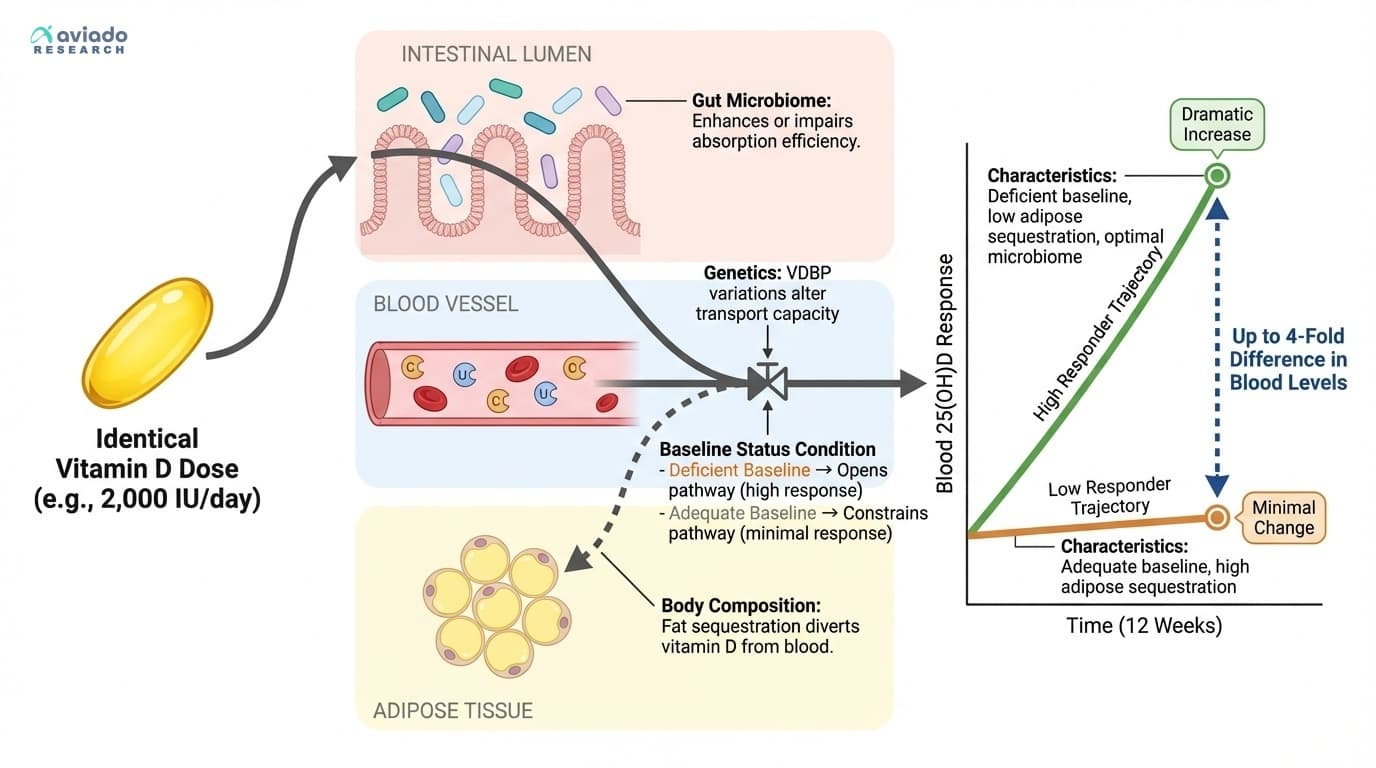
Researchers have seen this over and over: even when they give identical doses, people can have wildly different blood responses — up to a four-fold difference. Some shoot up to the high end of the healthy range. Others hardly move at all, even though they’re swallowing the same pill. Why does this happen?
First, your starting level matters. If you begin with very low vitamin D, your body is primed to soak up more from supplements. People who are already in the healthy range will see a much smaller jump, because their tissues are already saturated. This is the “baseline effect” — the lower you start, the bigger your response. That means if you start out deficient, you’re more likely to see real-life benefits from supplementing than someone who’s already topped up.
Second, body composition makes a huge difference. Vitamin D is fat-soluble. That means it gets stored in your fat tissue. If you have more body fat, more vitamin D will get sequestered away, and less will circulate in your blood. Heavier people often need higher daily doses just to reach the same blood level as someone leaner.
Third, your gut microbiome can influence how much vitamin D you actually absorb. Some gut bacteria help with vitamin D uptake. Others may block it. If your microbiome is out of balance, you might absorb less from your supplement than you expect. Add to that genetic differences in the proteins that transport vitamin D around your body, and you have a perfect recipe for unpredictable results.
The bottom line? Two people can take the same dose, and one could end up with three or four times as much vitamin D in their blood as the other. This is why some people feel a dramatic difference from supplementing, while others feel nothing at all. It’s also why guessing your dose based on someone else’s experience is a losing game.
So how do you know if you’re actually hitting your vitamin D target? That’s where blood testing comes in — and why it’s crucial for anyone who wants results, not just hope.
You might wonder if vitamin D is just a trendy supplement, or if its benefits are really that dramatic. The answer comes down to your starting point. If your blood vitamin D is low, raising it can be a game-changer. But if you’re already in a healthy range, boosting it higher won’t necessarily do anything — and might even have downsides.
Study after study shows the same pattern: people who start with low vitamin D see the biggest improvements in health when they supplement. This holds true for immune function, protection against respiratory infections, and metabolic health, including blood sugar and insulin sensitivity. For example, large trials found that people with blood vitamin D below about fifty nanomoles per liter — that’s twenty nanograms per milliliter — had lower immunity and higher risk of illness. When those people raised their vitamin D, their risk of infections and other issues dropped.
But once your vitamin D is above that threshold, the benefits level off. Taking more doesn’t make your immune system any better. It doesn’t make your muscles stronger or your mood brighter. That’s because vitamin D works like a hormone, not a traditional vitamin. Most of its benefits come from restoring a deficiency, not from pushing your levels ever higher.
Why does this happen biologically? Vitamin D acts as a regulator. When there’s enough in your system, your tissues respond optimally. But when you’re low, everything from calcium absorption to immune cell activation suffers. If you flood your body with more than it needs, your cells start ignoring the signal, or you can disrupt other hormone systems. More is not always better.
So if you’re wondering whether to start vitamin D — or if you should increase your dose — the first step is to know your baseline. That’s the number that tells you if you’re likely to see benefits, or if you’re already in the “sweet spot.” And that brings us to what you can actually measure, and what those numbers really mean for your health.
If you want to know where you stand with vitamin D, only one test matters: the 25-hydroxyvitamin D blood test, usually written as 25(OH)D. This is what your doctor should order, and what almost all scientific research uses to determine deficiency, sufficiency, or excess.
Here’s how to make sense of the numbers:
If your 25(OH)D is below fifty nanomoles per liter — or twenty nanograms per milliliter — you’re officially deficient. Research shows this is where your risk for poor immune function, low bone density, and hormonal imbalances starts to rise. People in this range are the most likely to see real, noticeable benefits from raising their vitamin D.
Levels between fifty and seventy-five nanomoles per liter — or twenty to thirty nanograms per milliliter — are often called “insufficient.” You might not have symptoms, but you’re not fully optimized. Many experts now recommend targeting at least seventy-five nanomoles per liter, or thirty nanograms per milliliter, to support robust immunity, hormonal balance, and muscle function.
The optimal range for most adults is seventy-five to one hundred nanomoles per liter — that’s thirty to forty nanograms per milliliter. This is where studies show the best outcomes for immune health, bone maintenance, and athletic performance, with the lowest risk of deficiency symptoms.
Above one hundred nanomoles per liter — or forty nanograms per milliliter — you’re still in a safe zone for most people, but going higher doesn’t bring extra benefits. If you push much above this for months at a time, especially with high-dose supplements, you risk side effects like high blood calcium, which can cause kidney stones or calcification of blood vessels.
So what does your number really mean for your day-to-day life? If you’re below seventy-five nanomoles per liter, you may notice more frequent illness, slower recovery from exercise, or low energy. You might have trouble building muscle or maintaining strong bones. If you’re in the optimal zone, you’re giving your body what it needs for immune defense and hormonal stability. That’s the range you’ll want to target — and maintain — with the right supplement and lifestyle plan.
But here’s the crucial point: you cannot predict your number just by guessing. Your weight, diet, and sun exposure all play a role, but only your blood test gives you the answer. And once you know your number, you can adjust your dose intelligently. So what’s the best way to do that safely and effectively? Let’s break down the evidence-based protocol next.
Most supplement labels and internet advice would have you believe there’s a one-size-fits-all answer for vitamin D dosing. But the research tells a different story. The right dose for you depends on your size, your baseline blood level, and your body’s unique biology.
For most adults, a good starting dose is one thousand to two thousand international units of vitamin D3 daily if you’re smaller or have lower body weight. If you weigh more, or if you have more body fat, you’ll likely need three thousand to four thousand international units daily to see the same rise in your blood level. A practical rule is about forty to fifty international units per kilogram of body weight. That works out to roughly three thousand international units daily for someone weighing seventy kilograms, or about four thousand to five thousand international units for someone who is closer to one hundred kilograms.
It’s crucial to take your vitamin D with a meal that contains fat. Vitamin D is fat-soluble, which means your body absorbs it much better when it’s paired with dietary fat. Taking it on an empty stomach or with black coffee can cut your absorption dramatically.
Avoid high-dose bolus regimens — like taking fifty thousand international units once a week or once a month — unless your clinician specifically prescribes it for a short-term correction. Research has shown that these big, infrequent doses can disrupt your vitamin D metabolism, create abnormal blood metabolites, and even increase the risk of fractures compared to daily dosing. Your body is built to handle small, steady amounts, just like you’d get from regular sun exposure.
After you start your daily dose, retest your blood after about twelve weeks. This gives your body time to reach a new steady-state. If you’re still below your target — that’s seventy-five to one hundred nanomoles per liter — safely increase your dose by one thousand international units daily and retest again in another twelve weeks. Don’t keep increasing forever without checking your blood, since too much vitamin D can raise your blood calcium and cause harm.
If you need to stay on higher daily doses for months at a time, ask your clinician to check your blood calcium periodically. This is a safety step to make sure you’re not overshooting, since high blood calcium can be a warning of vitamin D excess.
This test-adjust-retest protocol is the only way to know your supplement is actually working. You’ll avoid both underdosing and the risks of taking more than you need. And you’ll give your immune system, muscles, and hormones the support they need — tailored to your body’s real requirements.
Now that you know how to supplement smart, let’s talk about the lifestyle habits that can supercharge your vitamin D — and even reduce your need for supplements.
Supplements are just one piece of the vitamin D puzzle. The way you live — what you eat, how you move, and how much sunlight you get — can all shift your vitamin D level and how your body uses it. If you want to optimize your health, you need to combine smart supplementation with the right lifestyle habits.
Start with sunlight. Your skin makes vitamin D when exposed to UVB rays. Just ten to fifteen minutes of midday sun on your arms and legs, a few times a week, can generate significant vitamin D — especially in the summer or if you live closer to the equator. But if you wear sunscreen, have darker skin, or live in northern latitudes during winter, your skin might make very little. Age also matters. As you get older, your skin becomes less efficient at producing vitamin D from sunlight.
Diet can help, but the reality is, very few foods contain meaningful amounts of vitamin D. Fatty fish like salmon, mackerel, and sardines are among the best sources. A single serving of wild-caught salmon can provide between six hundred and one thousand international units. Egg yolks and fortified dairy or plant milks can add a bit more, but it’s tough to hit your optimal range with food alone unless you eat fish several times a week.
Exercise also plays a supporting role. Weight-bearing activity and resistance training can help your body regulate calcium and vitamin D, supporting stronger bones and better hormone balance. Muscle tissue itself helps process vitamin D, so the more lean mass you maintain, the better your body can utilize what you get from sun, food, or supplements.
Sleep is another hidden factor. Poor or inconsistent sleep can disrupt your hormonal rhythms and immune function, both of which are linked to vitamin D status. Getting at least seven to eight hours of quality sleep per night helps keep your vitamin D metabolism on track.
Gut health matters, too. A diverse, balanced microbiome helps you absorb and process vitamin D more efficiently. Eating a variety of fiber-rich foods, fermented foods like yogurt or kefir, and minimizing unnecessary antibiotics can help cultivate the right gut bacteria.
The takeaway: supplements fill the gap, but you get the best results when you combine them with sun exposure, a nutrient-rich diet, regular exercise, quality sleep, and good gut health. If you optimize these levers, you may need a lower supplement dose — but you should still confirm your blood level to be sure. So how do you know if your vitamin D strategy is working? That’s where early warning signs come in.
You might not notice when your vitamin D starts to slip. Deficiency can be subtle at first, but over time, the signs add up. Knowing what to watch for helps you catch low vitamin D before it turns into a bigger problem.
Frequent illness is one of the most common red flags. If you catch every cold or respiratory infection going around, or you take longer than usual to recover, low vitamin D could be part of the cause. Your immune system relies on vitamin D to activate key defense cells and coordinate the response to viruses and bacteria.
Persistent fatigue and low mood are other warning signs. While many factors can affect your energy and mental health, studies show that people with low vitamin D are more likely to experience tiredness, low motivation, and even depression. Raising low vitamin D can improve mood and energy in people who are deficient.
Muscle weakness, bone pain, or slow recovery after exercise can point to a deficiency, too. Vitamin D is essential for muscle function and helps regulate calcium in your bones. If you notice lingering aches, cramps, or reduced performance, it’s worth checking your level.
For adults, especially as you age, unexplained bone loss or fractures are a late sign of long-term deficiency. If you lose height, develop a stooped posture, or break a bone from a minor fall, get your vitamin D tested as part of your bone health assessment.
Skin and hair changes are less common but can happen. Some people with low vitamin D notice dry skin, hair thinning, or delayed wound healing.
If you’re starting a supplement, watch for warning signs of excess as well. High blood calcium can cause nausea, vomiting, constipation, confusion, or kidney stones. These are rare unless you’re taking very high doses for long periods, but they’re a reason to check both your vitamin D and your calcium if you feel unwell.
The bottom line: listen to your body. If you have any of these signs, or you’re in a high-risk group — limited sun, darker skin, higher weight, older age — a blood test is the fastest way to know where you stand. And once you know, you can take action before bigger issues develop. Which brings us to the final word on getting vitamin D right for your body.
Vitamin D is not a one-size-fits-all supplement. The dose that works for your neighbor, your spouse, or your favorite influencer might do nothing for you — or could even be too much. The science is clear: your starting blood level, body size, absorption, and metabolism all shape your ideal dose and your results.
You unlock the real benefits of vitamin D — for your immune system, muscle strength, hormone balance, and bone health — by getting tested, setting a target, and adjusting your dose based on evidence, not guesswork. Daily, consistent dosing is safer and more effective than mega-doses once a week or month. And stacking the right lifestyle habits can help your supplement go further, while keeping your blood levels in the optimal range.
Vitamin D is one of the most researched and essential nutrients for lifelong health, but only when it’s tailored to you. So the next time you reach for that bottle on your countertop, remember: the most important number is not on the label. It’s in your blood. Test, adjust, and retest — and you’ll know you’re giving your body exactly what it needs, no more and no less.
Ready to get started? Schedule your 25(OH)D blood test, review your results, and use them to set your personalized plan. Your future self — stronger, more resilient, and healthier — will thank you for it.
Your Vitamin D Supplement Dose Is Probably Wrong — And Only Your Blood Can Tell You Why
Individual response variation means the same dose can produce 4-fold differences in blood levels between people
Diagram glossary
- adipose:
- Anatomical tissue primarily composed of fat cells used for energy storage and insulation.
- insulin:
- A pancreatic hormone that regulates blood glucose levels by facilitating cellular sugar uptake.
- ng/mL:
- Nanograms per milliliter, a standard unit of measurement for concentration in fluids.
- vitamin D3:
- A fat-soluble vitamin essential for calcium absorption, bone health, and immune function.
Conclusions
Vitamin D is not a one-dose supplement. Your blood response can vary a lot. Testing turns guessing into a clear plan. Check 25(OH)D, use daily dosing, and retest in 12 weeks. Adjust your dose until you reach 75–100 nmol/L (30–40 ng/mL).
This article simplifies a complex topic. Target 25(OH)D ranges vary by guideline group and by health goal. Many studies measure average effects, not personal dose needs. Evidence on the microbiome and vitamin D binding protein genetics is still early. Some people also have medical reasons to avoid higher vitamin D doses, including sarcoidosis, some kidney disease, and hyperparathyroidism. Dosing and testing should be individualized with a clinician when risk is higher.
Track this in your stack
See how vitamin d3 relates to your health goals and monitor changes in your biomarkers over time.
