Your Heart Health Advantage: A Comprehensive Guide for Men in Their 20s and 30s
Why Early Action Protects Decades of Cardiovascular Health
Here's something surprising: every man over 20 already has heart disease starting in his arteries. Even if you feel perfectly healthy. The choices you make right now decide whether you're active at 50 or recovering from heart surgery.
Your arteries are still flexible in your 20s and 30s. But plaque buildup starts decades before symptoms appear. Men with more risk factors now end up with eight times more artery damage by midlife. The good news: early action can slow or reverse these changes before you feel anything wrong.
Start with omega-3s at 2-4 grams EPA+DHA daily. Add magnesium taurate at 300-400 mg daily for blood pressure. Use citrus bergamot at 500-1000 mg daily for cholesterol support. Include CoQ10 at 100-200 mg daily for heart energy. Combine these with regular cardio and strength training. Every step you take now protects decades of heart health.
- EPA+DHA
- EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid) are the two active omega-3 fatty acids found in fish oil that directly support heart health; the combined daily dose of both is what matters
- Magnesium Taurate
- A specific form of magnesium supplement where magnesium is bonded to taurine (an amino acid), which may improve absorption and offer additional cardiovascular benefits compared to other magnesium forms
- taurate or glycinate
- These are specific forms (formulations) of magnesium where the mineral is bonded to either taurine or glycine amino acids, making it easier for the body to absorb and less likely to cause digestive upset
- ApoB
- ApoB (Apolipoprotein B) is a protein found on the surface of cholesterol particles that carry fat through your bloodstream. High ApoB levels indicate more of these particles are circulating and potent
- Zone 2 Cardio
- Moderate-intensity exercise that improves your heart and fat-burning ability
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- Atherosclerotic Lesions
- Atherosclerotic lesions are areas of damage or buildup inside artery walls, ranging from early fatty streaks to raised plaques made of fat, cholesterol, and other substances. These lesions narrow the
- 120/80
- A standard normal blood pressure reading measured in millimeters of mercury.
- CAC
- Coronary artery calcium, a marker used to measure plaque buildup in heart arteries.
- CRP
- C-reactive protein, a blood marker that indicates inflammation levels in the body.
- DHA
- Docosahexaenoic acid, an omega-3 fatty acid crucial for heart and brain health.
- EPA
- Eicosapentaenoic acid, an omega-3 fatty acid that reduces inflammation and supports heart health.
You might think heart disease is only a problem for older men, but the science says otherwise. In the PAVE study, researchers performed autopsies on young people who died from accidents and found something shocking: every single man over 20 already had visible atherosclerotic lesions in their aorta [1]. These were not just minor changes—some men had fatty streaks, while others had raised lesions. This means the process of artery plaque buildup starts decades before symptoms appear.
If you’re a man in your 20s or 30s, your arteries are still flexible, and your blood vessel lining (the endothelium) is at its peak function. But this peak doesn’t last. From your early 20s onward, the risk factors you collect—like high blood pressure, poor diet, or smoking—start to compound. The Bogalusa Heart Study tracked children into adulthood and found that the more risk factors you had in your 20s, the more plaque you developed as an adult [2]. Men with three or more risk factors had eight times more plaque than men with none.
The takeaway is clear: what you do now sets the stage for your future health. Early plaque buildup is not destiny. Studies show that managing risk factors in young adulthood can slow or even reverse early heart changes. The sooner you start, the more control you have over your heart’s future. Next, let’s look at the unique risks that young men face—and why your timeline is different from women’s.
Men develop heart disease 7-10 years sooner than women. One reason is biology: estrogen helps protect women’s arteries until menopause, but men don’t get that benefit [3]. That means a 30-year-old man’s arteries may be aging as fast as a 40-year-old woman’s.
Another key player is ApoB—a protein found in the cholesterol particles that get stuck in your arteries. The earlier your ApoB levels rise, the sooner plaque starts to build. Lifetime exposure to ApoB is the single biggest driver of heart disease risk. Your clock started ticking when you were a teenager, and every year counts [4].
Blood pressure is also rising faster in young men than ever before. A 2023 analysis found that hypertension in men aged 18-39 jumped from 10.6% to 14.1% over the past decade. This increase is driven by obesity, high salt intake, and chronic stress [5]. Even if you feel healthy, your risk can be silently increasing.
On top of that, the lining of your blood vessels—the endothelium—starts to lose function after your early 20s. It gets harder to keep arteries flexible and prevent dangerous clots. If you’re active, you might think you’re safe, but sudden cardiac events in young athletes have shown that hidden electrical or structural problems can exist without symptoms. That’s why a baseline screening, especially if you have a family history, is smart. Next, let’s break down the most important biomarkers to track—and how to understand your personal risk.
Knowing your numbers is the foundation of heart disease prevention. For men in their 20s and 30s, some markers matter more than others. Here’s what to watch, what’s optimal, and how each one interacts:
- ApoB (Apolipoprotein B): This is the single best predictor of future heart risk. Each ApoB particle can sneak into your artery wall and start plaque formation. The standard range is usually up to 100 mg/dL, but for long-term prevention, aim for less than 80 mg/dL—and ideally under 60 mg/dL if you want to minimize lifetime risk [6]. ApoB is better than standard LDL cholesterol for predicting who will develop heart disease. ApoB rises with a high saturated fat diet, low activity, and excess weight. You can see changes in ApoB within 2-3 months of lifestyle or supplement changes. Lowering ApoB also improves other markers like LDL and triglycerides.
- Lp(a) (Lipoprotein(a)): This marker is mostly genetic. About 1 in 5 men have levels above 50 nmol/L (or 30 mg/dL), which can double or triple risk. Lifestyle changes don’t lower Lp(a), but knowing your number is crucial—it affects how aggressive you need to be with other risk factors. Get it tested once. If it’s high, your prevention plan needs to be stricter.
- hs-CRP (High-Sensitivity C-Reactive Protein): This test measures inflammation in your blood vessels. Even if your cholesterol is perfect, high hs-CRP means higher risk. Optimal is below 0.5 mg/L. You can lower hs-CRP with exercise, weight loss, omega-3s, and magnesium, often within 1-3 months. It interacts with cholesterol—high hs-CRP plus high ApoB is especially risky [7].
- Blood Pressure: Ideal is under 120/80 mmHg. Even “high normal” (120-129 systolic) increases risk by 30-40% over time. Home monitoring is better than single office checks. Lowering sodium, managing stress, and building muscle all help. Blood pressure changes can show within weeks of a new routine.
- Coronary Artery Calcium (CAC) Score: This scan looks for hard plaque in your arteries. A score of zero is highly reassuring if you’re in your 30s. If you have a family history, consider testing at age 35 or sooner.
- Homocysteine: This amino acid, when above 10 umol/L, can damage your artery lining and increase clot risk. Poor B-vitamin status is the main cause. Supplementing with methylated B vitamins can lower levels within a month.
Tracking these biomarkers gives you a clear picture of your risk—and helps you see progress as you take action. Up next, we’ll dig into the most effective supplements and lifestyle tweaks backed by evidence.
If you want one supplement for heart protection, start with omega-3 fatty acids, especially EPA and DHA. The REDUCE-IT trial found that high-dose EPA (2-4 grams per day) led to a 25% reduction in cardiovascular events, even in people with normal cholesterol [8]. That’s a big deal for prevention.
EPA and DHA lower triglycerides, reduce inflammation, and may help improve blood vessel lining. In men aged 18-39, omega-3s can move triglyceride numbers within 4-8 weeks and lower hs-CRP over 2-3 months. The EPA-dominant form is most effective for heart benefits. Look for purified fish oil or algae-based formulas that highlight EPA content.
There is a dose-response effect: benefits increase up to at least 4g per day, but even 2g shows positive changes. Omega-3s work synergistically with exercise and magnesium—together, they further lower blood pressure and inflammation. If you’re vegetarian or vegan, choose algae-based EPA/DHA supplements.
Early warning signs that omega-3s may be especially important for you include high triglycerides, a family history of sudden cardiac events, or elevated hs-CRP. The benefit compounds over time, so the earlier you start, the more protection you gain. Next, we’ll look at natural ways to optimize cholesterol—without jumping to statins.
Citrus bergamot is a polyphenol-rich extract from a Mediterranean citrus fruit. Multiple randomized controlled trials have shown that 500-1000 mg per day of bergamot can reduce LDL cholesterol by 20-30% and improve LDL particle size—a crucial factor for young men who want to optimize cholesterol without medication [9].
Bergamot works by reducing cholesterol synthesis in the liver and improving how your cells clear LDL particles from the blood. The effects usually show up within 4-12 weeks of starting supplementation. It’s particularly useful for men whose LDL or ApoB runs high despite a healthy lifestyle. The active polyphenols in bergamot also have antioxidant effects, which may help further protect the artery lining.
The best form is a standardized extract with at least 38% polyphenols. Research suggests bergamot stacks well with omega-3s, as the two target different pathways—one on cholesterol, the other on inflammation and triglycerides. Young men with a family history of early heart disease, or who want to avoid statins, may find bergamot a valuable add-on. However, if your Lp(a) is elevated, you’ll need to address that separately.
Watch for improvements in LDL-C, ApoB, and sometimes blood sugar. If you have a family history or high baseline cholesterol, check your markers after three months to track your response. Next, we’ll discuss magnesium—why most young men don’t get enough, and how the right form matters.
CoQ10, especially in the ubiquinol form, is essential for generating cellular energy in heart muscle. Men with a family history of heart disease are especially at risk for low CoQ10 levels. Supplementing with 100-200 mg per day of ubiquinol CoQ10 has been shown to improve endothelial function, which helps keep arteries flexible and responsive [5].
CoQ10 acts as an antioxidant inside your mitochondria, protecting them from damage and supporting efficient energy metabolism. Improvements in vascular function can be seen after 8-12 weeks.
CoQ10 works well alongside omega-3s, magnesium, and exercise. Together, these interventions support both the structure and function of your arteries. If you notice fatigue, muscle weakness, or a drop in exercise performance, these may be early signs of low CoQ10.
For men with high-intensity training routines or a family history of heart issues, CoQ10 may give your heart the energy resilience it needs. Next, let's move beyond supplements and address the foundation: movement.
Your heart is one of the most energy-hungry organs in your body. CoQ10, especially in the ubiquinol form, is essential for generating cellular energy in heart muscle. Men with a family history of heart disease, or those taking statins, are especially at risk for low CoQ10 levels. Supplementing with 100-200 mg per day of ubiquinol CoQ10 has been shown to improve endothelial function, which helps keep arteries flexible and responsive [5].
CoQ10 acts as an antioxidant inside your mitochondria, protecting them from damage and supporting efficient energy metabolism. If you’re using statins for cholesterol, your CoQ10 levels can drop by up to 40%, so supplementation is strongly recommended. Improvements in vascular function can be seen after 8-12 weeks.
CoQ10 works well alongside omega-3s, magnesium, and exercise. Together, these interventions support both the structure and function of your arteries. If you notice fatigue, muscle weakness, or a drop in exercise performance, these may be early signs of low CoQ10.
For men with high-intensity training routines or a family history of heart issues, CoQ10 may give your heart the energy resilience it needs. Next, let’s move beyond supplements and address the foundation: movement.
No supplement can replace movement when it comes to heart health. Research consistently shows that young men who combine Zone 2 cardio (moderate, steady effort) with resistance training get the biggest gains in heart protection [11].
The sweet spot is 150+ minutes per week of moderate cardio—think brisk walking, cycling, or swimming—plus 2-3 resistance sessions. Zone 2 cardio improves your body’s ability to burn fat and increases the flexibility of your arteries. Resistance training lowers blood pressure by 5-10 mmHg and reduces arterial stiffness. Together, they also lower hs-CRP and improve insulin sensitivity.
You’ll see changes in blood pressure and resting heart rate in as little as 4 weeks, with continued improvement over months. The effects are additive with supplements: for example, omega-3s and exercise together lower triglycerides more than either alone.
If you’re new to exercise, start with walking and basic strength moves, and build up gradually. Men with a family history of heart disease or those who notice early warning signs—like erectile dysfunction or high resting heart rate—should see exercise as a non-negotiable. Next, let’s discuss early warning signs and when to get extra screening.
Some men have silent risks that need early attention. If your father or brother had a heart attack or stroke before age 55, your risk is 2-4 times higher. This means you should get ApoB, Lp(a), and possibly a coronary artery calcium (CAC) score checked by age 30 [12].
Another warning sign is erectile dysfunction. The arteries in the penis are much smaller than those in the heart, so blood flow problems show up there first—often 3-5 years before a cardiac event. If you experience ED in your 20s or 30s, don’t ignore it. It can be a red flag for early vascular disease, not just a lifestyle issue.
A resting heart rate above 75 beats per minute, despite good sleep and fitness, is another signal that your heart or nervous system needs attention. It may indicate chronic stress, poor fitness, or undiagnosed heart issues.
If you fall into any of these categories, consider more frequent biomarker checks, earlier imaging, and aggressive lifestyle changes. These early warning signs are your chance to act before symptoms appear. In the final section, we’ll pull these actions together into a practical starter protocol.
You now have a roadmap for protecting your heart decades before most men even think about it. Here’s how to put it all together:
- Get your ApoB, Lp(a), hs-CRP, blood pressure, and (if indicated) CAC score checked. Track homocysteine if you have a family history or eat few B vitamins. - Start omega-3 supplementation: 2-4g EPA+DHA per day, with an EPA-dominant formula. Expect to see triglycerides and inflammation improve within 4-8 weeks. - Add citrus bergamot (500-1000 mg/day) if your LDL or ApoB is high or runs in your family. Check for changes in 3 months. - Supplement with magnesium taurate or glycinate (300-400 mg/day), especially if your blood pressure or resting heart rate is high, or you get muscle cramps. - Use CoQ10 (100-200 mg/day, ubiquinol form) if you take statins, have a family history, or want extra mitochondrial support. - Commit to 150+ minutes of Zone 2 cardio and 2-3 resistance training sessions weekly. The combination is more powerful than either alone.
For young men, these interventions are the equivalent of brushing your teeth—a daily investment for decades of protection. Adjust your plan based on biomarker feedback and family history. By acting now, you stack the odds in your favor for a healthy, active life.
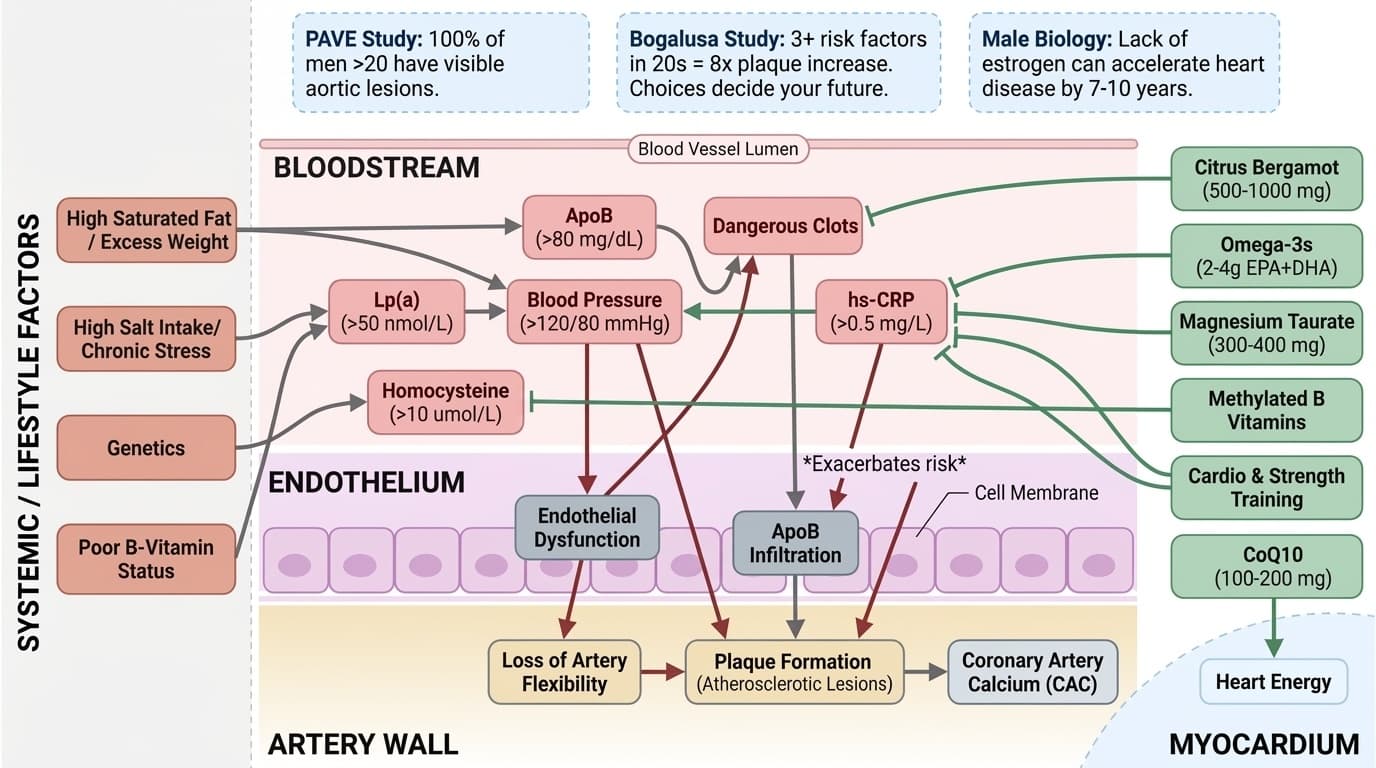
Your Heart Health Advantage: A Comprehensive Guide for Men in Their 20s and 30s
Why Early Action Protects Decades of Cardiovascular Health
Diagram glossary
- 120/80:
- A standard normal blood pressure reading measured in millimeters of mercury.
- CAC:
- Coronary artery calcium, a marker used to measure plaque buildup in heart arteries.
- CRP:
- C-reactive protein, a blood marker that indicates inflammation levels in the body.
- DHA:
- Docosahexaenoic acid, an omega-3 fatty acid crucial for heart and brain health.
- EPA:
- Eicosapentaenoic acid, an omega-3 fatty acid that reduces inflammation and supports heart health.
- Homocysteine:
- An amino acid in the blood that increases cardiovascular risk at high levels.
- LDL:
- Low-density lipoprotein, known as bad cholesterol, which contributes to plaque buildup in arteries.
- PAVE:
- A scientific study referenced for examining early atherosclerotic lesions in young people.
- estrogen:
- A primary sex hormone responsible for regulating the female reproductive system.
- mg:
- Milligram, a metric unit of mass equal to one thousandth of a gram.
- mmHg:
- Millimeters of mercury, a standard unit of measurement used for blood pressure.
Conclusions
Heart disease starts far earlier than most men realize. The evidence is clear: your 20s and 30s are the most powerful years to shape your cardiovascular future. By tracking the right biomarkers, targeting proven supplements like omega-3s, magnesium, citrus bergamot, and CoQ10, and maintaining a consistent exercise routine, you can dramatically lower your risk. Early action doesn’t just delay heart problems—it may prevent them altogether. Make small, consistent changes now for a lifetime of stronger, healthier living.
Most studies referenced focus on middle-aged or higher-risk populations, with fewer long-term trials specifically in men aged 18-39. While the mechanisms and biomarker targets are well-established, individual response may vary based on genetics, lifestyle, and adherence. Some interventions, like citrus bergamot or high-dose omega-3s, may not be suitable for everyone and should be discussed with a healthcare provider. The evidence for Lp(a) management is still emerging, and not all supplements have FDA approval for prevention. As always, use these strategies as part of a comprehensive approach under medical guidance.
Track this in your stack
See how omega 3 relates to your health goals and monitor changes in your biomarkers over time.
Sources (12)
This article informs how supplementation moves 3 markers.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
% EPA + DHA in red-blood-cell membranes. Target >= 8% for cognitive protection; most US adults sit at 4-5%.
High-sensitivity C-reactive protein. > 3 mg/L associated with chronic systemic inflammation affecting the brain and vasculature.
Apolipoprotein B — particle count of atherogenic lipoproteins. Levels > 80 mg/dL associated with cardiovascular event risk independent of LDL-C.
