Cardiovascular Mastery for Men 40–65: Precision Strategies to Outpace Heart Disease
Why Your Next Decade Determines Your Lifelong Vascular Health
Here's a surprising truth: half of all heart attacks in men strike before age 65, often with zero warning signs.
Standard cholesterol tests miss up to 40% of men who will have heart attacks. Your LDL number alone doesn't tell you how many dangerous particles are attacking your arteries right now.
You need better tests and targeted action. Advanced markers like ApoB, Lp(a), and Coronary Artery Calcium scores reveal hidden plaque that basic tests miss. Even subtle changes like declining stamina or erectile dysfunction can signal arterial problems years before a crisis hits.
The fix is precise and proven. Take 2-4 grams of EPA omega-3 daily to cut heart events by 25%. Add 200-300 mg of ubiquinol CoQ10 for heart muscle energy. Use 1200 mg aged garlic extract to slow plaque buildup and drop blood pressure by 5-8 points. Combine with 150-180 minutes of moderate cardio weekly. These steps can dramatically shift your odds and protect your heart, brain, and vitality for decades.
- Ubiquinol
- The active, reduced form of CoQ10 that your body absorbs better than standard CoQ10. Essential for heart muscle energy production and antioxidant protection.
- EPA (Eicosapentaenoic Acid)
- A specific omega-3 fatty acid that at high doses (2-4 grams daily) reduces inflammation, lowers triglycerides, and stabilizes arterial plaque. More cardio-protective than DHA.
- Aged Garlic Extract
- A specific formulation of garlic that has been fermented or aged to concentrate its active sulfur compounds, making them more bioavailable and less harsh than raw garlic. At doses around 1200 mg, rese
- Zone 2 Cardio
- Moderate-intensity exercise where you can still hold a conversation. The optimal intensity for improving arterial health and cardiovascular fitness.
- Apolipoprotein B
- Apolipoprotein B, the protein component of atherogenic particles. Desirable <90 mg/dL (risk-dependent).
- Calcium
- Total serum calcium, essential for bone health, muscle contraction, and nerve signaling. low levels cause muscle cramps and osteoporosis risk, while high values may indicate parathyroid disorders.
- Nitric Oxide
- A naturally produced molecule in the body that signals blood vessel walls to relax and widen, improving blood flow and keeping arteries flexible. Declining levels, often linked to lower testosterone i
- CAC
- A measure of calcium buildup in coronary arteries used to assess heart attack risk.
- EPA
- An omega-3 fatty acid used to reduce cardiovascular events and lower inflammation.
- estrogen
- A steroid hormone that regulates reproductive function and can influence arterial inflammation.
- LDL-C
- The cholesterol found in low-density lipoproteins, commonly known as bad cholesterol.
You might feel healthy, but heart disease often starts decades before the first symptom. For men between 40 and 65, plaque has been building silently since your teens. By midlife, your arteries have seen 25 years or more of exposure to harmful particles—long before a heart attack or stroke ever occurs. The real question is not if you have plaque, but how much and how stable it is.
This process speeds up as testosterone levels decline and visceral fat increases. Lower testosterone reduces your body's ability to produce nitric oxide, which helps keep arteries flexible and clear. At the same time, higher estrogen (from testosterone converting in fat tissue) increases inflammation, making your arterial walls more vulnerable to damage. Blood pressure also rises quietly, often spiking overnight or in stressful situations, even if office readings seem normal. Over time, these factors work together to stiffen arteries and raise your risk of a serious event.
The key insight here is that cardiovascular disease does not show up overnight. The choices you make—and the biomarkers you track—during these decades set the course for your health in later years. Next, we’ll look at why standard cholesterol tests don’t tell you the whole story and which advanced markers can actually reveal your true risk.
For years, your doctor has likely focused on your LDL cholesterol number. But research shows that up to 40% of heart attacks happen in men with 'normal' LDL-C. That’s because LDL-C measures only the mass of cholesterol, not how many dangerous particles are circulating. Two men could have the same LDL-C but very different numbers of atherogenic particles—and very different risks.
ApoB is the key marker here. It counts all the particles that can build plaque in your arteries. Aiming for an ApoB below 80 mg/dL is ideal if you have moderate risk, and below 60 mg/dL if you have a high risk or family history. Unlike LDL alone, ApoB gives you a much clearer picture of what's actually happening inside your arteries.
Lp(a) is another powerful marker. It’s almost entirely set by your genes and stays stable over your life. If your Lp(a) is over 75 nmol/L, your risk for heart events triples, and you’ll need to be much more aggressive with your prevention strategy. Most men only need to check this once—but not knowing your number can leave you with a false sense of security.
These markers interact: someone with high ApoB and high Lp(a) faces the highest risk, even if their standard cholesterol looks normal. The next section will show how the Coronary Artery Calcium score gives you a direct look at actual plaque and why it can reclassify your risk in minutes.
The Coronary Artery Calcium (CAC) score is a simple CT scan that measures calcified plaque in your heart arteries. This test cuts through the guesswork with direct evidence. A zero CAC score at age 50 means your 10-year heart attack risk is under 2%—regardless of cholesterol or family history. A score over 100 puts you in the high-risk category requiring immediate action.
Unlike blood tests that estimate risk, CAC shows actual disease in your arteries. This $75-150 scan can completely reshape your prevention strategy. Get a baseline CAC at age 40-45, then repeat every 5 years if above zero. The result determines how aggressively you need to intervene with supplements and lifestyle changes.
Research shows aged garlic extract can slow CAC progression by 7.5% annually compared to placebo. Rapid CAC increases (>15% per year) signal unstable plaque requiring intensive management. When combined with elevated ApoB or Lp(a), high CAC scores identify men at extremely high risk who benefit most from comprehensive intervention protocols.
Even after you lower cholesterol, hidden inflammation can keep your risk high. The high-sensitivity C-reactive protein (hs-CRP) test measures this silent threat. An hs-CRP below 1.0 mg/L is ideal. Higher levels mean your arteries are more likely to develop unstable plaque—plaque that can rupture and cause a heart attack. If your hs-CRP is elevated, you’ll want to address sources of inflammation, including abdominal fat, poor sleep, and insulin resistance.
The triglyceride/HDL ratio is another key number. You want this ratio below 1.5 for optimal heart health (and below 2.0 is still acceptable). Why does this matter? A high ratio signals a type of cholesterol imbalance that accelerates plaque formation and often reflects insulin resistance. This ratio moves quickly with changes in diet, exercise, or targeted supplements, so you can see improvements in a matter of weeks to months.
These markers interact with ApoB and Lp(a): high inflammation or insulin resistance can make even moderate particle numbers more dangerous. That’s why a comprehensive approach—tracking and lowering all these markers—yields the best results. Next, we’ll cover blood pressure, one of the most modifiable and underappreciated drivers of heart risk.
Blood pressure is the most modifiable risk factor for stroke and heart attack, yet it often gets overlooked. Many men develop 'white coat normal' readings—normal in the doctor’s office but consistently high at home or overnight. The gold standard is a 24-hour ambulatory blood pressure monitor, aiming for a true average below 120/80 mmHg.
Arterial stiffness rises as you age, and even slight increases in blood pressure speed up plaque buildup. High blood pressure interacts with high ApoB and elevated inflammation to create a perfect storm for arterial damage. The timeline for improvement can be as short as a few weeks with the right interventions—diet, exercise, and targeted supplements like aged garlic extract, which research suggests can lower systolic blood pressure by 5-8 mmHg and slow plaque progression.[3]
Keeping your blood pressure in range is especially important if you have other risk factors like high Lp(a) or a positive CAC score. Next, we move from diagnostics to action: evidence-based supplements that move these markers in the right direction.
Targeted supplements work, but dosage and form determine results. Here's what clinical evidence supports for cardiovascular protection:
High-dose EPA omega-3 (2-4 grams daily): The REDUCE-IT trial demonstrated a 25% reduction in cardiovascular events at these doses.[1] EPA-dominant formulations outperform balanced EPA/DHA for heart protection. Triglycerides drop 15-30% within 6-12 weeks, and the triglyceride/HDL ratio improves significantly.
CoQ10 as ubiquinol (200-300 mg daily): Essential for heart muscle energy production. The Q-SYMBIO trial showed 43% fewer cardiovascular deaths in heart failure patients.[2] Ubiquinol absorbs 8 times better than standard CoQ10. Benefits for exercise capacity and fatigue appear within 8-12 weeks.
Citrus bergamot (500-1000 mg daily): Reduces LDL by 20-30% and triglycerides by 15-25% while raising HDL. Works through the same HMG-CoA reductase pathway as pharmaceutical interventions but without muscle side effects. Most effective in men with metabolic syndrome.
Aged garlic extract (1200 mg daily): The LA BioMed trial showed 80% slower coronary calcium progression over 12 months.[3] Additionally reduces systolic blood pressure by 5-8 mmHg. Synergistic effects when combined with omega-3 and exercise.
Stack these based on your biomarker profile: high ApoB responds best to bergamot plus EPA; elevated blood pressure benefits most from aged garlic plus CoQ10.
Exercise is not just about burning calories—it directly affects your arteries, lipids, and blood pressure. The sweet spot is 150–180 minutes per week of sustained, moderate-intensity cardio (Zone 2), where you can still hold a conversation. This level of exercise improves endothelial function, raises HDL, lowers triglycerides, and reduces arterial stiffness.
The dose-response is powerful: moving from sedentary to just 150 minutes a week gives you 80% of the total cardiovascular benefit. Improvements in triglyceride/HDL ratio and blood pressure can be seen in as little as 4–8 weeks. Exercise also enhances the effects of supplements like omega-3s and aged garlic extract.
For men with high CAC or ApoB, exercise is especially effective when combined with targeted supplementation. If you’re experiencing early signs like declining exercise capacity or increased recovery time, it’s a signal to ramp up your cardiovascular workup and activity plan. Next, we’ll explore early warning signs unique to men in this age group and why you should never ignore them.
Your body often gives subtle hints before a serious heart event—but only if you know what to look for. Erectile dysfunction (ED) is a classic early sign: the arteries in the penis are smaller than those in the heart, so ED can appear 3–5 years before a heart attack. If you’ve started using medications like PDE5 inhibitors, it’s time for a full cardiovascular workup, including CAC and advanced lipid testing.
Exercise intolerance is another warning. If activities that were easy in your 40s now leave you winded in your 50s, it’s not just aging. Reduced recovery or stamina strongly predicts risk and should prompt stress testing and deeper biomarker review.
Family history also matters: if your father or brother had a heart attack before age 55, your risk doubles. Combine this with an Lp(a) test and CAC score to pinpoint your true baseline. These demographic-specific red flags mean you can’t rely on population averages—you need a personalized approach. Next, we’ll show how all these pieces fit together into a comprehensive, actionable strategy for men in their 40s through 60s.
Bringing it all together, the most effective approach to heart health at midlife is precision prevention. Standard care—just checking LDL and prescribing a statin—misses too much. Instead, you need to track the markers that actually predict risk: ApoB, Lp(a), CAC, hs-CRP, and the triglyceride/HDL ratio. Each marker responds to specific interventions on its own timeline, and the best results come from stacking strategies.
For example, if your ApoB is high and CAC is above 100, combine high-dose EPA, CoQ10, citrus bergamot, aged garlic extract, and Zone 2 cardio. Recheck your blood pressure and triglyceride/HDL ratio every 3–6 months to track progress. If your Lp(a) is elevated, focus on even more aggressive lipid lowering and consider clinical trials.
The why behind this strategy is simple: you’re not just preventing a heart attack, you’re preserving brain function, sexual health, and exercise capacity—everything that depends on strong circulation. With these tools, you can control your risk and maximize your healthspan for decades. In the final section, we’ll summarize the most important takeaways and set the stage for deeper dives into each intervention.
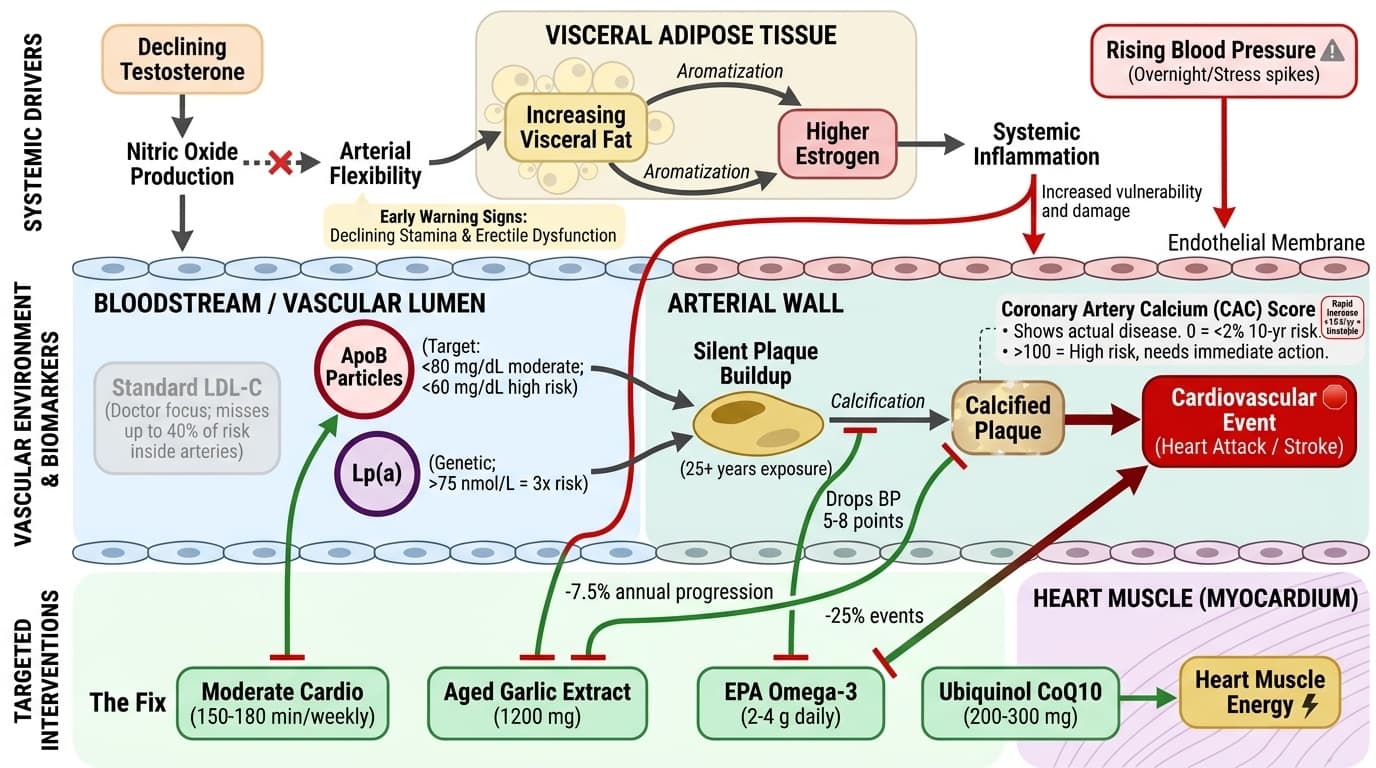
Cardiovascular Mastery for Men 40–65: Precision Strategies to Outpace Heart Disease
Why Your Next Decade Determines Your Lifelong Vascular Health
Diagram glossary
- CAC:
- A measure of calcium buildup in coronary arteries used to assess heart attack risk.
- EPA:
- An omega-3 fatty acid used to reduce cardiovascular events and lower inflammation.
- estrogen:
- A steroid hormone that regulates reproductive function and can influence arterial inflammation.
- LDL-C:
- The cholesterol found in low-density lipoproteins, commonly known as bad cholesterol.
Conclusions
The years between 40 and 65 are the make-or-break decade for your cardiovascular health. Heart disease often strikes without warning, but the right tests and interventions can dramatically shift your odds. Standard cholesterol checks miss too much—advanced markers like ApoB, Lp(a), and the CAC score provide a complete picture. Targeted supplements such as high-dose EPA, CoQ10, citrus bergamot, and aged garlic extract, combined with consistent Zone 2 cardio, can move your numbers in the right direction and help stabilize or even regress plaque. By tracking these markers and acting early, you don’t just lower your risk of heart attack—you protect your vitality, brain, and longevity.
While the evidence for these interventions is strong, most studies focus on high-risk or already-diagnosed patients, and long-term data in healthy men are still emerging. CAC scoring exposes you to low-dose radiation, so discuss frequency with your doctor. Lp(a) remains difficult to modify directly, and not all supplements are regulated equally—choose pharmaceutical-grade products when possible. Always tailor protocols to your unique biomarker profile and medical history, and work with a healthcare provider for personalized risk management.
Track this in your stack
See how omega 3 relates to your health goals and monitor changes in your biomarkers over time.
Sources (3)
This article informs how supplementation moves 3 markers.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
% EPA + DHA in red-blood-cell membranes. Target >= 8% for cognitive protection; most US adults sit at 4-5%.
High-sensitivity C-reactive protein. > 3 mg/L associated with chronic systemic inflammation affecting the brain and vasculature.
Apolipoprotein B — particle count of atherogenic lipoproteins. Levels > 80 mg/dL associated with cardiovascular event risk independent of LDL-C.
