Gut Health in Midlife Men: The Hidden Driver of Your Health After 40
Why Your Microbiome Matters More Than Testosterone, Cholesterol, or Diet
Surprising fact: Your gut bacteria outnumber your own cells and produce 95% of your serotonin.
Most men focus on testosterone or cholesterol after 40. But your 38 trillion gut bacteria control inflammation, hormone balance, and brain chemistry. Common medications like heartburn drugs quietly destroy gut diversity by 20%.
This means digestive issues, brain fog, or new food sensitivities might signal gut damage. Your microbiome affects everything from mood to cancer risk. Poor gut health lets toxins enter your bloodstream. This triggers inflammation that drives metabolic problems and hormone imbalances.
You can restore gut health in weeks with targeted interventions. Add 25-35 grams of varied prebiotic fiber daily from multiple sources. Take spore-based probiotics that survive stomach acid. Use L-Glutamine at 5-10 grams daily to repair gut lining. Add butyrate supplements at 300-600mg daily. These steps work together to rebuild your gut barrier and reduce inflammation.
- Spore-based Probiotics
- Hardy probiotic strains that survive stomach acid better than regular probiotics.
- SCFA (Short-Chain Fatty Acids)
- Beneficial compounds made when gut bacteria break down fiber.
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- L-Glutamine
- An amino acid that helps fuel and repair your gut lining.
- Microbiome
- The community of trillions of bacteria living in your gut that influence health.
- Butyrate
- A fatty acid made by gut bacteria that keeps your gut lining healthy.
- Prebiotic Fiber
- Types of fiber that feed the good bacteria in your gut.
- B12
- An essential vitamin synthesized by gut microbes that supports nerve function and DNA production.
- Calprotectin
- A protein biomarker found in stool that indicates inflammation in the gastrointestinal tract.
- CRP
- C-reactive protein is a blood marker produced by the liver indicating systemic inflammation.
- estrogen
- A steroid hormone involved in reproductive health, bone density, and metabolic regulation.
- Glutamine
- An amino acid used as a supplement to repair and maintain the gut lining.
Most men in midlife focus on their testosterone, cholesterol, or weight. But the 30-foot-long gut running through your core is quietly steering these very systems. Your gut microbiome—the 38 trillion bacteria living within you—acts as a hidden command center. These microbes produce 95% of your serotonin, synthesize vitamins like K2 and B12, and help regulate immune function.
As you age, your microbiome diversity naturally declines. This process is accelerated by common medications, processed foods, and stress. Men between 40 and 65 are especially at risk: the very drugs often prescribed for cholesterol, heartburn, or pain can damage the gut lining and shift your bacterial balance. A recent meta-analysis showed that low microbiome diversity in men over 40 was linked to higher rates of metabolic syndrome, heart disease, depression, and even early death [1].
This means your gut is not a side issue—it’s a central regulator of your metabolism, immunity, and mental health. If you ignore your gut, you may be undermining every other health goal. Next, you’ll see how the microbiome shapes your risk for inflammation, hormone imbalance, and cancer.
For men in their 40s, 50s, and 60s, gut health becomes the upstream regulator for nearly every system. When your gut lining weakens and becomes 'leaky,' bacterial toxins (like LPS) can slip into your blood. This fuels low-grade inflammation that drives insulin resistance, fatty liver, and hardening of the arteries.
Your gut also communicates directly with your brain through the vagus nerve. When your microbiome is out of balance, it can trigger or worsen depression, anxiety, and brain fog—symptoms often chalked up to 'stress' or 'aging.'
Your gut bacteria even help process hormones. The “estrobolome” is a collection of gut bacteria that determines how much estrogen is recycled in your body. If this system goes wrong, you can end up with an unfavorable testosterone-to-estrogen balance, a common midlife problem. On top of that, gut dysfunction makes it harder to absorb nutrients like magnesium, zinc, and B12, chipping away at your energy, muscle function, and immunity. As if that weren't enough, your risk for colon cancer climbs sharply in this age group—and your microbiome may determine whether you develop cancer, even if your lifestyle matches others who don’t. The next section will show you what biomarkers you can track to get a clear picture of your gut health.
Understanding your gut health starts with tracking the right biomarkers. Zonulin is a protein that reflects how 'leaky' your gut is. The standard range is below 30 ng/mL, and optimal is as low as possible. High zonulin signals a compromised gut barrier and is linked to autoimmune disorders and metabolic issues. Improving diet and reducing stress can lower zonulin, often within weeks to months.
Calprotectin, tested in your stool, measures gut inflammation. Healthy adults should have levels below 50 mcg/g. If your calprotectin is high, it points to active inflammation in your gut lining, which can be tracked as you make changes.
Your Microbiome Diversity Index, available from companies like Viome or Thorne, should be in the upper quartile for your age. Higher diversity means greater resilience and better health outcomes. Diversity can improve within a few weeks of dietary or supplement adjustments, especially with increased prebiotic fiber. hs-CRP, a blood test, should be below 1.0 mg/L. If it’s elevated and you don’t have joint pain, infection, or obvious illness, your gut could be the culprit. LPS-Binding Protein (LBP) should be under 10 mcg/mL. High LBP, especially with high CRP, is a sign that your gut is letting toxins into your bloodstream.
Finally, check your SCFA (short-chain fatty acid) profile, particularly butyrate. Butyrate in the upper quartile is ideal, since it fuels gut cells and keeps your barrier strong. Low butyrate means your diet is low in fermentable fiber, or your microbiome is depleted. Each of these markers interacts with the others—improving one often helps the rest. Next, we’ll dive into concrete actions you can use to move these biomarkers in the right direction.
Many common medications systematically damage your gut health. Proton pump inhibitors (PPIs) reduce gut diversity by 20% in men over 40 within six months of use. They lower stomach acid, allowing harmful bacteria to overgrow in the small intestine. NSAIDs like ibuprofen directly damage gut lining cells, increasing intestinal permeability by 30-50% within hours of use.
Antibiotics devastate gut diversity for 6-12 months after a single course. Even short antibiotic treatments can reduce beneficial bacteria by 90% temporarily. For men taking multiple gut-damaging medications, these effects compound and systematically dismantle your microbiome.
Work with your doctor to review medication necessity. Limit PPI use to the shortest duration possible. Consider targeted alternatives to NSAIDs for pain management. If you must continue these medications, add protective strategies like spore-based probiotics and prebiotic fiber to minimize damage. These changes can help restore your gut's balance and protect against chronic inflammation.
The most effective way to support your gut is by increasing the diversity of prebiotic fibers you eat. Aim for 25-35 grams daily, rotating between sources like psyllium husk, acacia fiber, partially hydrolyzed guar gum, inulin, and resistant starch from cooked-and-cooled potatoes or green banana flour. Each type feeds different bacteria, so variety is more important than total grams.
Spore-based probiotics, such as Bacillus subtilis and B. coagulans, survive stomach acid and establish themselves better than traditional probiotics. Clinical trials on products like MegaSporeBiotic show they can reduce endotoxin leakage (LPS) and improve microbial diversity. Standard dosing starts with one capsule daily, building up as tolerated.
L-Glutamine, at 5-10 grams daily, acts as fuel for your gut lining. Multiple trials show it helps reduce intestinal permeability, especially in stressed or compromised guts. Take it on an empty stomach for best absorption. Butyrate, either as sodium or calcium butyrate (300-600mg daily) or as tributyrin (a more absorbable form), directly nourishes your gut lining and calms inflammation. Tributyrin may be better tolerated and has less odor. Stack these interventions for best effect—fiber feeds the bacteria, probiotics help diversify them, and butyrate plus L-glutamine repair the lining. Next, we’ll examine the timeline for results and how to stack these tools for maximum synergy.
Gut health can improve surprisingly fast once you start targeted interventions. Microbiome diversity can rise within two to four weeks of adding multiple prebiotic fibers. Butyrate levels in your stool may increase within a month as beneficial bacteria return. Studies suggest that L-Glutamine’s effects on gut permeability are measurable within one to two weeks, especially in people with high stress or recent illness.
Spore-based probiotics can begin shifting your microbiome composition in as little as ten days, though the full benefit unfolds over several months with continued use. The synergy between interventions is key: prebiotic fibers feed the bacteria introduced by probiotics, which in turn produce more butyrate and other short-chain fatty acids. Butyrate and L-Glutamine together reinforce the gut barrier, reducing both zonulin and calprotectin levels.
For men who also review medications with their doctor, gut improvements may be even greater. Serial testing every three to six months is the best way to track your progress, especially if you’re pursuing multiple goals like lowering inflammation or improving mood. Up next, let’s look at early warning signs that your gut health needs attention—before bigger problems develop.
Gut dysfunction often flies under the radar until symptoms become obvious. For men in midlife, new or worsening bloating, gas, or irregular bowel movements are not just 'getting older'—they can signal dysbiosis, SIBO (small intestinal bacterial overgrowth), or increasing food intolerances. If symptoms flare after medications like PPIs or NSAIDs, your gut lining may be compromised.
Mental health shifts that show up alongside digestive symptoms are also a red flag. If you notice depression, anxiety, or brain fog emerging or worsening as your gut acts up, research suggests the gut-brain connection may be at play [1].
Pay attention to new food sensitivities, especially to foods you’ve eaten for years. Suddenly reacting to gluten, dairy, eggs, or high-fiber foods may mean your gut barrier is letting larger protein fragments through, triggering your immune system. SIBO testing (like a lactulose breath test) is widely available and can clarify if bacterial overgrowth is part of the picture. Spotting these signs early lets you intervene before chronic inflammation sets in. Next, let’s examine how gut health interacts with other health markers and interventions.
Gut health is deeply intertwined with other critical markers in men’s health. When your gut barrier breaks down, endotoxins like LPS cross into your blood, raising markers like hs-CRP and LBP. This not only drives inflammation but also worsens insulin resistance and metabolic syndrome. Improving your gut can lower these markers, making your whole system more resilient.
The gut’s estrobolome determines how much estrogen versus testosterone circulates. Dysbiosis can cause excess estrogen to be reabsorbed, which may tip your hormone balance in a direction that undermines muscle mass and libido. Nutrient absorption is also at stake: a compromised gut absorbs less magnesium, zinc, B12, and fat-soluble vitamins, even if your diet or supplement routine is solid. This can quietly chip away at your energy, mood, and immunity.
Finally, your microbiome can influence cancer risk. Certain bacteria (like Fusobacterium nucleatum) promote tumor growth, while others (butyrate producers) suppress it. Shifting your microbiome in a favorable direction may protect against colon cancer, which peaks in men 40-65. The next section will pull together key action steps and how to personalize your approach.
Your gut health protocol should fit your unique risk factors, symptoms, and medication use. Start by tracking your key biomarkers—zonulin, calprotectin, microbiome diversity, hs-CRP, LBP, and butyrate. Use these as a baseline and check every three to six months to see your progress.
Add diverse prebiotic fibers (25-35g daily from varied sources), spore-based probiotics, L-Glutamine (5-10g daily), and butyrate (300-600mg daily) as your foundation. Review your medications with your physician, especially PPIs, NSAIDs, and statins, to minimize harm while optimizing benefit. Pay attention to symptoms—digestive changes, new sensitivities, or mental health shifts all offer clues to your gut’s status.
Stack interventions for synergy: prebiotics and probiotics together, plus butyrate and L-Glutamine, reinforce the gut barrier and restore function. Serial testing and symptom tracking let you adjust your plan as you go. The key is consistency and diversity—your gut responds quickly to positive changes. In the final section, we’ll summarize the key lessons and offer a path forward.
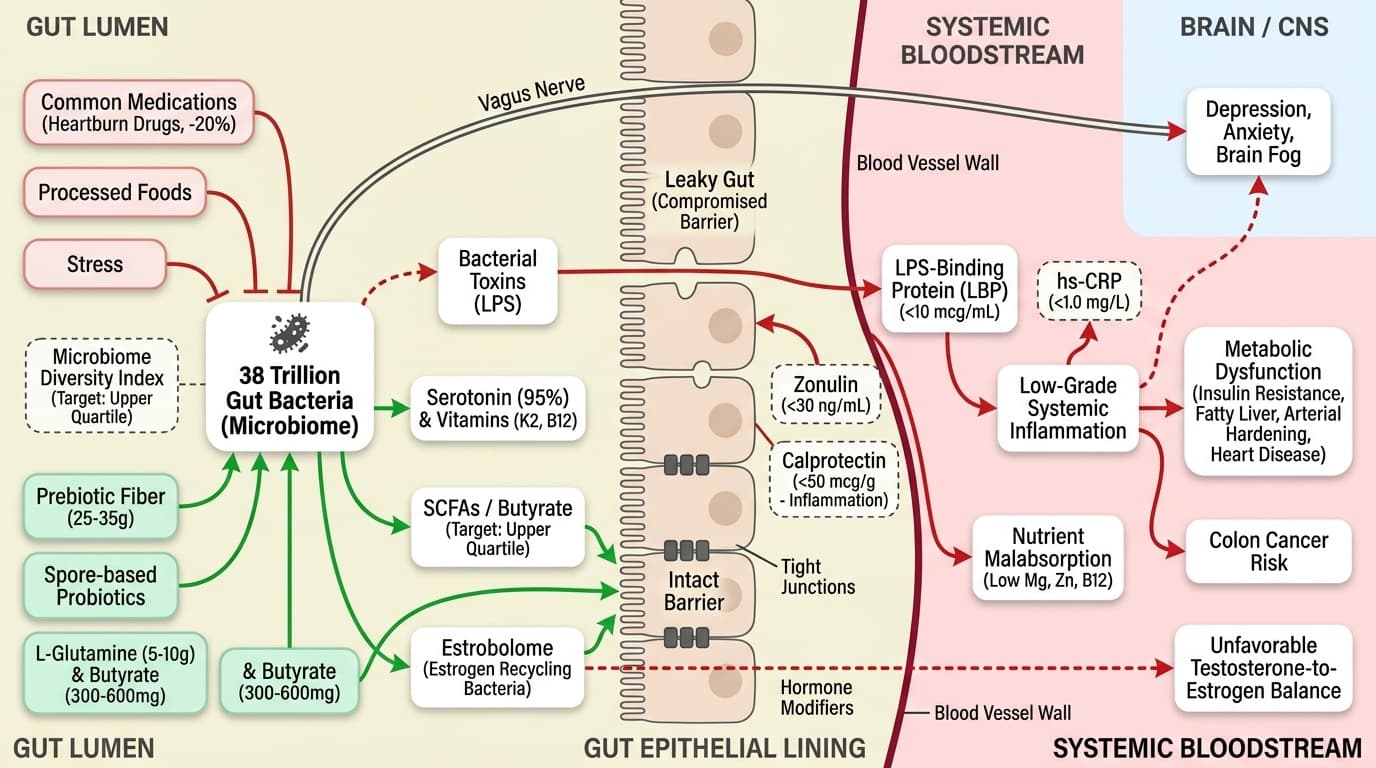
Gut Health in Midlife Men: The Hidden Driver of Your Health After 40
Why Your Microbiome Matters More Than Testosterone, Cholesterol, or Diet
Diagram glossary
- B12:
- An essential vitamin synthesized by gut microbes that supports nerve function and DNA production.
- Butyrate:
- A short-chain fatty acid produced by gut bacteria that nourishes the intestinal lining.
- Calprotectin:
- A protein biomarker found in stool that indicates inflammation in the gastrointestinal tract.
- CRP:
- C-reactive protein is a blood marker produced by the liver indicating systemic inflammation.
- estrogen:
- A steroid hormone involved in reproductive health, bone density, and metabolic regulation.
- Glutamine:
- An amino acid used as a supplement to repair and maintain the gut lining.
- insulin:
- A pancreatic hormone that regulates blood sugar levels and metabolic processes.
- LBP:
- Lipopolysaccharide-binding protein is a blood marker indicating an immune response to bacterial toxins.
- LPS:
- Lipopolysaccharide is a bacterial endotoxin that triggers systemic inflammation when entering the bloodstream.
- SCFA:
- Short-chain fatty acids are beneficial metabolites produced by gut bacteria fermenting dietary fiber.
- Zonulin:
- A protein that regulates the permeability of tight junctions in the intestinal wall.
Conclusions
For men between 40 and 65, gut health is a powerful—yet often overlooked—driver of well-being. The gut microbiome influences your metabolism, immune system, hormone balance, and even mental health. Age, common medications, and modern habits can quietly erode your gut’s resilience, but targeted interventions can restore diversity and function within weeks. By tracking the right biomarkers, adding diverse fibers, using targeted probiotics, and reviewing your medications, you can quickly see meaningful improvements. Treat your gut as a central pillar of health, not a side issue, and you’ll build a more resilient foundation for all your other goals.
Most of the evidence for gut interventions comes from clinical trials on specific populations, and results may vary based on your genetics, diet, and medication use. Stool-based microbiome testing provides valuable insights but is not yet standardized across labs. Some interventions, like spore-based probiotics or tributyrin, are newer and have moderate but not overwhelming evidence. Always consult your physician before major changes, especially if you have underlying gut conditions or are on multiple medications.
Track this in your stack
See how probiotics relates to your health goals and monitor changes in your biomarkers over time.
Sources (1)
This article informs how supplementation moves 1 marker.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
