Niacin Raises HDL 21% But Fails to Cut Heart Attacks: The Biomarker Trap That Fooled Cardiologists for Decades
Why spectacular lab improvements don't always translate to better health outcomes
You might think that if a supplement boosts your 'good' cholesterol, your heart is automatically safer.
Niacin, a form of vitamin B3, seemed to be that miracle—raising HDL by over twenty percent. But decades of research show that better lab numbers do not always mean fewer heart attacks. Let’s dig into why that is, what niacin really does in your body, and how you can approach heart health with the full picture in mind.
- HCAR2 receptor (GPR109A)
- A receptor niacin activates on fat and immune cells. It helps explain niacin’s lipid and inflammation effects.
- Extended-release (ER) niacin
- A slow-release niacin form that reduces flushing. It can still affect glucose, uric acid, and homocysteine.
- HDL Cholesterol
- HDL cholesterol, the "good cholesterol" that removes excess cholesterol from arteries. higher levels are cardioprotective.
- NAD+
- A molecule your cells use for energy and repair. Niacin is one vitamin source used to make NAD+.
- Glucose
- Blood sugar level, the primary energy source for cells. Fasting glucose is normal, prediabetes, ≥126 suggests diabetes.
- Hemoglobin A1c
- Average blood sugar over the past 2-3 months by assessing glycated hemoglobin. each 1% increase raises cardiovascular risk by 18%.
- Adiponectin
- Protective adipokine that enhances insulin sensitivity and reduces inflammation. low levels predict type 2 diabetes and cardiovascular disease.
- HCAR2
- A receptor on fat and immune cells activated by niacin to alter metabolism.
- HDL
- High-density lipoprotein, often called good cholesterol, which helps remove other cholesterol from blood.
- homocysteine
- An amino acid in the blood linked to an increased risk of cardiovascular disease.
You wake up early, grab your coffee, and scroll through your latest lab results on your phone. The numbers look good. HDL cholesterol, which your doctor called the 'good guy', is up. Triglycerides are down. Maybe you started taking niacin a few months back, hoping to nudge your heart health in the right direction. The sense of victory is real—after all, who doesn’t want proof their efforts are working?
But as you head out the door, you can’t help but wonder—does a better lab result really mean your heart is safer? For decades, even top cardiologists believed that boosting HDL with niacin would protect you from heart attacks. It seemed logical. More HDL should mean cleaner arteries, right? Yet, the science tells a more complicated story. Sometimes, what looks like progress on paper doesn’t translate to real-world protection.
That brings us to the heart of today’s question: Is niacin’s boost to your numbers actually helping your heart, or could it be a case of fixing the scoreboard while the game stays the same? Let’s look at why this matters, how niacin really works inside your body, and what you need to know to make decisions for your own heart health.
Cholesterol is one of those words that can make you tense up at the doctor’s office. There’s 'good' HDL, 'bad' LDL, and triglycerides—all swirling around in your blood. For years, doctors aimed to raise HDL and lower LDL. It made sense because people with higher HDL tend to have fewer heart attacks. Niacin, also known as vitamin B3, became a favorite supplement because it could quickly nudge the numbers in the right direction.
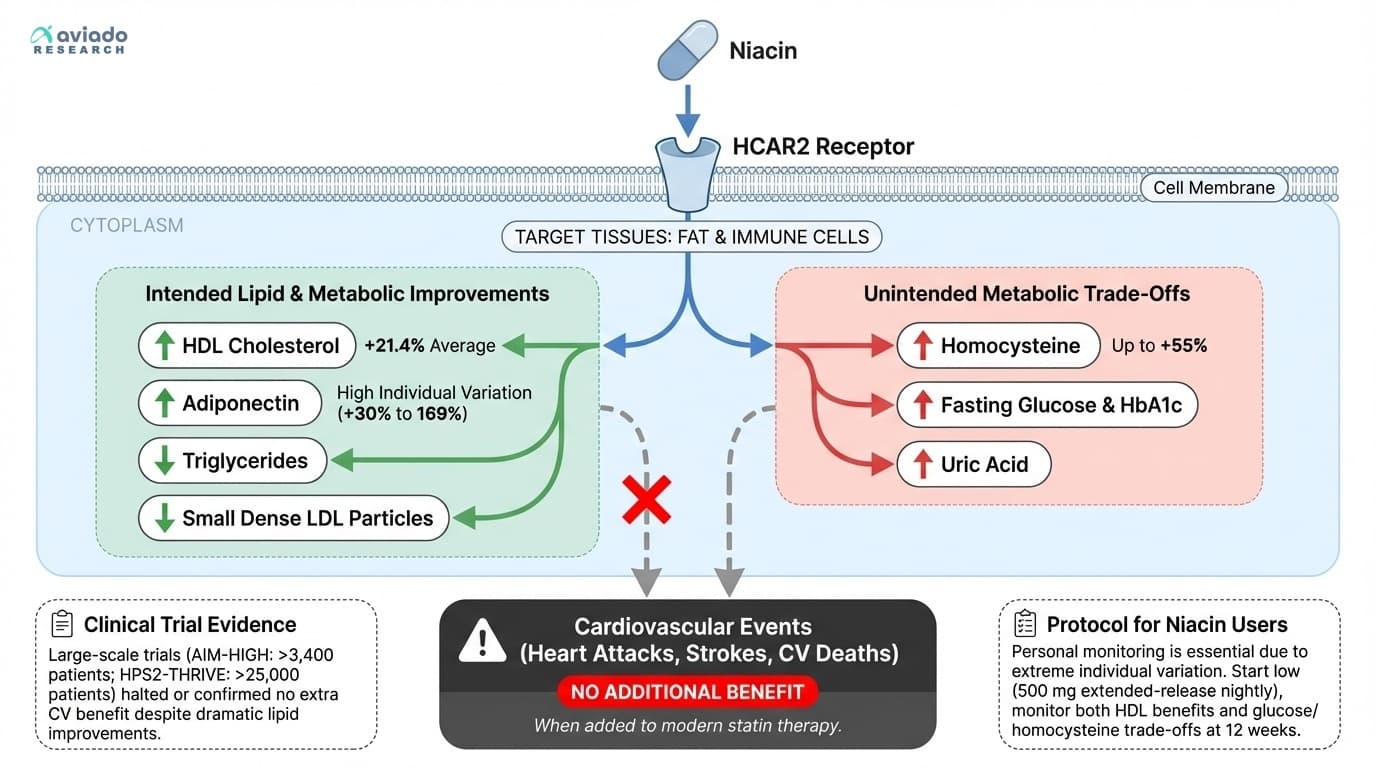
Here’s how niacin works: When you take it, it activates a receptor called HCAR2 on the surface of fat cells and immune cells. This sets off a cascade that decreases the breakdown of fats stored in your tissues. As a result, fewer fatty acids flood into your liver, which means your liver produces less of the bad cholesterol. At the same time, niacin increases the particles that carry HDL, helping to remove cholesterol from your arteries.
It sounds perfect in theory. In fact, a comprehensive review that pooled data from over thirty-five thousand participants showed that niacin increased HDL by about twenty-one percent. The supplement also decreased triglycerides and improved the quality of LDL, making it less likely to cause plaque buildup.
But here’s where biology throws a curveball. The relationship between cholesterol numbers and actual heart protection is not as simple as it seems. Raising HDL with niacin does not automatically make your arteries healthier. Your heart is influenced by dozens of pathways—some of which niacin affects, and others it does not. Understanding why perfect labs don’t always mean perfect health is the key to navigating your own choices safely. So what do the big studies actually show?
Let’s talk about the numbers that matter. When you check your cholesterol profile, you usually see HDL, LDL, and triglycerides. Niacin is famous for raising HDL cholesterol, sometimes by as much as twenty-one percent, and lowering triglycerides. On paper, these are wins. But what about the numbers behind those numbers?
Large clinical trials like AIM-HIGH and HPS2-THRIVE put niacin to the test. These studies followed tens of thousands of people. The goal was to see whether niacin, added to standard statin therapy, could prevent heart attacks, strokes, or cardiovascular deaths. The result was both surprising and sobering. Despite dramatic improvements in HDL and triglycerides, niacin did not reduce the number of heart attacks or strokes compared to statin therapy alone. In fact, the trials were stopped early because no benefit was seen.
So what does this mean for you? It means that while your HDL number can look better, the real measure of heart health—avoiding heart attacks—may not improve just because you take niacin. This is what researchers call the 'biomarker trap.' It’s the gap between what you can measure on a lab report and what actually protects your life.
There’s more to the story. Niacin can also influence other markers. For example, it raises adiponectin, a hormone that supports insulin sensitivity and healthy metabolism. But it can also increase homocysteine, which in high amounts is linked to higher cardiovascular risk. Niacin sometimes nudges fasting glucose and hemoglobin A1c up, making blood sugar control harder for some people.
If you’re thinking about niacin, you’ll want to keep an eye on more than just cholesterol. Track HDL and LDL, but also check fasting glucose, hemoglobin A1c, homocysteine, and uric acid. That full set gives you a much clearer picture of whether niacin is helping or quietly causing harm. The right biomarkers help you avoid the trap of celebrating numbers that don’t tell the whole story. Now, let’s look at what the research says about niacin as a supplement and how to use it safely.
Niacin is one of the oldest cholesterol-lowering supplements around. People have used it for decades, sometimes at very high doses. But just because it works on your lab numbers doesn’t mean it’s risk-free or equally effective for everyone.
Most of the research uses extended-release niacin, which is less likely to cause the intense facial flushing that immediate-release forms often trigger. The typical starting dose is five hundred milligrams taken at night, usually with food to reduce flushing. After a week, if you tolerate it, you can consider increasing to one thousand milligrams nightly. The sweet spot for most people falls between five hundred and one thousand milligrams per day. Higher doses may bring more side effects without extra health benefit.
The mechanism behind niacin’s effects is tied to how it alters fat metabolism. By dialing down the release of free fatty acids from your fat stores, niacin forces your liver to make less LDL cholesterol. It also enhances the recycling of HDL, pulling cholesterol out of your arteries. These changes are visible on your next lipid panel, usually within twelve weeks.
But the same pathway can have unwanted effects. Niacin often increases homocysteine levels by as much as fifty-five percent in some people. This happens because niacin interferes with methylation, a process your body uses to detoxify and manage inflammation. High homocysteine is linked to higher risk for both heart disease and stroke. Niacin can also push fasting glucose and hemoglobin A1c higher, especially in people already at risk for diabetes.
If you want to use niacin, start low, go slow, and monitor carefully. Check your full lipid panel, homocysteine, fasting glucose, hemoglobin A1c, and uric acid before you start. Repeat labs after twelve weeks, then every six months if you continue. This gives you a safety net. If you notice rising homocysteine or blood sugar, you can reconsider your approach. And always talk to your doctor before adding niacin, especially if you take other medications or have a history of liver issues.
Niacin is only one lever among many for improving heart health. While supplements can nudge your numbers, lifestyle shifts create long-term change that medications simply can’t match. If you want to protect your heart, here’s where the science points you.
Exercise is a powerhouse for raising HDL and improving insulin sensitivity. Aim for at least one hundred fifty minutes of moderate aerobic activity each week. This could be brisk walking, cycling, swimming, or any movement that gets your heart rate up and keeps it there. Regular exercise not only boosts your HDL but also improves the function of each particle, making it more effective at clearing cholesterol from your arteries. Mechanistically, exercise stimulates enzymes that help transfer cholesterol from your tissues back to your liver for disposal.
Nutrition matters just as much. Diets high in fiber, especially from whole grains, vegetables, and legumes, can lower LDL cholesterol and support healthy HDL. Include omega-3 rich foods like fatty fish or consider a high-quality fish oil supplement. These fats reduce inflammation and help stabilize the lining of your arteries. Limit saturated and trans fats, which can counteract the benefits of niacin and other interventions.
Sleep is an underrated tool for heart health. Poor sleep raises cortisol and disrupts blood sugar control, both of which can worsen cholesterol numbers and increase your risk for heart disease. Prioritize at least seven hours of quality sleep each night. Keep a regular sleep schedule and create a calming bedtime routine. This helps regulate the hormones that influence both fat metabolism and inflammation.
Stress management rounds out the lifestyle picture. Chronic stress can raise blood pressure, disrupt glucose control, and even lower HDL. Simple practices like deep breathing, meditation, or short daily walks can reduce the impact of stress hormones on your heart. In short, the best heart protection comes from a combination of targeted supplements like niacin—when appropriate—and consistent lifestyle choices.
Most people think heart trouble arrives with dramatic chest pain or a big scare, but early signs are often subtle and easy to overlook. If you’re using niacin, or thinking about it, knowing what to watch for can make all the difference.
One red flag is unexpected changes in your energy or exercise ability. If you find yourself more tired during routine activities or notice that walks or workouts feel harder, it could signal a shift in cardiovascular function or blood sugar control. This is especially true if you’ve recently changed your supplement regimen.
Keep an eye on skin flushing, which is common but usually harmless. More concerning are symptoms like new muscle aches, joint pain, or dark urine, which can point to liver stress. Niacin can also increase uric acid, which sometimes triggers gout attacks—sudden pain and swelling in a joint, often the big toe.
Blood sugar changes are another early warning. If you notice increased thirst, frequent urination, or blurry vision, it could mean your blood sugar is climbing. Niacin can push hemoglobin A1c and fasting glucose up in some people, especially if you have prediabetes or metabolic syndrome.
Finally, pay attention to subtle cognitive changes. Brain fog or difficulty concentrating can sometimes be linked to higher homocysteine levels, which niacin can raise. If you notice these symptoms, it’s a signal to check your biomarkers and talk to your healthcare provider. Early action can help you adjust your plan before small problems become big ones. So how do you put all of this together for your long-term health?
Niacin’s story is a powerful lesson in the difference between fixing your lab numbers and truly protecting your heart. Decades of research prove that even when a supplement like niacin raises HDL dramatically, it may not lower your risk for heart attacks or strokes. The numbers on your lab report matter, but they are only part of the picture.
If you choose to use niacin, treat it as a personal experiment. Start with low doses, increase gradually, and monitor a complete set of biomarkers—not just cholesterol, but also glucose, hemoglobin A1c, homocysteine, and uric acid. This approach helps you catch both the expected benefits and the potential silent harms.
Remember, the most powerful heart protection comes from combining targeted supplements with daily lifestyle choices. Exercise, nutrition, sleep, and stress management all work together to build a resilient cardiovascular system. Supplements can help, but they should never be your only strategy.
The real takeaway is this: Do not settle for perfect labs if they are not matched by better health. Use the science to guide your decisions, measure what matters, and partner with your healthcare provider for a plan that fits you—not just the 'average' person in a study. Heart health is about more than numbers. It is about feeling strong, staying active, and living the life you want—now and for decades to come.
Niacin Raises HDL 21% But Fails to Cut Heart Attacks: The Biomarker Trap That Fooled Cardiologists for Decades
Why spectacular lab improvements don't always translate to better health outcomes
Diagram glossary
- adiponectin:
- A protein hormone involved in regulating glucose levels and fatty acid breakdown.
- glucose:
- A simple sugar that serves as the primary energy source for living cells.
- HCAR2:
- A receptor on fat and immune cells activated by niacin to alter metabolism.
- HDL:
- High-density lipoprotein, often called good cholesterol, which helps remove other cholesterol from blood.
- homocysteine:
- An amino acid in the blood linked to an increased risk of cardiovascular disease.
- insulin:
- A pancreatic hormone that regulates blood glucose levels by facilitating cellular sugar uptake.
- LDL:
- Low-density lipoprotein, often called bad cholesterol, which contributes to arterial plaque formation.
- Niacin:
- A B vitamin used therapeutically to improve lipid profiles and alter cholesterol levels.
Conclusions
Niacin is a clean example of the biomarker trap. It can raise HDL and improve parts of your lipid panel, yet large modern trials found no added drop in heart attacks or strokes when niacin was added to statins. Niacin can also raise homocysteine and worsen blood sugar in some people, so “better cholesterol” may come with hidden costs. If you try niacin, your best protection is not hope—it is measurement: check lipids plus HbA1c, fasting glucose, homocysteine, and uric acid before and after you start.
Most major outcome trials tested niacin added to statins, so results may not fully apply to people who cannot take statins. Many benefits discussed (like adiponectin increases) are biomarker outcomes, not proven reductions in heart events. Reports of homocysteine and glucose worsening vary by population, dose, and formulation, and not all trials measured these consistently. Evidence for neurological and eye benefits is early and mostly observational or mechanistic, not based on large randomized outcome trials.
Track this in your stack
See how niacin relates to your health goals and monitor changes in your biomarkers over time.
Sources (8)
This article informs how supplementation moves 1 marker.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
