The Four Blood Signals That Predict Brain Aging—and What Most Doctors Miss
A comprehensive action plan for your next doctor visit
Most people think brain health is about avoiding disease.
But surprising research shows four simple blood tests can predict whether your brain is aging faster or slower than expected. Your doctor probably doesn't order these tests. They're available at any lab. They catch warning signs years before memory problems start.
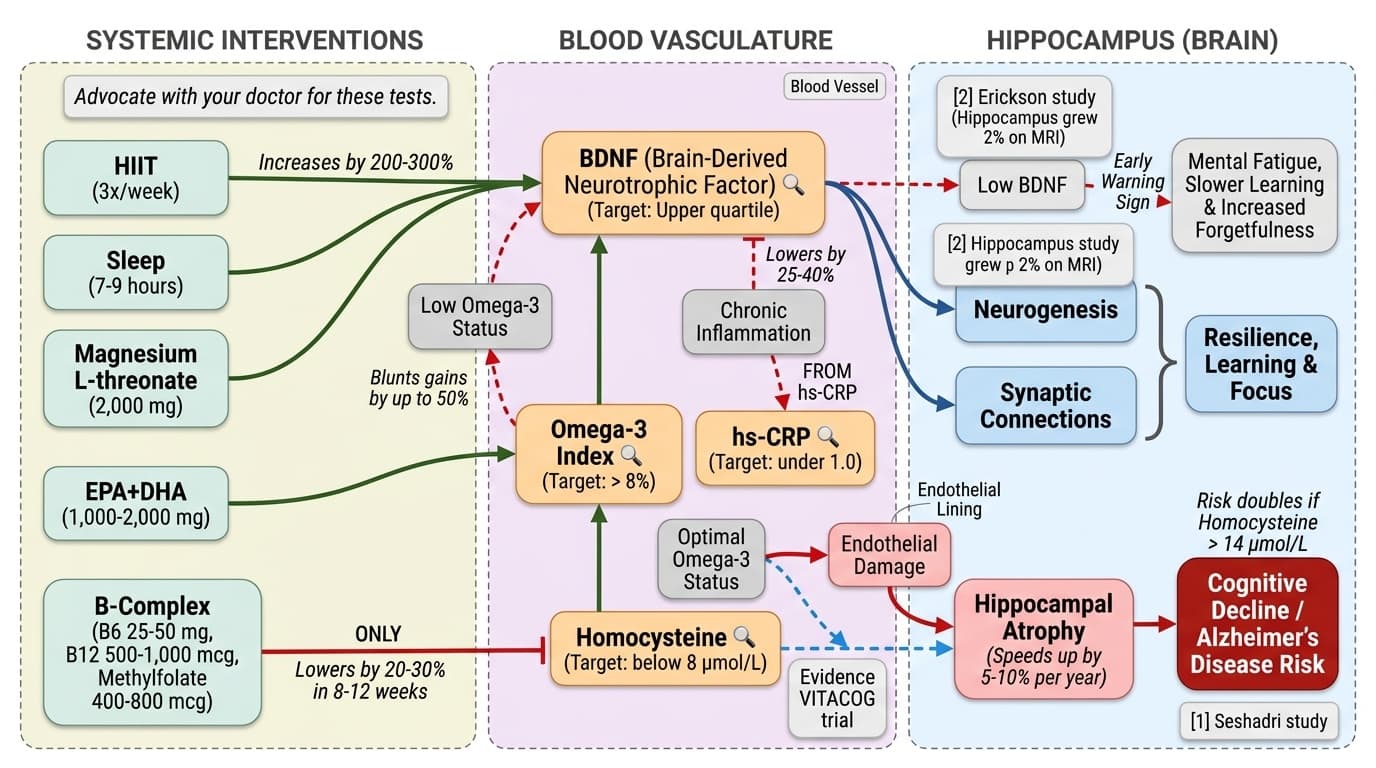
You can take control of your brain's future. Four blood signals tell the story: BDNF shows brain growth. Homocysteine reveals hidden toxicity. Omega-3 index measures brain fuel. hs-CRP tracks inflammation. Testing all four together gives you a complete picture. Most doctors miss this because it's not on standard panels.
Target these numbers: homocysteine below 8, omega-3 index above 8%, hs-CRP under 1.0. Take 1,000-2,000 mg EPA+DHA daily. Add B-complex with 400-800 mcg methylfolate. Do high-intensity interval training 3 times per week. Recheck in 8-12 weeks to track progress.
The Four Blood Signals That Predict Brain Aging—and What Most Doctors Miss
A comprehensive action plan for your next doctor visit
Diagram glossary
- B12:
- A water-soluble vitamin essential for nerve function, brain health, and red blood cell production.
- B6:
- A water-soluble vitamin involved in amino acid metabolism, neurotransmitter synthesis, and brain health.
- BDNF:
- A protein that promotes the survival, growth, and maintenance of neurons in the brain.
- CRP:
- A blood marker that indicates the level of systemic inflammation in the body.
- DHA:
- An omega-3 fatty acid essential for brain health, cognitive function, and eye development.
- EPA:
- An omega-3 fatty acid that helps reduce inflammation and supports cardiovascular and brain health.
- HIIT:
- A cardiovascular exercise strategy alternating short periods of intense exercise with recovery periods.
- Homocysteine:
- An amino acid in the blood linked to neurotoxicity and cardiovascular risk at high levels.
- methylfolate:
- The biologically active form of vitamin B9 necessary for DNA synthesis and neurological function.
- MRI:
- A medical imaging technique using magnetic fields to generate detailed images of internal organs.
- Omega-3 Index
- A measure of the amount of EPA and DHA (healthy fats) in your red blood cells, reflecting your brain's fatty acid status.
- EPA+DHA
- EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid) are the two key active omega-3 fatty acids found in fish oil supplements; together they are the forms your body and brain can directly use.
- Phospholipid Forms
- A way of packaging omega-3 fatty acids (like EPA and DHA) inside a fat molecule structure called a phospholipid, which is the same form found naturally in fish roe and krill oil; this structure may allow better absorption than standard fish oil.
- HIIT (High-Intensity Interval Training)
- Short bursts of intense exercise that can raise BDNF more effectively than steady-state cardio.
- DHA
- Docosahexaenoic acid, a specific omega-3 fatty acid that is a primary structural building block of brain cell membranes, making it especially critical for cognitive function and brain health.
- BDNF
- A protein that supports neuron growth and survival, often called 'fertilizer for the brain.' Higher levels associated with better memory and mood.
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- B12
- A water-soluble vitamin essential for nerve function, brain health, and red blood cell production.
- B6
- A water-soluble vitamin involved in amino acid metabolism, neurotransmitter synthesis, and brain health.
- CRP
- A blood marker that indicates the level of systemic inflammation in the body.
- EPA
- An omega-3 fatty acid that helps reduce inflammation and supports cardiovascular and brain health.
- HIIT
- A cardiovascular exercise strategy alternating short periods of intense exercise with recovery periods.
Why Your Next Checkup Misses the Brain—and How You Can Fix It
At your next doctor visit, you’ll likely get a standard set of blood tests: cholesterol, blood sugar, maybe a complete blood count. But if you look closely, you’ll notice something missing. There is no routine panel for brain health. Your brain—the organ that defines your personality, memory, and independence—doesn’t show up anywhere on the standard order form. That’s not because the science is lacking. It’s because medicine hasn’t caught up to what we now know about early brain aging.
Four blood tests, all available at major labs and covered by most insurance plans, can give you a snapshot of your brain’s health years before symptoms appear. These are not just academic tools; they are practical, actionable signals that can help you take control of your brain’s future. The challenge: most doctors do not order them unless you specifically ask, because they are not part of the default checklist. If you want these insights, you need to advocate for yourself.
Understanding how these markers work together can empower you to make targeted changes—before memory slips, mood changes, or cognitive fog set in. In the next sections, you’ll learn exactly what to test, what the results mean for your brain, and how to move each number in the right direction.
Signal One: BDNF—The Brain’s Growth Signal
BDNF, or Brain-Derived Neurotrophic Factor, acts as your brain's primary growth signal. It drives neurogenesis—helping you form new brain cells, especially in the memory-critical hippocampus. BDNF also strengthens synaptic connections, which are crucial for learning, focus, and adapting to new challenges. When BDNF levels are high, your brain is more resilient and better able to repair itself after stress or injury.
There is no universal standard range for BDNF yet, but research suggests you want to be in the upper quartile for your age group. Most people never measure it, because standard labs don't offer the test. Specialty labs can check serum BDNF with a simple blood draw. Early warning signs of low BDNF include mental fatigue, slower learning, and increased forgetfulness—symptoms that may be especially noticeable in women in perimenopause or adults over 50.
High-intensity interval training (HIIT) is the most powerful way to raise BDNF. Compared to steady-state cardio, HIIT can increase BDNF by 200-300%. A 2011 study led by Erickson showed that regular aerobic exercise increased BDNF and actually grew the hippocampus by 2% on MRI scans [2]. Omega-3 supplementation at 1,000-2,000 mg EPA+DHA daily, magnesium L-threonate at 2,000 mg, and 7-9 hours of quality sleep can also boost BDNF. You may start seeing changes in BDNF within 2 to 4 weeks of lifestyle shifts. BDNF interacts with inflammation and omega-3 status: low omega-3 can blunt BDNF gains from exercise by up to 50%, while chronic inflammation (high hs-CRP) can lower BDNF by 25-40%. Knowing your BDNF number lets you see if your interventions are working and helps tailor your brain health plan.
Signal Two: Homocysteine—The Hidden Brain Toxin
Homocysteine is an amino acid produced during protein metabolism. When levels rise above optimal, homocysteine becomes directly toxic to your brain. It damages the endothelial lining of blood vessels, speeds up hippocampal atrophy by 5-10% per year, and increases the risk of cognitive decline. Standard labs may report anything below 15 μmol/L as normal, but research on neuroprotection sets a much stricter functional target: you want homocysteine below 8 μmol/L for optimal brain health.
Elevated homocysteine is a silent risk. A landmark study from Seshadri and colleagues found that people with homocysteine above 14 μmol/L had double the risk of developing Alzheimer's disease [1]. Early warning signs are subtle—brain fog, low mood, and slower processing speed. These are often missed in adults under 60, but are especially critical if you have a family history of dementia or cardiovascular disease.
Homocysteine responds dramatically to B vitamin supplementation—specifically, B6 (25-50 mg), B12 (500-1,000 mcg), and methylfolate (400-800 mcg daily). Here's the key insight: according to the VITACOG trial, B vitamins only lower brain atrophy if your omega-3 index is also optimal [1][1]. The dose-response is clear—B vitamins can reduce homocysteine by 20-30% in 8-12 weeks. Most people see measurable reductions in 8 to 12 weeks after starting supplements. Homocysteine interacts with both inflammation (hs-CRP) and omega-3 status, so you need to check all three to get the full picture. Testing homocysteine is simple—a fasting blood sample at any lab will do. Ask your doctor for a plasma homocysteine test and target a result below 8 μmol/L.
Signal Three: Omega-3 Index—Building Blocks for Your Brain
The omega-3 index measures the percentage of EPA and DHA—two crucial omega-3 fats—incorporated into your red blood cell membranes. This number directly reflects your long-term omega-3 intake and, by extension, your brain's structural integrity. DHA makes up about 40% of the polyunsaturated fats in your brain. When your omega-3 index falls below 4%, research shows your risk of smaller brain volume increases by 20% and executive dysfunction rises sharply [1]. Most Americans hover between 4 and 5%, well below the neuroprotective threshold.
Aim for an omega-3 index above 8%. This target is linked to 37% lower risk of dementia and healthier brain aging. The test itself is accessible—a simple finger-prick blood sample, often available as a home kit for $50-75. Early warning signs of low omega-3 include dry skin, low mood, and increased forgetfulness. These are especially likely in older adults, vegetarians, and those who rarely eat fatty fish.
Taking daily EPA+DHA supplements is the most reliable way to raise your omega-3 index. Doses of 1,000-2,000 mg combined EPA+DHA per day are typical, but some people may need up to 3,000 mg if baseline levels are very low. The form matters: triglyceride or phospholipid forms are absorbed 50-70% better than ethyl esters. You'll see meaningful changes in your omega-3 index after 3 to 4 months of consistent supplementation. Omega-3s interact with B vitamins—without an omega-3 index above 8%, B vitamin therapy for homocysteine may not protect your brain [1][1]. Testing the omega-3 index tells you if your current supplement or diet plan is actually delivering brain benefits.
Signal Four: hs-CRP—The Inflammation Link
hs-CRP (high-sensitivity C-reactive protein) is your body's universal alarm signal for inflammation. While it's often used to assess heart risk, research shows that systemic inflammation and neuroinflammation are tightly linked. When hs-CRP is elevated—even in the absence of obvious illness—your brain faces accelerated aging, cognitive decline, and mood disorders.
The functional medicine target for hs-CRP is below 1.0 mg/L. Many standard labs consider up to 3.0 mg/L as "normal," but studies such as Satizabal 2012 show that people with hs-CRP above 2.0 mg/L in midlife had 40% faster cognitive decline and 60% higher dementia risk 25 years later [1]. Early warning signs of high inflammation include joint aches, poor recovery from exercise, and increased mental fatigue. These are especially important to watch in midlife adults, those with autoimmune conditions, and people under chronic stress.
You can lower hs-CRP through targeted interventions. Omega-3 supplementation at 2,000-3,000 mg EPA+DHA daily can reduce hs-CRP by 20-30%. Regular exercise lowers it by 15-25%. Anti-inflammatory nutrients like ashwagandha (300-600 mg daily) and curcumin (500-1,000 mg daily) provide additional reductions of 10-20%. Changes in hs-CRP can be seen as quickly as 4 to 8 weeks after starting interventions. High hs-CRP can suppress BDNF by 25-40% and worsen the effects of elevated homocysteine, making it crucial to monitor all these signals together. Testing hs-CRP is straightforward—a fasting blood test at any lab will provide accurate results.
The Interaction Effect—Why You Must Test All Four Signals
Each of these four blood signals tells you something important about your brain, but their true power comes from looking at them together. BDNF and omega-3 index both support the strength and flexibility of your brain’s synaptic connections. Meanwhile, homocysteine and hs-CRP both threaten those connections through toxicity and inflammation. Testing and optimizing all four gives you a complete map of your brain’s health trajectory.
The most striking finding comes from the VITACOG trial: B vitamin supplementation only slowed brain atrophy when omega-3 index was high enough [1][1]. If you only correct one marker without checking the others, you may miss the synergy that makes real brain protection possible. For example, raising BDNF through exercise works best when inflammation (hs-CRP) is low and omega-3 status is optimal. On the flip side, high homocysteine and chronic inflammation can cancel out the benefits of supplements or lifestyle changes.
This interaction effect means you need a holistic testing approach. If you address just one or two markers, you risk missing the bigger picture. Testing all four signals at the same time gives you actionable data to personalize your interventions and track your progress. In the next section, you’ll get a step-by-step guide to making this happen at your next doctor visit.
Your Next Doctor Visit: The Exact Tests and How to Use Them
You now know which markers matter most for brain aging. Here’s how to put this knowledge into action. At your next appointment, ask for these four tests: 1) serum BDNF (typically through a specialty lab), 2) plasma homocysteine, 3) omega-3 index (finger-prick home test or lab draw), and 4) hs-CRP. If your doctor is unfamiliar with these tests, bring this article and explain the rationale—each one is supported by strong evidence for brain health.
If you’re paying out of pocket, expect a total cost of $150 to $250 for all four tests. Many insurance plans will cover at least homocysteine and hs-CRP. If you’re already working on lifestyle changes—such as taking omega-3s, B vitamins, or exercising regularly—test now to get a baseline. Then, retest in 8 to 12 weeks to track your response. This time frame is based on published studies showing meaningful changes in all four markers over two to three months of intervention.
Bring your results to your next visit and discuss a plan to optimize any out-of-range numbers. For most adults, aiming for a homocysteine below 8, omega-3 index above 8%, hs-CRP under 1.0 mg/L, and BDNF in the upper quartile for age is a strong target. This approach puts you in control—turning abstract brain health ideas into concrete, trackable progress.
Conclusions
Four simple blood tests—BDNF, homocysteine, omega-3 index, and hs-CRP—offer the most practical, early-warning system for brain aging available today. Optimizing these markers can help you preserve cognitive function, protect against dementia risk, and make every day sharper and more productive. By testing all four together and personalizing your interventions, you can take proactive steps to support your brain health for decades to come.
While the evidence supporting these four biomarkers is strong, not all tests are available in every region or covered by standard insurance. Reference ranges for BDNF are not yet standardized for all ages or demographics. The interaction effects—especially between omega-3 index and B vitamin supplementation—are based on recent research but may not capture all genetic or lifestyle variables. Always consult a healthcare provider for personalized guidance, and remember that biomarkers are just one piece of the brain health puzzle.
Track this in your stack
See how brain cognitive biomarkers relates to your health goals and monitor changes in your biomarkers over time.
