The HPA Axis Traffic Switch: How Your Body Allocates Hormonal Resources Under Stress
A Comprehensive Guide to Understanding the Interplay Between Stress, Thyroid, and Sex Hormones
It's surprising how many people have normal thyroid tests but still feel exhausted and foggy. Your doctors might be missing a crucial connection. Your thyroid, stress hormones, and sex hormones don't work alone. They share resources like a budget.
When you're stressed for months, your body makes more cortisol. This steals resources from making active thyroid hormone and DHEA. You end up tired even with normal TSH. Women after menopause get hit hardest because their adrenal glands become their main hormone factory.
To fix this pattern, test free T3 (aim for 3.0-4.0 pg/mL), DHEA-S (target 100-200 mcg/dL for women over 40), and morning cortisol (under 18 mcg/dL is better). Many people need all three markers tested together, not just TSH. Managing stress becomes as important as any hormone therapy.
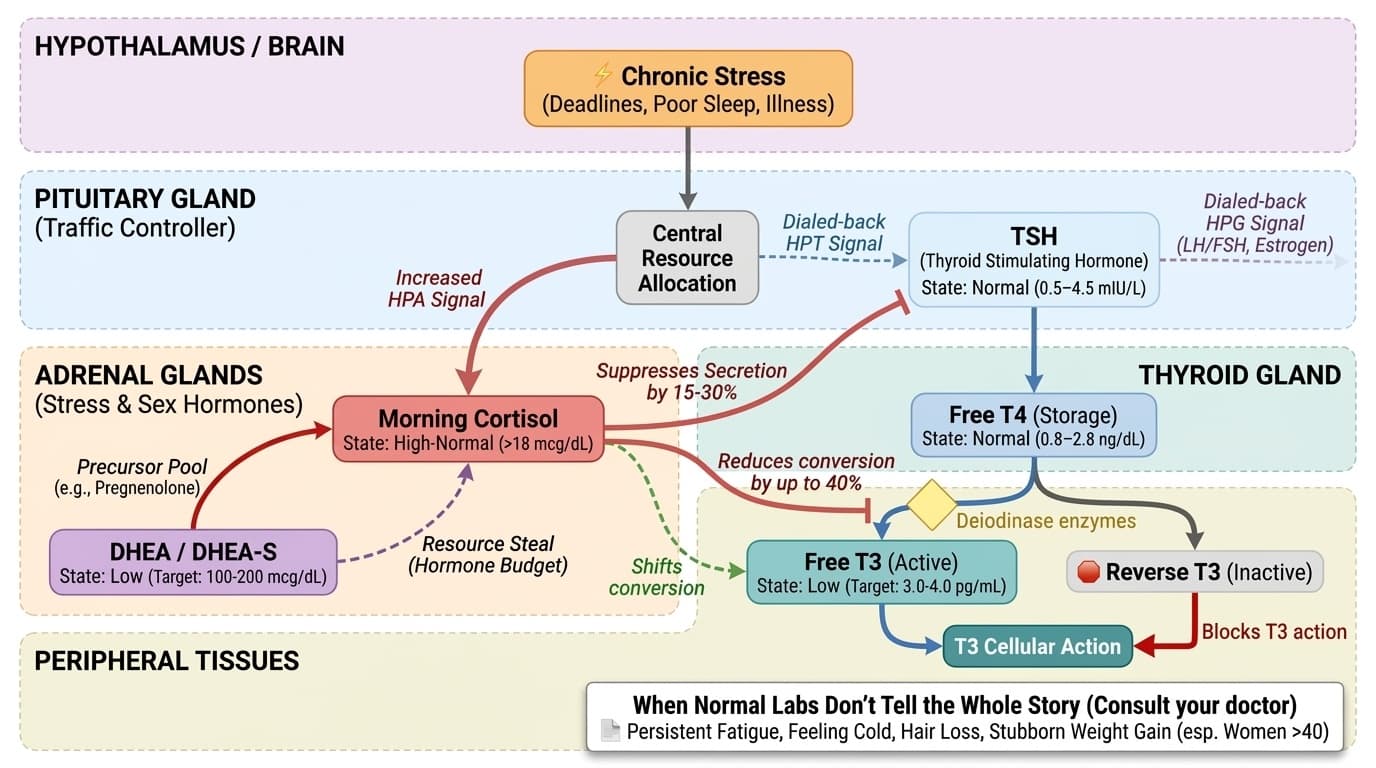
The HPA Axis Traffic Switch: How Your Body Allocates Hormonal Resources Under Stress
A Comprehensive Guide to Understanding the Interplay Between Stress, Thyroid, and Sex Hormones
Diagram glossary
- deiodinase:
- An enzyme responsible for converting inactive thyroid hormone into its active form within tissues.
- DHEA-S:
- An adrenal steroid hormone often measured to assess adrenal gland function and stress response.
- estrogen:
- A primary female sex hormone responsible for regulating the reproductive system and secondary characteristics.
- HPA:
- The hypothalamic-pituitary-adrenal axis is a complex neuroendocrine system regulating the body's stress response.
- HPG:
- The hypothalamic-pituitary-gonadal axis is a hormonal system that regulates reproductive function and sex hormones.
- HPT:
- The hypothalamic-pituitary-thyroid axis is a hormonal system responsible for regulating thyroid function and metabolism.
- LH/FSH:
- Pituitary hormones that work together to regulate the reproductive system and stimulate gonadal function.
- mcg/dL:
- A standard unit of concentration used in blood tests to measure hormone levels.
- mIU/L:
- A standard unit of measurement used in blood tests for hormones like TSH.
- ng/dL:
- A standard unit of measurement used in blood tests to quantify trace hormone concentrations.
- TSH:
- Thyroid-stimulating hormone is a pituitary hormone that triggers the thyroid to produce thyroid hormones.
- HPA Axis
- The body's central stress response system connecting the brain to adrenal glands. Chronic activation leads to elevated stress hormones and negative health effects.
- HPT Axis
- The hormonal system involving your hypothalamus, pituitary, and thyroid glands.
- Free T3
- Free triiodothyronine, the most metabolically active thyroid hormone. Low levels indicate impaired T4-to-T3 conversion or hypothyroidism.
- DHEA-S
- DHEA-sulfate, the most abundant adrenal androgen and cortisol precursor. low levels associated with fatigue.
- TSH
- Thyroid-stimulating hormone, the primary thyroid function screening test. elevated TSH indicates hypothyroidism, low values suggest hyperthyroidism.
- Cortisol
- Your main stress hormone released by adrenal glands. Morning levels above 18 mcg/dL may indicate chronic stress affecting other hormones.
- Pregnenolone Steal
- The theory that chronic stress diverts cholesterol toward making cortisol instead of sex hormones like DHEA and testosterone.
- deiodinase
- An enzyme responsible for converting inactive thyroid hormone into its active form within tissues.
- estrogen
- A primary female sex hormone responsible for regulating the reproductive system and secondary characteristics.
- HPA
- The hypothalamic-pituitary-adrenal axis is a complex neuroendocrine system regulating the body's stress response.
- HPG
- The hypothalamic-pituitary-gonadal axis is a hormonal system that regulates reproductive function and sex hormones.
- HPT
- The hypothalamic-pituitary-thyroid axis is a hormonal system responsible for regulating thyroid function and metabolism.
The Opening: When Normal Lab Results Don’t Tell the Whole Story
Imagine you visit your doctor because you feel exhausted all the time. Your hair is thinning, your weight isn’t budging, and you’re frustrated. The doctor orders a standard thyroid panel. Your TSH comes back in the normal range. Free T4, also normal. You go home with more questions than answers. Later, a different doctor checks your cortisol and DHEA-S on a separate day. Cortisol is high-normal; DHEA-S is low. Nobody puts the puzzle pieces together, because each number was checked in isolation.
But your body doesn’t see these hormones as separate. The real story is in the pattern. Your stress, thyroid, and sex hormone systems are all wired together through the HPA axis. When one part of the system faces a heavy load—like your stress response—the others may quietly turn down their output. This is why symptoms can show up even when labs look 'normal.'
Early warning signs of this pattern include persistent fatigue, feeling cold, hair loss, and stubborn weight gain, especially in women over 40. These symptoms are not just random—they often point to a resource allocation problem within your hormonal system. Understanding that your body is constantly balancing these axes sets the stage for deeper insight into your labs and your health journey.
The Traffic Controller: How the Pituitary Gland Directs Hormonal Flows
At the heart of your hormonal system sits the pituitary gland. Think of it as a traffic controller. The pituitary receives signals from the hypothalamus and coordinates three major hormone highways: the HPA axis (stress and cortisol), the HPT axis (thyroid hormones), and the HPG axis (sex hormones like estrogen, progesterone, and testosterone).
When your life gets stressful—chronic work deadlines, poor sleep, illness—the HPA axis demands more attention. The pituitary increases the signal for cortisol production, which helps you survive acute stress. But this increased traffic to the adrenal glands can mean less signaling and fewer resources available for your thyroid and sex hormone systems. These axes don’t shut down, but the pituitary dials them back. This phenomenon is especially pronounced during periods of chronic stress, as described in a comprehensive review by Tsigos and Chrousos, which outlined how the pituitary reallocates resources across these axes in response to ongoing demands [1].
For you, this means that during times of sustained stress, your thyroid and sex hormones may function at suboptimal levels—even if their primary signals (like TSH or LH/FSH) fall within the lab’s normal range. Recognizing this pituitary-managed resource allocation helps explain why symptoms can appear before lab abnormalities, and why holistic hormone assessment is crucial.
The Cortisol-Thyroid Connection: Why Stress Can Masquerade as Hypothyroidism
Cortisol is your body's main stress hormone. When its levels stay high for too long, it doesn't just manage stress—it starts to interfere with your thyroid system. Elevated cortisol suppresses TSH secretion from the pituitary by 15-30%, meaning your thyroid gets less of a 'go' signal. This can lead to normal or even low-normal TSH levels, masking underlying issues.
But the story goes deeper. Cortisol blocks the conversion of T4 (the storage form of thyroid hormone) to T3 (the active form your cells use). Instead, more T4 is converted to reverse T3, an inactive form that blocks T3 action. Bauer's 2008 work showed that chronic stress reduces T4-to-T3 conversion by up to 40% via cortisol's effect on deiodinase enzymes [2].
The standard ranges for TSH (about 0.5–4.5 mIU/L) and free T4 (0.8–2.8 ng/dL) may not reveal this problem. Optimal free T3 for most adults is 3.0–4.0 pg/mL, but under chronic stress, you may see free T3 drop below 3.0 even while TSH and T4 are 'normal.' These changes can show up within 4-6 weeks of sustained stress. Because cortisol and thyroid hormones interact at multiple levels, it's crucial to test free T3 and reverse T3, especially if you have ongoing fatigue, cold intolerance, or unexplained weight gain.
The Cortisol-Sex Hormone Connection: The Pregnenolone Steal and Its Limits
Your adrenal glands make cortisol and DHEA (the building block of sex hormones) from a common precursor: cholesterol. The 'pregnenolone steal' hypothesis suggests that, under chronic stress, your body channels more pregnenolone toward making cortisol, leaving less available for DHEA, testosterone, and estrogen. This idea, outlined by Parker in 1999, helps explain why people under chronic stress often have low DHEA-S and sex hormone levels [4].
However, this model is debated. Some researchers now argue that the main problem isn’t so much a shortage of upstream precursors, but rather direct suppression of sex hormone production by pituitary signaling. In other words, your pituitary may put the brakes on DHEA and sex hormone synthesis when the HPA axis is overactive. Heaney’s 2012 review explored this complex crosstalk, showing that both resource competition and signaling suppression can occur [5].
Standard DHEA-S ranges are about 35–430 mcg/dL for women, but optimal levels for women over 40 are often 100–200 mcg/dL. Chronic stress can cause DHEA-S to fall below this, sometimes in as little as a few weeks. Lower DHEA-S can mean lower downstream testosterone and estrogen, contributing to fatigue, low libido, and mood changes. These changes tend to happen together with high-normal or elevated cortisol, forming a recognizable pattern. It’s not just about one number—it’s about understanding how stress can quietly erode your hormonal reserve.
Reading the Pattern: Concordant Axis-Level Signatures
When it comes to your hormonal health, patterns matter more than isolated numbers. Instead of looking at TSH, cortisol, or DHEA-S in a vacuum, research suggests you should look for axis-level signatures—clusters of values that move together. Lennartsson's 2013 study of people with chronic burnout found a classic pattern: elevated cortisol (>18 mcg/dL morning), low DHEA-S (<100 mcg/dL), and low free T3 (<3.0 pg/mL), often with normal TSH [3].
This pattern predicts specific symptoms. People with this combination report 60% more fatigue, 45% worse mood scores, and 30% longer recovery times from exercise compared to those with balanced hormones. The changes may appear within 4-8 weeks of ongoing stress, and persist as long as the underlying drivers aren't addressed.
The cortisol rhythm gives you even more information. A healthy pattern shows morning cortisol at 12-18 mcg/dL, dropping to 3-5 mcg/dL by evening. A flat or inverted cortisol curve, combined with low DHEA-S and free T3, signals that your stress system is not just overactive, but may be burning out. Reading these markers as a pattern, not in isolation, is the best path toward understanding what's really happening in your body.
Why This Matters Post-Menopause: The Adrenal Glands Step Up
After menopause, your ovaries largely stop making estrogen and progesterone. Your adrenal glands, which also produce DHEA, become your main source of these sex hormone precursors. But if your HPA axis is under chronic stress, your adrenal glands may shift even more of their resources toward making cortisol, leaving less for DHEA and downstream hormones. This is especially important for postmenopausal women, whose hormonal reserves are already reduced.
Standard DHEA-S ranges do not always reflect the needs of women after menopause. A level below 100 mcg/dL is common in this group, but research and clinical experience suggest that maintaining DHEA-S in the 100–200 mcg/dL range can help preserve mood, energy, and libido. When stress is high and DHEA-S is suppressed, postmenopausal women may feel doubly depleted—losing both their ovarian and adrenal contributions to sex hormones. This can show up as severe fatigue, increased abdominal fat, sleep disturbance, hot flashes, and depressed mood.
Recognizing this pattern makes stress management a hormonal health issue—not just a matter of feeling better day-to-day. If you are postmenopausal and see this pattern in your labs, it’s a strong signal to prioritize interventions that lower chronic stress—for example, improving sleep, reducing inflammation, and considering adaptogenic supplements under medical guidance. This sets the stage for the next section: why these hormonal shifts also impact your brain health and cognitive function.
The Bottom Line: Hormones as an Interconnected Network
Your hormonal system is not a collection of independent dials. Instead, it’s a network where stress, thyroid, and sex hormones share resources and influence each other’s production. When the HPA axis is activated by chronic stress, your body may quietly turn down thyroid and sex hormone output—even if individual lab numbers look normal. This resource competition and signaling crosstalk means that interpreting your labs as a pattern gives you much more insight than any single value.
When you see high cortisol, low DHEA-S, low free T3, and a normal TSH, you’re looking at a classic chronic stress pattern. For postmenopausal women, this pattern can be especially draining, since the adrenal glands are now the main source of sex hormone precursors. Research suggests that managing stress and supporting adrenal health is as important as any medication for maintaining hormonal balance and overall vitality.
This understanding also forms the bridge to brain health. When the HPA axis diverts resources away from thyroid and sex hormones, it can also impact neurotransmitter production and cognitive function. The health of your hormonal network is the foundation for both your body and your mind—and reading these patterns is your most powerful tool for targeted, effective action.
Conclusions
Your hormones do not exist in silos. They are part of one interconnected network, managed by the HPA axis, that reallocates resources in response to stress. The key to understanding persistent symptoms is to read lab markers as patterns, not as isolated numbers. For women—especially postmenopausal women—chronic stress can lead to a predictable drop in thyroid and sex hormone activity, even when traditional labs appear normal. Focusing on the full hormonal pattern, and prioritizing stress management, offers the clearest path to restoring energy, mood, and resilience.
Most of the evidence linking stress, thyroid, and sex hormone suppression comes from observational and mechanistic studies, not large randomized trials. The 'pregnenolone steal' hypothesis remains debated, with some researchers arguing for a greater role of pituitary signaling suppression. Optimal reference ranges for hormones like DHEA-S and free T3 are still under discussion, especially for demographic groups like postmenopausal women. Individual responses can vary, and integrating these insights with your doctor’s guidance is essential. More research is needed to clarify how best to intervene and personalize approaches.
Track this in your stack
See how hpa axis relates to your health goals and monitor changes in your biomarkers over time.
