The omega-3 index as a status marker: what the proven blood response tells you that dose labels cannot
Why identical fish oil doses produce dramatically different blood levels—and why measuring your omega-3 index matters more than capsule milligrams
Imagine taking a daily fish oil capsule, expecting it to boost your heart, brain, and immune health—only to find your actual omega-3 status is wildly different from your partner, who takes the same dose.
The truth is, what ends up in your bloodstream is what matters, not what’s on the supplement label. In this episode, you’ll learn why the omega-3 index is the only way to know if you’re getting enough, how it links to real health outcomes, and what you can do to optimize your levels for lifelong protection.
- Omega-3 index
- A blood test measuring EPA and DHA as a percentage of total red blood cell fatty acids, with 8-12% considered optimal for cardiovascular health
- EPA (eicosapentaenoic acid)
- A long-chain omega-3 fatty acid found in fish oil that's particularly important for reducing inflammation and triglycerides
- DHA (docosahexaenoic acid)
- A long-chain omega-3 fatty acid crucial for brain function and found in high concentrations in neural tissue
- Plasma phospholipid levels
- The concentration of omega-3 fatty acids incorporated into cell membrane components in blood, reflecting recent intake and tissue status
- Triglycerides
- Triglycerides, the primary fat storage molecule in blood. elevated levels indicate metabolic dysfunction and increase cardiovascular risk.
- Meta-Analysis
- A statistical technique combining results from multiple studies to find overall patterns.
- Bile acid production
- Bile acids are substances made by the liver that help digest and absorb dietary fats in the intestine. Differences in bile acid production can affect how well omega-3 fatty acids are absorbed into the
Picture yourself at the breakfast table, unscrewing the cap on your fish oil bottle. Maybe you picked it up after hearing about omega-3’s benefits for your heart, your mind, or your immune system. You take the same capsule every morning, just like your friend or your partner. You both expect the same protection, the same boost.
But a few months later, you each get your omega-3 index tested. Your score is low, theirs is high. You’re both surprised—and maybe a little frustrated. How can two people, taking identical supplements, end up with such different results?
This is not just a curiosity. It’s a reality that plays out for millions of people who take omega-3 supplements. The amount printed on the bottle is only the starting point. What truly matters is the amount of EPA and DHA—those are the active omega-3s—that actually makes it into your blood and your cells.
The science is clear on this: health benefits track with the omega-3s in your body, not the number of milligrams you swallow. That disconnect between dose and outcome is why so many people feel let down by supplements, or wonder if they’re wasting money. But there’s a way to know exactly where you stand, and how to get the benefits you’re aiming for.
Let’s break down why this matters for you, and what you can do about it.
Omega-3 fatty acids are essential for nearly every system in your body. They’re especially critical for your heart, your brain, your immune system, and even your sleep quality. But what makes them so influential?
Start with your heart. EPA and DHA, the main omega-3s from fish oil, are incorporated into the membranes of your red blood cells and heart cells. This changes the way your cells communicate, how flexible your blood vessels are, and even helps stabilize the electrical rhythms of your heart. That’s why people with higher omega-3 levels have lower rates of sudden cardiac events, lower blood pressure, and improved cholesterol profiles.
Move to your brain, and the story gets even more interesting. DHA makes up a huge portion of the fats found in your brain’s gray matter. It’s a structural building block for your neurons, helping keep their connections fluid and responsive. When you have enough DHA, your brain cells communicate more efficiently. That translates to better memory, sharper focus, and a lower risk of cognitive decline as you age.
Omega-3s are also powerful anti-inflammatories. When they’re abundant in your cells, they get converted into molecules called resolvins and protectins. These molecules actually turn off inflammation once it’s done its job, preventing chronic, low-grade inflammation that damages tissues and accelerates aging. That’s why omega-3s are linked to lower C-reactive protein levels, reduced joint pain, and even fewer symptoms in conditions like rheumatoid arthritis.
And then there’s sleep. Omega-3s, especially DHA, help regulate melatonin production and the health of your cell membranes in the brain. That means getting enough can translate to deeper, more restorative sleep. It’s not just about falling asleep faster—it’s about giving your brain the chance to clear out toxins and reset for the next day.
But here’s the catch: how much benefit you get depends on how much EPA and DHA actually make it into your blood and your cells. Your body is not a machine; genetics, gut health, medications, and even what you eat with your supplement can all shift the end result. That brings us to the real question: how can you know if your omega-3s are working for you?
If you’ve ever wondered whether your daily fish oil is doing anything, the omega-3 index gives you the answer. This is a simple blood test that measures the percentage of EPA and DHA in your red blood cell membranes. It reflects your true omega-3 status, not just what you’ve been swallowing.
Here’s how it works. When you take in omega-3s—whether from fish, krill oil, or algae—they get absorbed in your gut and then transported through your blood. Some get packed into your red blood cells, where they stay for two to three months. The omega-3 index tells you what percent of your total red blood cell fats are made up of EPA and DHA. This matters because it’s a direct marker of the long-term omega-3 levels in your tissues, not just a snapshot of what you ate last night.
What’s the target? The best evidence, especially for heart health, points to an optimal omega-3 index of eight to twelve percent. That’s the range associated with the lowest risk for sudden cardiac death and the greatest cardiovascular protection. Falling below four percent puts you at higher risk for heart problems, and unfortunately, most people in Western countries land somewhere between four and six percent.
Why does this range matter? In studies that tracked health outcomes, people who maintained an omega-3 index in the optimal zone had fewer cardiovascular events, lower triglycerides, and better cognitive outcomes as they aged. It’s not just about being above the minimum. Staying in the sweet spot means you’re getting the full protective effect.
What about other markers? Plasma omega-3 levels, which some labs measure, swing up and down quickly based on diet and recent meals. The omega-3 index is more reliable because it shows your average status over a couple of months, not just a single day.
This is why the omega-3 index is becoming the gold standard for measuring your true omega-3 status. It’s actionable knowledge. If your index is below eight percent, you know you need to make changes—either increasing your dose, changing your supplement, or tweaking your diet. And if you’re in range, you can be confident you’re getting the benefits that matter.
Here’s a reality check. The number of milligrams on your fish oil bottle is not a guarantee. Two people can take identical doses and end up with omega-3 indexes that are miles apart.
Why does this happen? The answer lies in how your body absorbs and processes these fats. Genetics play a big role. Some people have variations in genes that control how efficiently they absorb and convert omega-3s. Your gut health matters, too. If your gut lining isn’t healthy, or if you don’t make enough bile acids to digest fats properly, you might absorb less from each capsule. What you eat at the same time also changes things—taking omega-3s with a fat-containing meal can double or even triple absorption.
A major systematic review of randomized controlled trials showed that while higher supplement doses usually give higher blood levels, the relationship is far from perfect. Some people reach the optimal omega-3 index with a low dose, while others need much more. One person might hit eight percent with a thousand milligrams a day; another might need two thousand or more.
Food sources matter as well. Omega-3s from fatty fish are typically more bioavailable than those from plant sources, since the body can use them directly without conversion. Age, sex, baseline omega-3 status, and even medications like statins or certain diabetes drugs can all shift absorption and metabolism.
What does this mean for you? The only way to know if your dose is enough is to measure your omega-3 index. If you’re below target, you may need to adjust your supplement or your diet. If you’re in range, you know your current approach is working. This is the key lesson from the research: health benefits track with achieved blood levels, not with the number printed on a bottle. That brings us to what the evidence says about specific health outcomes.
Let’s get specific about why hitting the right omega-3 index matters for your health. The strongest evidence connects your blood EPA and DHA levels with lower triglycerides, reduced inflammation, and protection for your brain as you age.
Start with triglycerides. High triglycerides are a major cardiovascular risk factor. Meta-analyses show that omega-3s lower triglycerides in a dose-dependent fashion, but only when your blood levels go up. In a comprehensive review, people who achieved higher plasma EPA and DHA saw the greatest drops in triglycerides—sometimes up to twenty percent or more. This effect is especially strong in people who start with high triglycerides or metabolic syndrome. What does that mean for you? If you have elevated triglycerides, reaching an omega-3 index of eight percent or higher can be a game-changer for your heart health.
Now, inflammation. Chronic, low-grade inflammation underlies many diseases, from heart disease to type 2 diabetes to autoimmune conditions. C-reactive protein, or CRP, is a key blood marker for inflammation. A dose-response meta-analysis found that people with higher omega-3 blood concentrations had the most consistent reductions in CRP, especially if they already had high baseline inflammation or metabolic issues. This wasn’t just about the dose taken—benefits tracked with how much omega-3 made it into the blood.
What about your brain? Cognitive function studies show a similar pattern. The best results come when participants achieve higher blood DHA. A systematic review found cognitive improvements—like better memory and slower decline—were strongest in older adults with mild cognitive changes who got their DHA blood levels up. In younger, healthy adults, the effect is smaller, but maintaining a high omega-3 index is still linked to long-term brain health and resilience.
The takeaway? Whether your goal is heart health, taming inflammation, or keeping your mind sharp, the omega-3 index gives you the most reliable window into whether your efforts are paying off. Next, let’s talk about how to move your numbers in the right direction.
If your omega-3 index is below eight percent—or if you want to be sure you’re getting the full benefits—here’s how you can take action, backed by the strongest evidence.
First, choose a high-quality omega-3 supplement. Look for products that specify the actual amount of EPA and DHA per capsule, not just “fish oil.” Aim for a combined dose of fifteen hundred to two thousand milligrams of EPA plus DHA per day for most adults seeking heart, brain, and immune benefits. Some people may need more, especially if their starting omega-3 index is low or if they have higher cardiovascular risk. Algae-based omega-3s are a good option if you avoid fish products—the key is the EPA and DHA content, not the source.
Take your omega-3s with a meal that contains fat. This one change can double or triple your absorption. If you take your supplement with just water or on an empty stomach, you’re likely wasting much of the dose.
Consistency is crucial. Because the omega-3 index reflects your average levels over two to three months, it takes at least that long to see changes in your numbers. Retest after three months to see if you’ve reached your goal. If not, increase your dose or check with your healthcare provider for personalized adjustments.
If you prefer food sources, focus on two to three servings of fatty fish per week. Salmon, sardines, mackerel, anchovies, and herring are top choices. Plant-based sources like flaxseed or chia provide ALA, but your body converts only a tiny fraction to EPA and DHA, so they’re not a substitute for marine omega-3s if you’re aiming for a specific index target.
Monitor your other lifestyle factors, too. High alcohol intake, smoking, and some medications can lower your omega-3 status. If you have gut issues that affect fat absorption, you may need a higher dose or a different supplement form, such as emulsified omega-3s, which are easier to absorb for some people.
Finally, remember that omega-3 supplementation is safe for most people, but if you have a bleeding disorder, are on blood thinners, or take high-dose aspirin, check with your doctor before starting high doses. Now, let’s expand beyond supplements and look at the lifestyle levers that can move your omega-3 index and your health even further.
Supplements are just one part of the story. Your diet, exercise habits, and sleep patterns all shape your omega-3 status and how your body uses these fats.
Start with food. The Mediterranean diet, which is rich in fatty fish, olive oil, nuts, and plenty of colorful vegetables, is consistently linked to higher omega-3 indexes and better cardiovascular and brain outcomes. Swapping red meat or processed foods for seafood just twice a week can raise your omega-3 index by one to two percent over several months. Small, oily fish like sardines and anchovies are especially high in EPA and DHA, and they’re less likely to be contaminated with mercury. If you’re plant-based, focus on walnuts, flaxseed, and chia, but remember you may need an algae-based supplement to hit your blood target.
Exercise also matters. Regular aerobic activity improves blood flow, reduces inflammation, and helps your body incorporate omega-3s into cell membranes. Even brisk walking for thirty minutes most days of the week supports cardiovascular health and can help lower triglycerides in synergy with omega-3s.
Sleep is often overlooked, but it plays a real role. Poor sleep increases inflammation and stresses your cardiovascular system, which can blunt some of the benefits of omega-3s. Prioritize seven to eight hours of quality sleep, aiming for consistent bed and wake times. If you struggle with sleep, omega-3 supplementation may help by supporting melatonin production and reducing nighttime inflammation—but you also need to address sleep hygiene basics.
Other lifestyle factors matter, too. Chronic stress, high alcohol intake, and smoking can all reduce your omega-3 index or interfere with its protective effects. Managing stress with mindfulness, yoga, or daily movement helps your body get the most from your omega-3 efforts.
By combining targeted supplementation, smart food choices, movement, and restorative sleep, you set the stage for optimal omega-3 status and lasting health benefits. But how do you know if things are slipping? That’s where early warning signs come in.
You might wonder, how would you know if your omega-3 status is too low—especially before a blood test? While symptoms can be subtle, there are clues your body may send.
If you notice your skin and hair are dry and brittle, or wounds heal more slowly than usual, these can be early signs of low omega-3s. Trouble with memory or focus, especially as you age, can also be a signal that your brain needs more DHA. Frequent colds, higher-than-usual joint pain, or lingering low mood may be linked to low omega-3 status, since these fats help regulate inflammation and neurotransmitter balance.
If you have a family or personal history of heart disease, high triglycerides, or metabolic syndrome, you’re automatically at higher risk of deficiency. People following restrictive diets, especially vegan or very low-fat plans, should be especially vigilant, since plant-based sources alone are unlikely to provide enough EPA and DHA.
Certain medications, like cholesterol-lowering drugs, can interfere with fat metabolism, which may impact your omega-3 status. Digestive conditions that limit fat absorption—like celiac disease, Crohn’s, or a history of gallbladder removal—also put you at risk.
If you’re experiencing any of these patterns—or if you simply want to optimize your health—the next step is clear. Get your omega-3 index tested. This gives you a baseline to work from. If you’re below eight percent, take action with the protocol outlined earlier, then recheck after three months.
Don’t wait for obvious symptoms. By the time cardiovascular or cognitive problems show up, underlying deficiencies may have been smoldering for years. Testing and acting early puts you in control. That brings us to the final takeaway—the bottom line for your health and your future.
The promise of omega-3s is real, but only if you get enough where it counts—in your cells, not just your supplement bottle. The omega-3 index is your personal dashboard for heart, brain, immune, and sleep health. It tells you what’s working, what needs adjusting, and how well your interventions are protecting you.
The science is clear: health outcomes follow your blood EPA and DHA, not the milligrams you swallow. The right dose for you is the one that gets your omega-3 index into the eight to twelve percent sweet spot. For most people, that means two to three servings of fatty fish per week, or a supplement providing fifteen hundred to two thousand milligrams of combined EPA and DHA daily, always taken with food. But individual needs vary, and the only way to know is to test.
By tracking your omega-3 index and making evidence-based changes, you give yourself the best shot at cardiovascular protection, a resilient brain, strong immunity, and better sleep as you age. Don’t settle for guessing—measure, act, and retest. The benefits are too important to leave to chance. The best time to start optimizing your omega-3 status is now—and with the right approach, you can see and feel the difference in a matter of months.
Your Omega-3 Supplement May Be Doing Nothing: The Omega-3 Index Is the Only Way to Know
Why taking fish oil and having optimal omega-3 status are completely different things
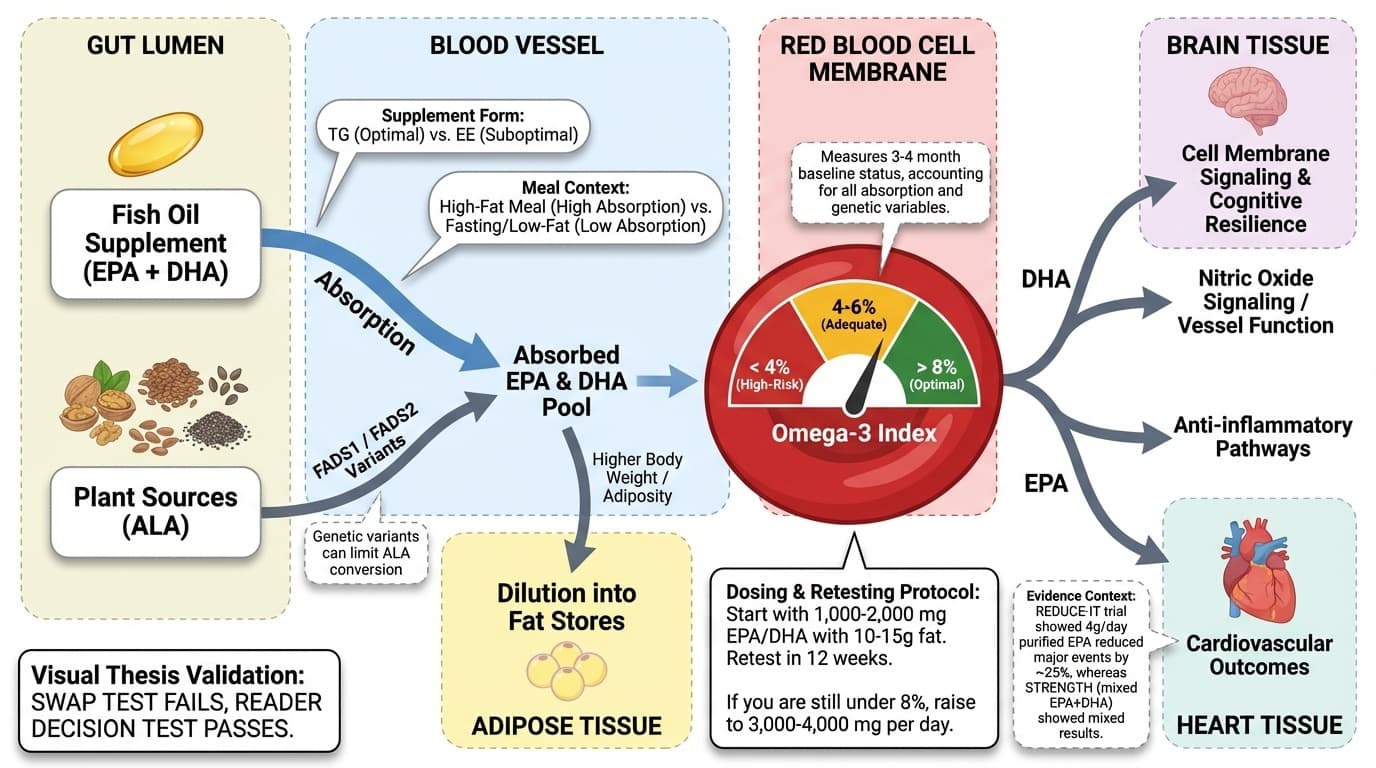
Diagram glossary
- ALA:
- A plant-based omega-3 fatty acid found in foods like flax or chia seeds.
- EPA/DHA:
- Marine omega-3 fatty acids that impact heart health and determine your Omega-3 Index.
- FADS1/FADS2:
- Genes whose variants can limit the conversion of plant ALA into EPA and DHA.
Conclusions
The omega-3 index represents a shift from dose-based to blood-level-based evaluation of omega-3 status. Rather than relying solely on fish oil dose, blood testing can reveal actual omega-3 status. The evidence shows that health outcomes—particularly triglyceride reduction and cardiovascular benefits—correlate with achieved blood levels rather than supplement doses. However, most research establishing optimal omega-3 index ranges has focused on cardiovascular outcomes, with less data available for other health goals.
Most omega-3 index research has focused on cardiovascular outcomes, with less data available for optimal ranges related to cognitive function, athletic performance, or general wellness [4]. The 8-12% target range comes primarily from cardiovascular studies and may not apply to all health goals [4]. Additionally, while the omega-3 index is a validated biomarker, the relationship between omega-3 index changes and long-term health outcomes requires more longitudinal research to fully establish causality [1][5].
Track this in your stack
See how omega 3 fatty acids relates to your health goals and monitor changes in your biomarkers over time.
Sources (6)
This article informs how supplementation moves 3 markers.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
% EPA + DHA in red-blood-cell membranes. Target >= 8% for cognitive protection; most US adults sit at 4-5%.
High-sensitivity C-reactive protein. > 3 mg/L associated with chronic systemic inflammation affecting the brain and vasculature.
Apolipoprotein B — particle count of atherogenic lipoproteins. Levels > 80 mg/dL associated with cardiovascular event risk independent of LDL-C.
