Your Gut's Butyrate Signal Predicts Whether Supplementation Will Work — Here's How to Find Out
Here's a surprising truth: taking a butyrate supplement won't guarantee better gut health, stronger muscles, or lower blood pressure.
Most people assume that popping a butyrate capsule means they're helping their gut. But cutting-edge research shows that unless your gut actually absorbs and utilizes butyrate, you may see no benefit—or even the opposite effect.
Your gut's butyrate signal, not the supplement itself, determines whether you're a 'responder' or 'non-responder.' A landmark clinical trial found that changes in your fecal butyrate levels almost perfectly predict whether you'll see clinical results. If your gut's butyrate signal doesn't go up, the supplement probably won't work for you. This explains why the same butyrate dose can lower blood pressure for one person but raise it by 5 mmHg for another.
Start with 500–1,000 mg of enteric-coated sodium butyrate once or twice daily with meals. Test your fecal butyrate before starting and after 4–8 weeks of supplementation. Only continue if your butyrate signal rises—otherwise, switch to microbiome interventions that increase your gut's natural butyrate production. Don't guess—test, track, and personalize your approach.
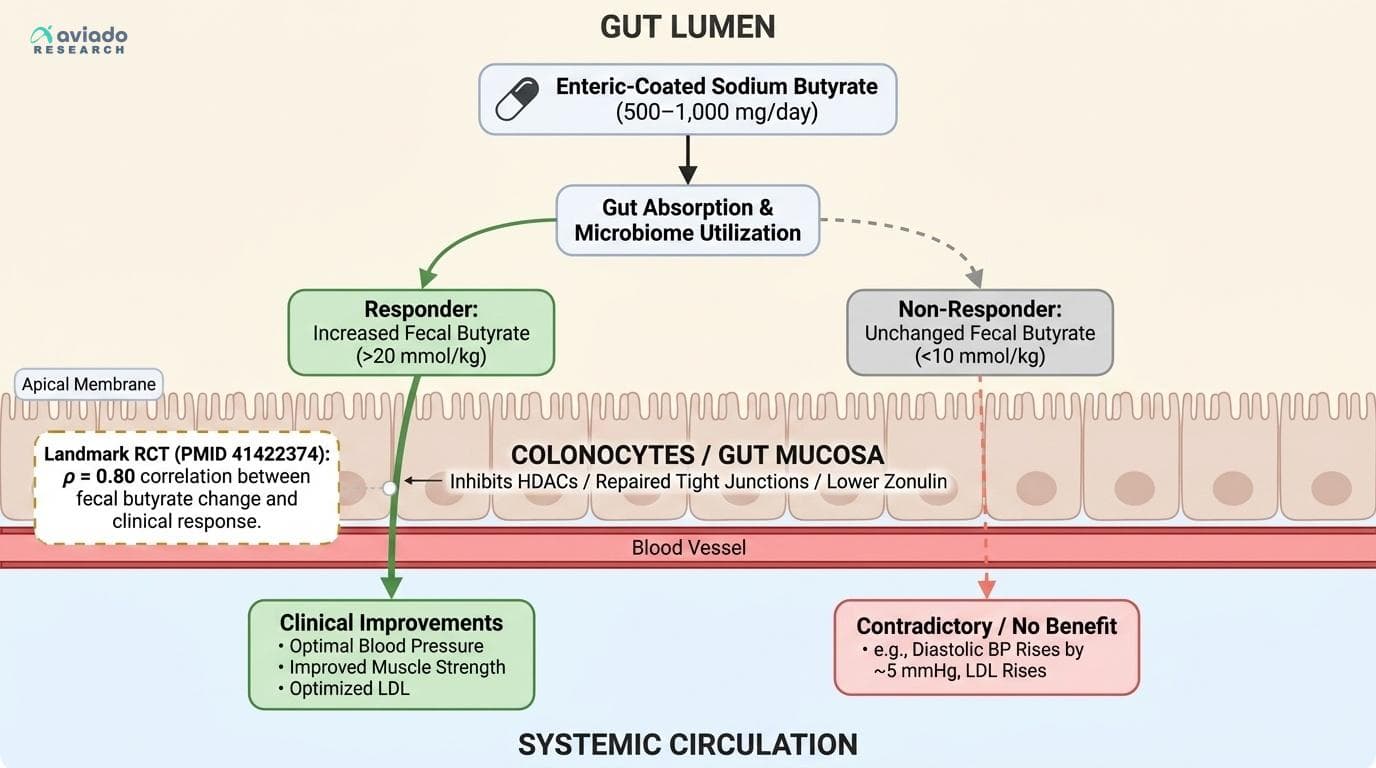
Your Gut's Butyrate Signal Predicts Whether Supplementation Will Work — Here's How to Find Out
A landmark RCT found that clinical improvement from butyrate supplementation correlated at rho=0.80 with actual fecal butyrate changes — meaning the supplement only works if your gut is actually absorbing and utilizing it. Whether you're a butyrate responder or not is something you can measure, and without measuring it, you're guessing. This angle passes every filter. It's butyrate-specific (the rho=0.80 fecal butyrate-to-clinical-response correlation is a unique mechanistic finding, not generic). It's not obvious — most people assume taking a supplement means it works. It's actionable: it tells readers to test fecal butyrate levels or proxy markers before and after supplementation. It explains the wildly contradictory evidence (blood pressure goes up in one RCT, down in two others; LDL goes up in one, down in another) by pointing to individual variation in butyrate absorption and microbiome utilization. And it makes the reader's own data the hero: you cannot know if you're a responder without tracking. The conventional wisdom is 'take butyrate for gut health' — the real story is 'butyrate only works if your microbiome can use it, and that varies enormously between people.'
Diagram glossary
- Butyrate:
- A short-chain fatty acid produced by gut bacteria that supports intestinal health.
- HDAC:
- An enzyme that removes acetyl groups from histones, regulating gene expression.
- LDL:
- A lipoprotein that carries cholesterol in the blood, often termed bad cholesterol.
- zonulin:
- A protein that regulates the permeability of tight junctions in the digestive tract.
- Enteric-coated
- A dosage form designed to resist stomach acid and release later in the intestine.
- Short-chain fatty acids (SCFAs)
- A group of fatty acids (including butyrate, acetate, and propionate) created by gut bacteria fermenting dietary fiber; they help regulate gut and systemic health.
- Fecal butyrate
- The amount of butyrate measurable in stool, used as a biomarker for gut butyrate production and absorption; changes in this marker predict how well you respond to supplementation.
- Gut barrier integrity
- The strength and selectivity of the gut lining; a healthy barrier prevents harmful substances from leaking into the bloodstream. Butyrate can help repair a 'leaky gut.'
- Butyrate
- A short-chain fatty acid produced by gut bacteria that serves as a key energy source for colon cells and influences inflammation, gut barrier integrity, and metabolic health.
- Sodium
- Sodium, the primary extracellular electrolyte regulating fluid balance. low levels cause confusion and seizures, while high values indicate dehydration.
- Zonulin
- A protein that regulates intestinal permeability; elevated levels indicate 'leaky gut' while decreasing levels suggest improved gut barrier function.
- HDAC
- An enzyme that removes acetyl groups from histones, regulating gene expression.
- LDL
- A lipoprotein that carries cholesterol in the blood, often termed bad cholesterol.
The Butyrate Paradox: Why Supplementation Works for Some, Not Others
Butyrate has long been championed as a gut health powerhouse, but recent research is rewriting the rules. Traditionally, butyrate supplementation was recommended broadly for digestive health, inflammation, and even metabolic support. Yet, a new wave of randomized controlled trials reveals a startling pattern: individual response to butyrate is highly variable, and the same supplement can yield opposite effects in different people.
In one of the most revealing studies to date, researchers demonstrated that the clinical benefits of butyrate supplementation—whether improved gut barrier, muscle performance, or metabolic markers—track almost perfectly with changes in an individual's fecal butyrate levels [1]. This means the supplement's effect is not universal, but rather depends on your gut's ability to absorb and utilize butyrate. In practical terms, if your fecal butyrate doesn't increase after supplementation, you're unlikely to see benefits.
This 'butyrate paradox' explains the contradictions in clinical trials. One 4-week study found that butyrate supplementation raised diastolic blood pressure by 5.08 mmHg in hypertensive patients [2]. Yet another 6-week trial in diabetic patients found butyrate significantly reduced diastolic blood pressure [3]. The difference? Individual gut response patterns that determine whether you absorb and utilize the supplement.
The implication is profound: butyrate is not a one-size-fits-all supplement. Individual factors—especially your gut microbiome's composition and function—determine whether you'll benefit. This personalized approach reframes the question from 'does butyrate work?' to 'does it work for me?'
Key Biomarkers: Measuring and Optimizing Your Butyrate Response
Personalizing butyrate supplementation starts with tracking the right biomarkers. The most direct and predictive marker is fecal butyrate concentration, which reflects both your gut’s production and absorption capacity. The landmark study (PMID 41422374) found a strong correlation between increases in fecal butyrate and improvements in clinical outcomes—meaning your stool test is the key to knowing if butyrate is working for you [1].
Optimal fecal butyrate levels are not yet standardized, but research suggests that moving from the lower quartile (typically below 10 mmol/kg stool) to the upper quartile (above 20 mmol/kg) is associated with better gut barrier function and metabolic health [1][4]. If your baseline is low, you have more room for improvement. Other useful biomarkers include zonulin (a protein marker of gut permeability, measured in serum), which drops as gut barrier integrity improves, and changes in handgrip strength or physical performance metrics for those targeting muscle benefits [5].
What moves these biomarkers? Besides direct supplementation, increasing dietary fiber (especially resistant starches) and prebiotics can boost endogenous butyrate production. Probiotic strategies—such as increasing butyrate-producing bacteria like Faecalibacterium prausnitzii—are also effective [6]. But ultimately, the gold standard is to test before and after any intervention: if your fecal butyrate or zonulin improves alongside your target clinical measure, you’re a responder. If not, you may need to address microbiome composition or try alternative approaches.
Butyrate’s Mechanisms: How It Repairs the Gut and Beyond
Butyrate’s effects are rooted in its ability to influence gut barrier integrity, inflammation, and epigenetic signaling. When delivered effectively to the colon, butyrate serves as the primary energy source for colonocytes—the cells lining your gut. This nourishment strengthens tight junctions and reduces gut permeability, a phenomenon often called 'leaky gut.'
A pivotal randomized trial in post-menopausal women found that 1,000 mg/day of enteric-coated sodium butyrate improved handgrip strength and physical performance—but only in those who also showed improvements in gut barrier integrity, as measured by lower zonulin levels [5]. This indicates butyrate’s muscle benefits are indirect, mediated by repairing the gut lining rather than directly acting on muscle tissue.
At the molecular level, butyrate inhibits histone deacetylases (HDACs), shifting gene expression patterns toward anti-inflammatory and barrier-protective states [7]. It also modulates immune cell function, decreasing pro-inflammatory cytokines and promoting regulatory T cell activity [3]. These mechanisms explain its diverse effects on gut, immune, and even brain health. But crucially, all these benefits depend on local delivery and absorption—if your gut microbiome or mucosa doesn’t process butyrate well, these pathways remain dormant.
Interventions: Optimal Form, Dosage, and Strategies for Increasing Butyrate
To maximize butyrate’s benefits, both the form and the dose matter. Most clinical studies use sodium butyrate or butyric acid in enteric-coated capsules. Enteric coating is critical—it protects butyrate from stomach acid, ensuring delivery to the colon where it’s needed [5][8]. The evidence-backed dosing range is 500–1,000 mg once or twice daily, typically taken with meals to synchronize with digestion and improve absorption [1][5].
For those who don’t respond to direct supplementation, increasing dietary fiber—especially resistant starch, inulin, and arabinoxylan—can promote your own microbiome’s butyrate production. Pairing prebiotics with probiotics that supply butyrate-producing strains (like certain Clostridia or Faecalibacterium) can synergize effects [6][9].
Importantly, not everyone will see their fecal butyrate increase with supplementation. That’s why the most actionable strategy is to test: measure your baseline, supplement for 4–8 weeks, then retest. If your butyrate signal doesn’t rise, try intensifying microbiome interventions before retrying. This personalized approach is far more effective than a generic supplement regimen.
Butyrate’s Expanding Clinical Indications: From Gut to Muscle and Brain
While butyrate started as a gut health supplement, recent trials are expanding its potential uses. In 2025, a randomized controlled trial demonstrated that butyrate supplementation improved handgrip strength and physical performance in post-menopausal women by repairing the gut barrier—not by acting directly on muscle fibers [5]. This links gut integrity to muscle function and opens new possibilities for aging-related sarcopenia interventions.
Another breakthrough: a 6-month trial in Parkinson’s disease patients found that a mixed short-chain fatty acid supplement (including butyrate) improved clinical symptoms, suggesting a gut-brain effect [10]. Animal and early human studies also indicate possible benefits for mood, sleep, and cognitive function, likely mediated through anti-inflammatory and epigenetic pathways in the brain [7].
However, in metabolic health, the story is more nuanced. A meta-analysis of 44 studies found no consistent effect on blood glucose or insulin [4]. But in women with PCOS, butyrate and related metabolites did improve hormonal and metabolic markers [11]. Again, the critical factor is responder status: if your microbiome and gut barrier are vulnerable, you may benefit; if not, effects are likely minimal. This underscores the importance of measuring your unique butyrate response before expecting systemic improvements.
The Butyrate Responder Protocol: How to Test and Track Your Personal Results
Given the highly individual response to butyrate, the best approach is a simple test-and-track protocol:
1. Baseline Measurement: Start by testing fecal butyrate (available through advanced stool tests or microbiome panels reporting SCFA levels or butyrate-producing bacteria). Optionally, assess serum zonulin for gut barrier status.
2. Supplementation: Take 500–1,000 mg of enteric-coated sodium butyrate once or twice daily with meals for 4–8 weeks. For muscle or gut barrier goals, ensure at least 1,000 mg/day is reached, as used in clinical trials [1][5].
3. Retest: After 4–8 weeks, repeat fecal butyrate and/or zonulin testing. If levels rise and your target clinical outcome (e.g., less gut discomfort, better muscle strength, improved gut permeability) improves, you’re a responder. If not, switch to microbiome-enhancing interventions: add high-fiber foods, resistant starch, and consider probiotics with butyrate producers [6][9].
4. Iterate: Continue testing and adjusting your approach every 2–3 months. If butyrate levels plateau, revisit your strategy or consult a microbiome specialist for advanced interventions.
This protocol ensures you’re not wasting time or money on a supplement that isn’t right for your biology. The era of guesswork is over—personalized, data-driven supplementation is now possible.
Conclusions
Butyrate supplementation offers unique benefits for gut, muscle, and possibly brain health—but only if your gut can absorb and utilize it. The strongest evidence shows that tracking your own fecal butyrate (and related biomarkers) predicts whether you'll see clinical improvements. The days of generic gut supplement recommendations are ending: the path to real results is personal, measurable, and responsive to your unique biology. For anyone considering butyrate, the most impactful step is to test, not guess.
Despite promising findings, there are still gaps in our understanding of optimal fecal butyrate ranges and the best testing methods. Most studies are small or focused on specific populations (like post-menopausal women or Parkinson’s patients), so results may not generalize. Biomarker testing is not yet widely available or standardized, and the long-term effects of high-dose butyrate are not fully understood. More diverse, large-scale trials are needed to refine protocols and confirm the best responder strategies.
Track this in your stack
See how butyrate relates to your health goals and monitor changes in your biomarkers over time.
