Zinc's Benefits Are Real — But Only If You're Actually Deficient
Meta-analyses reveal zinc supplementation dramatically improves metabolic markers in diabetics while potentially lowering HDL in healthy people
The surprising thing about zinc is this. It can help a lot. Or it can do nothing. Many people take zinc “just in case.” That can backfire in healthy people.
Here is the simple rule for you. Zinc helps most when your body is low. It also helps more when your labs look off. This includes high blood sugar or high inflammation. If your labs look good, zinc may not help.
Use clear doses. Try 15–30 mg elemental zinc daily. Stay in that range for 8–12 weeks. Recheck your HDL and hs-CRP at 12 weeks. Avoid going above 40 mg per day long term.
- Type 2 diabetes
- A condition where blood sugar stays high due to insulin resistance and/or low insulin output.
- Zinc forms (gluconate, sulfate, picolinate, bisglycinate, oxide)
- Different chemical forms that can change absorption and stomach tolerance. The label should state the form.
- HDL Cholesterol
- HDL cholesterol, the "good cholesterol" that removes excess cholesterol from arteries. higher levels are cardioprotective.
- HOMA-IR (calc)
- Insulin resistance by combining fasting glucose and insulin levels.
- Glucose
- Blood sugar level, the primary energy source for cells. Fasting glucose is normal, prediabetes, ≥126 suggests diabetes.
- C-Reactive Protein (cardiac)
- High-sensitivity C-reactive protein, a liver-produced acute-phase reactant. Independent predictor of heart attack and stroke.
- High-sensitivity C-reactive protein (hs-CRP)
- A more precise version of the standard C-reactive protein test that can detect very low levels of inflammation in the blood. It is commonly used to assess cardiovascular risk, even when inflammation i
- bisglycinate
- A highly absorbable compound where a mineral is bound to two glycine molecules.
- CRP
- A blood protein produced by the liver that indicates systemic inflammation.
- cytokine
- A small protein involved in cell signaling and immune system regulation.
The Population Split: Why Zinc Works for Some and Not Others
Recent meta-analyses do not show one “zinc effect.” They show a split. The same dose can move markers in opposite directions.
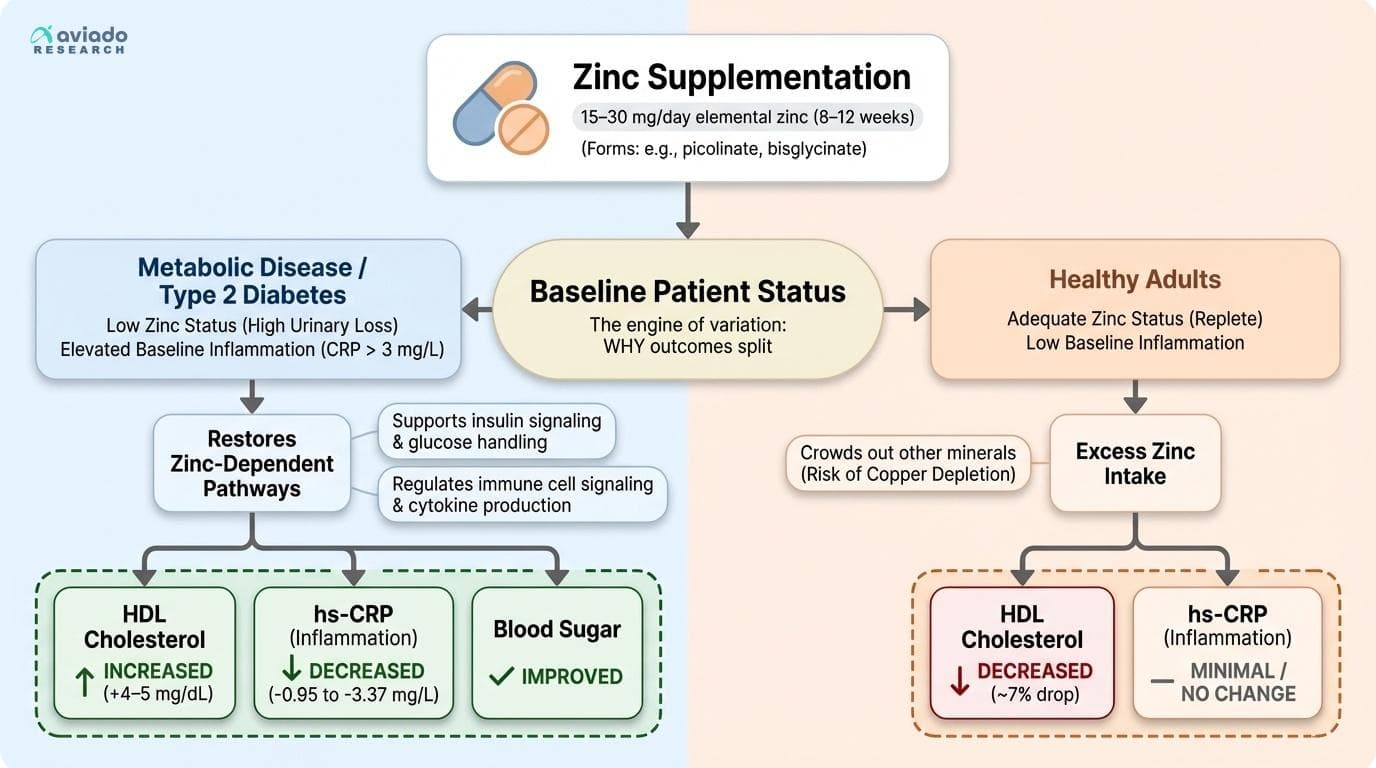
In healthy adults, a large meta-analysis (33 interventions; >14,000 people) found zinc lowered HDL cholesterol by about 7% [1]. In contrast, meta-analyses in people with type 2 diabetes found zinc raised HDL by about 4–5 mg/dL [3].
This split shows up in inflammation too. In metabolically stressed groups, zinc reliably lowers CRP. One dose-response meta-analysis reported a 3.37 mg/L CRP drop in adults overall, with larger effects in higher-risk subgroups [2]. Healthy groups with low baseline inflammation often show smaller or no changes.
A practical explanation fits the pattern. Zinc supports insulin signaling and glucose handling. People with type 2 diabetes can also lose more zinc in urine. If your zinc status is low, adding zinc can improve zinc-dependent pathways. If your zinc status is already solid, extra zinc may crowd out other minerals and shift lipids in the wrong direction.
The Inflammation Response: Consistent Benefits in the Right Population
Zinc's anti-inflammatory effects show the same population-specificity pattern, but with more consistent evidence across studies. Multiple meta-analyses have documented significant reductions in inflammatory markers, particularly C-reactive protein, in people with elevated baseline inflammation.
A meta-analysis of 35 randomized controlled trials involving nearly 2,000 participants found zinc supplementation reduced high-sensitivity CRP by 0.95 mg/L [4]. Another analysis of 32 placebo-controlled trials showed even larger reductions of 1.31 mg/L in hs-CRP [5]. The effect appears dose-dependent and most pronounced in individuals with baseline CRP levels above 3 mg/L — the threshold considered high cardiovascular risk.
The anti-inflammatory mechanism involves zinc's role in regulating immune cell signaling and cytokine production. Zinc deficiency leads to overactivation of inflammatory pathways, while adequate zinc status helps maintain immune balance [6]. This explains why people with chronic inflammatory conditions or metabolic disease see the most dramatic improvements, while those with normal inflammatory markers may see minimal changes.
Interestingly, the inflammation benefits appear more universal than the cholesterol effects. Even some healthy individuals with elevated stress or subclinical inflammation may benefit from zinc's immune-modulating properties, though the effects are generally smaller than those seen in people with overt metabolic dysfunction.
Dosing and Forms: What the Meta-Analyses Actually Used
Most of the metabolic trials used moderate doses, not mega-doses. Across meta-analyses, common intakes were 15–30 mg per day of elemental zinc, often as zinc sulfate or zinc gluconate, for about 8–12 weeks [2][3][4].
Some forms may absorb better. Zinc picolinate and zinc bisglycinate often show higher bioavailability than zinc oxide in comparative work [7]. But in real-world trials, baseline status likely matters more than form.
More is not always better. Doses around 30–40 mg per day did not consistently outperform lower doses for metabolic outcomes and can raise the risk of copper depletion over time.
Takeaway for use: pick a form you tolerate, stay in the 15–30 mg/day range, and avoid stacking zinc with calcium or iron at the same time, since they can reduce zinc uptake.
The Diagnostic Problem: Why Zinc Status Is Hard to Measure
Zinc status is hard to pin down with one lab test. Serum zinc is the most common marker, but it reflects only a small pool and can look “normal” even when zinc-dependent functions are strained.
Zinc also works inside thousands of proteins and enzymes. That means “enough zinc” is partly about function, not just blood levels [8]. This helps explain why study results look mixed when trials do not confirm deficiency at baseline.
In practice, your best clues are often the markers you want to improve. If your fasting glucose, HbA1c, triglycerides, or hs-CRP are high, you are more likely to see a measurable response than someone with clean labs.
Alternative approaches (like red blood cell zinc or taste tests) exist, but they are not perfect. The most useful strategy is to track outcomes: repeat the same glucose, lipid, and inflammation markers after a defined zinc trial.
Zinc's Benefits Are Real — But Only If You're Actually Deficient
Meta-analyses reveal zinc supplementation dramatically improves metabolic markers in diabetics while potentially lowering HDL in healthy people
Diagram glossary
- bisglycinate:
- A highly absorbable compound where a mineral is bound to two glycine molecules.
- CRP:
- A blood protein produced by the liver that indicates systemic inflammation.
- cytokine:
- A small protein involved in cell signaling and immune system regulation.
- gluconate:
- A salt of gluconic acid commonly used to formulate mineral supplements like zinc.
- glucose:
- A simple sugar that serves as the primary energy source for the body's cells.
- HDL:
- High-density lipoprotein is a beneficial cholesterol that removes other forms of cholesterol from blood.
- insulin:
- A pancreatic hormone that regulates blood glucose levels by facilitating cellular uptake.
- picolinate:
- A derivative of picolinic acid used in supplements to enhance mineral absorption.
Conclusions
Zinc is not a “take it forever” supplement for everyone. The evidence points to a clear responder group: people with type 2 diabetes, metabolic syndrome features, or higher inflammation. In these groups, typical doses (15–30 mg elemental zinc daily for ~8–12 weeks) can improve HDL and lower CRP. In healthy people, the same doses can nudge HDL down without clear upside. The smart move is targeted zinc: use it when your markers suggest you may need it, then measure whether you actually respond.
Most zinc trials are short (often 8–16 weeks), so long-term effects are less certain. Many studies also lack strong baseline zinc assessment, and serum zinc can miss functional deficiency, making “who is deficient” hard to define. Populations vary widely (age, diet, inflammation level, diabetes control), which can drive different results across meta-analyses. Finally, higher-dose zinc can reduce copper status over time, and many trials did not fully track trace-mineral interactions.
Track this in your stack
See how zinc relates to your health goals and monitor changes in your biomarkers over time.
Sources (8)
This article informs how supplementation moves 2 markers.
Each biomarker page clusters supplements, ranges, and the evidence behind every score. Useful when you're starting from a number, not a goal.
3-month average blood glucose. Levels >= 5.7% associated with cognitive decline independent of diabetes diagnosis.
Apolipoprotein B — particle count of atherogenic lipoproteins. Levels > 80 mg/dL associated with cardiovascular event risk independent of LDL-C.
